Organizations increasingly recognize that employee mental health directly influences productivity, retention, and overall performance. Implementing effective strategies to improve mental health requires more than awareness campaigns or isolated interventions. It demands systematic approaches that integrate evidence-based practices into organizational culture, leadership behavior, and daily operations. For HR professionals and organizational leaders, understanding which strategies deliver measurable outcomes becomes essential when building sustainable workplace mental health programs that protect employees while advancing business objectives.
Understanding the Foundation of Workplace Mental Health
Mental health represents a state of wellbeing in which individuals realize their abilities, cope with normal life stresses, work productively, and contribute to their communities. This comprehensive understanding of mental health extends beyond the absence of illness to encompass psychological resilience, emotional regulation, and adaptive functioning.
In organizational contexts, mental health exists on a continuum. Employees experience varying levels of psychological wellbeing influenced by workplace factors, personal circumstances, and broader social determinants. Recognizing this spectrum allows leaders to implement strategies that support all employees, not just those experiencing clinical conditions.
Key workplace mental health indicators include:
- Employee engagement and motivation levels
- Absenteeism and presenteeism rates
- Conflict resolution effectiveness
- Innovation and creative output
- Turnover patterns and retention metrics
Research demonstrates that workplace factors contribute significantly to mental health outcomes. Current mental health statistics reveal the substantial impact of work-related stress, highlighting the urgent need for organizational intervention.
Developing Manager Capability Through Targeted Training
Frontline managers represent the most critical leverage point for workplace mental health interventions. Managers directly influence team culture, workload distribution, psychological safety, and access to support resources. Without adequate training, even well-intentioned managers may inadvertently create conditions that undermine employee wellbeing.

Effective manager training programs should address specific behavioral competencies rather than general awareness. Managers need practical skills in recognizing early warning signs, conducting supportive conversations, implementing reasonable adjustments, and navigating disclosure situations appropriately.
Essential Manager Training Components
| Training Element | Purpose | Expected Outcome |
|---|---|---|
| Mental health literacy | Build accurate understanding of conditions | Reduced stigma, appropriate responses |
| Conversation frameworks | Provide structured approaches to sensitive discussions | Increased manager confidence |
| Legal and ethical boundaries | Clarify manager role versus clinical support | Protected organization, supported employee |
| Reasonable adjustment processes | Enable practical workplace modifications | Improved retention, faster recovery |
| Trauma-informed principles | Create safety-oriented interactions | Enhanced psychological safety |
Programs offered through online mental health training platforms allow managers to develop these competencies flexibly while maintaining consistent quality standards across distributed teams.
Managers also require ongoing support beyond initial training. Peer learning networks, case consultation opportunities, and access to specialist advice ensure managers can navigate complex situations confidently. These strategies to improve mental health capabilities at the leadership level create cascading positive effects throughout organizational hierarchies.
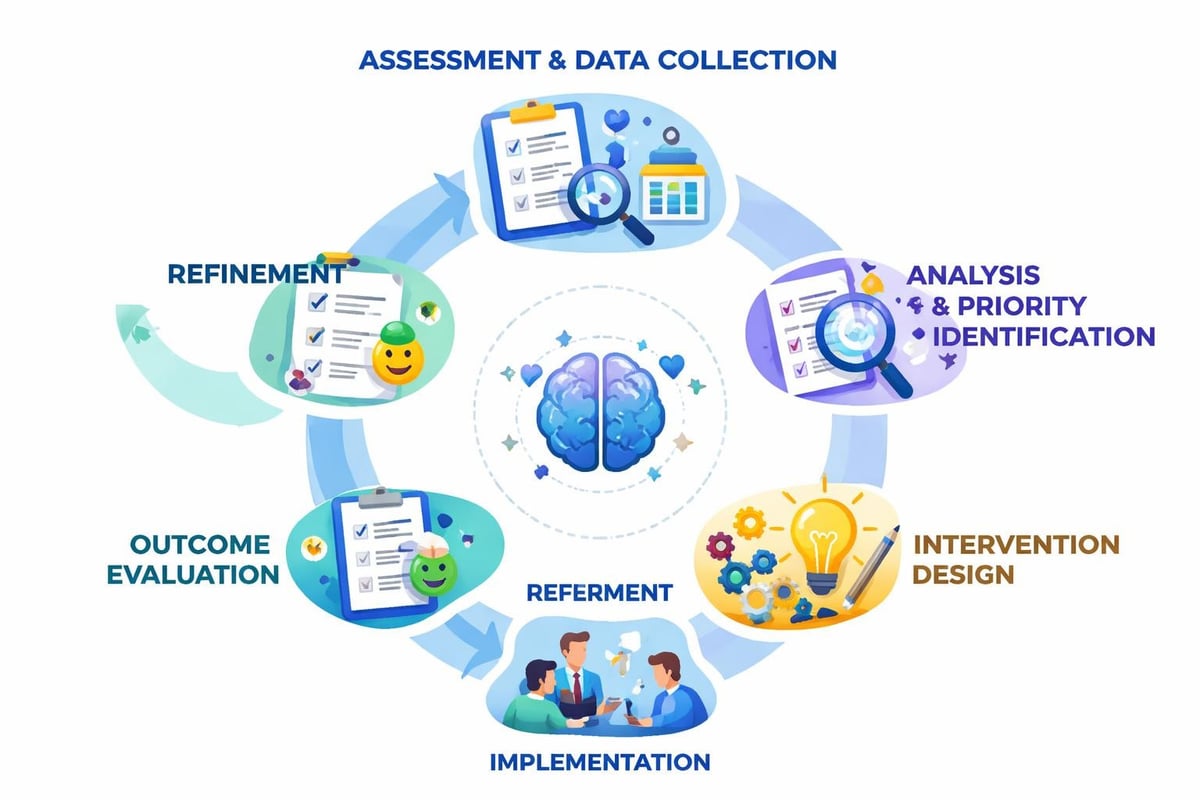
Implementing Systematic Wellbeing Assessment
Organizations cannot improve what they do not measure. Systematic wellbeing assessment provides the data foundation for targeted intervention, resource allocation, and program evaluation. Yet many organizations approach assessment inconsistently or focus on metrics that fail to capture meaningful psychological factors.
Comprehensive assessment strategies examine multiple dimensions:
- Organizational factors: Work design, role clarity, resource adequacy, change management processes
- Team dynamics: Psychological safety, inclusion, conflict patterns, support availability
- Individual experiences: Stress levels, coping capacity, work-life integration, meaning and purpose
- Outcome indicators: Engagement, burnout symptoms, help-seeking behaviors, performance metrics
Effective assessment combines quantitative surveys with qualitative insights gathered through focus groups, manager observations, and confidential individual feedback mechanisms. This mixed-method approach captures both prevalence data and contextual understanding necessary for designing appropriate interventions.
Assessment Implementation Framework
Regular assessment cycles (quarterly or biannually) allow organizations to identify emerging risks before they escalate into crises. Anonymous reporting mechanisms protect employee privacy while generating actionable intelligence for organizational improvement.
Assessment data should inform:
- Strategic priorities for mental health investment
- Targeted interventions for high-risk teams or departments
- Evaluation of existing program effectiveness
- Resource allocation decisions across organizational units
- Communication strategies that address identified concerns
Organizations must communicate assessment findings transparently while maintaining individual confidentiality. Employees need to see that their feedback generates tangible improvements, creating a feedback loop that encourages ongoing participation and trust in organizational mental health initiatives.
Creating Psychologically Safe Work Environments
Psychological safety, the shared belief that team members can take interpersonal risks without fear of negative consequences, represents a foundational requirement for workplace mental health. Without psychological safety, employees conceal struggles, avoid seeking support, and experience chronic stress from maintaining professional facades.
Leaders create psychological safety through consistent behaviors that normalize vulnerability, reward help-seeking, and respond constructively to mistakes or challenges. These behaviors for improving mental health extend beyond individual practices to organizational culture.
Teams with high psychological safety demonstrate better performance outcomes, increased innovation, and faster problem resolution. Members share concerns early when interventions remain simple rather than waiting until situations become crises requiring intensive support.
Building Psychological Safety Systematically
Organizations can implement specific practices that cultivate psychological safety across teams and departments. Leadership modeling remains essential, as employees observe senior leader behavior to determine acceptable norms.
Practical psychological safety strategies include:
- Structured check-in processes that normalize discussing challenges
- Explicit permission for flexible work arrangements without justification requirements
- Celebration of help-seeking as strength rather than weakness
- Transparent communication about organizational changes and decision-making
- Consistent application of policies without favoritism or arbitrary enforcement
- Leadership acknowledgment of their own struggles and support-seeking behaviors
Trauma-informed organizational practices enhance psychological safety by recognizing that many employees have experienced adverse events that shape their workplace interactions. Training programs focused on trauma-informed care equip employees with awareness of how past experiences influence present reactions, creating more compassionate and effective work environments.
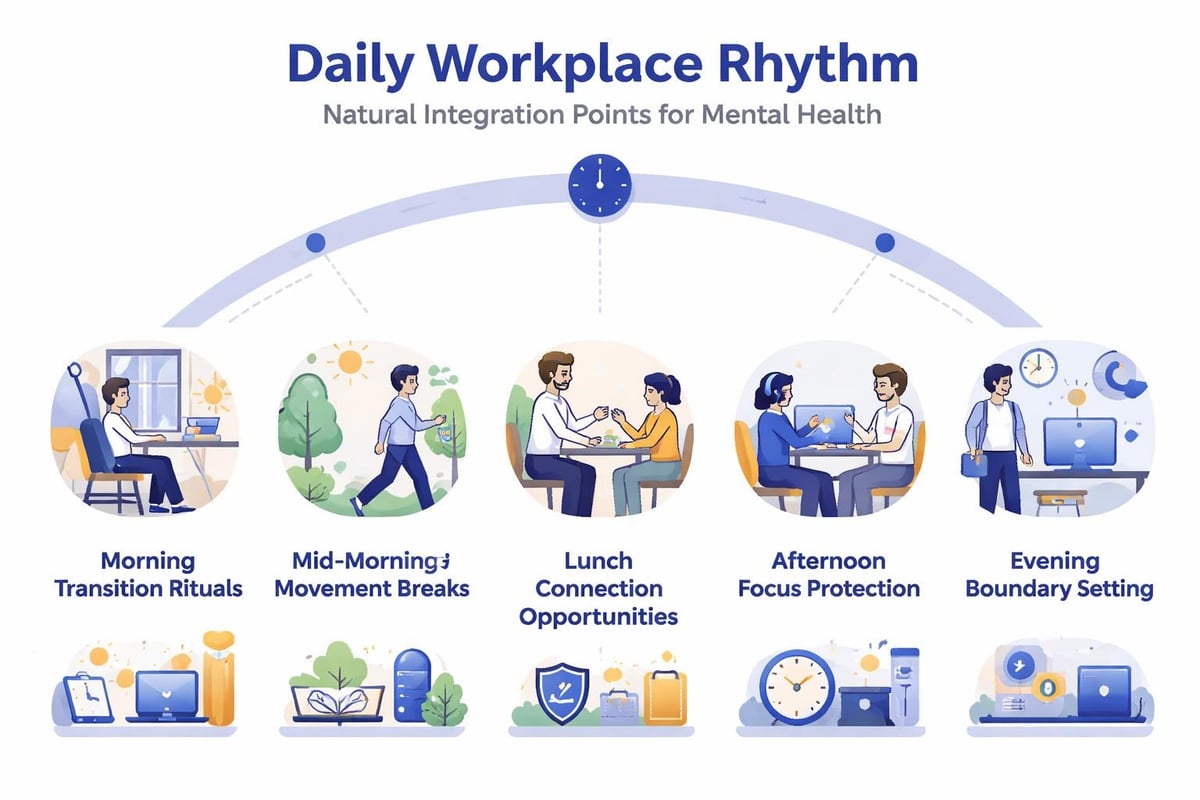
Integrating Daily Wellbeing Practices
While organizational systems create the foundation for mental health, individual practices provide the daily mechanisms through which employees maintain resilience and recover from stressors. Effective strategies to improve mental health combine structural supports with accessible, evidence-based individual practices.
Organizations can facilitate daily wellbeing practices without mandating specific approaches that may not resonate with diverse employee populations. Providing options, education, and enabling environments allows employees to select practices aligned with their preferences, values, and circumstances.
| Practice Category | Examples | Implementation Support |
|---|---|---|
| Physical activity | Walking meetings, stretching breaks, standing desks | Facilities, scheduling norms, leadership modeling |
| Social connection | Team rituals, peer support programs, mentoring | Dedicated time, structured opportunities, recognition |
| Mindfulness and reflection | Meditation apps, quiet spaces, journaling | Resources, physical space, cultural permission |
| Skill development | Learning opportunities, creative projects, autonomy | Budget allocation, time protection, growth pathways |
| Boundary management | Email norms, meeting-free periods, leave encouragement | Policy clarity, manager training, accountability |
Research on strategies rooted in positive psychology demonstrates that practices emphasizing strength-building, meaning-making, and positive emotions complement deficit-focused interventions addressing symptoms or problems.
Organizations should evaluate practice adoption and effectiveness through both utilization data and wellbeing outcome measures. Low participation may indicate implementation barriers, cultural misalignment, or inadequate communication rather than lack of employee interest.
Supporting Sustainable Practice Adoption
Employees often struggle to maintain wellbeing practices despite recognizing their value. Time scarcity, competing priorities, and cultural pressures to prioritize work over self-care create significant barriers.
Organizational supports that address these barriers include:
- Protected time: Designated periods where wellbeing activities receive explicit priority
- Social structures: Group practices that leverage accountability and connection
- Environmental design: Physical and digital spaces that facilitate rather than obstruct healthy behaviors
- Leadership accountability: Manager performance metrics that include team wellbeing indicators
- Resource accessibility: Low-barrier access to tools, spaces, and guidance without bureaucratic obstacles
Establishing Comprehensive Support Pathways
Even with robust prevention strategies, employees will experience mental health challenges requiring targeted support. Organizations must establish clear, accessible pathways connecting employees with appropriate resources matching their needs and preferences.
Support pathway effectiveness depends on multiple factors: awareness, accessibility, quality, cultural appropriateness, and integration with workplace accommodations. Gaps in any element create barriers that prevent employees from receiving timely, effective assistance.
Comprehensive support systems include:
- Employee Assistance Programs offering confidential counseling and practical support
- Peer support networks trained in active listening and resource navigation
- Manager support in implementing workplace adjustments during treatment or recovery
- Return-to-work protocols that facilitate gradual reintegration after leave
- Connection to community mental health services for ongoing clinical care
- Specialized supports for populations facing unique challenges (parents, remote workers, shift workers)
Organizations should regularly evaluate support pathway utilization, identifying whether low uptake reflects genuinely low need or barriers preventing access. Effective strategies for improving mental health care emphasize reducing access barriers and ensuring service quality.
Reducing Help-Seeking Barriers
Multiple obstacles prevent employees from accessing available support despite experiencing significant distress. Understanding these barriers allows organizations to design interventions that increase appropriate help-seeking.
Common barriers include:
- Stigma concerns about professional or social consequences
- Lack of awareness regarding available resources
- Uncertainty about which resource matches specific needs
- Logistical challenges (scheduling, location, cost)
- Previous negative experiences with mental health services
- Cultural factors affecting help-seeking preferences
- Time constraints and competing work demands
Addressing these barriers requires multifaceted approaches combining education, policy clarification, cultural change, and practical accommodations. Organizations demonstrating commitment to confidentiality, non-discrimination, and genuine support increase employee willingness to utilize resources proactively.
Embedding Mental Health in Organizational Strategy
Isolated mental health initiatives, however well-designed, produce limited impact without integration into broader organizational strategy. Strategies to improve mental health achieve sustainability when embedded in operational planning, performance management, budgeting processes, and leadership accountability structures.
Strategic integration positions mental health as a core organizational capability rather than a peripheral HR program. This positioning influences resource allocation, priority setting, and cultural messaging about the organization’s genuine commitments.
Strategic Integration Elements
| Integration Point | Action | Impact |
|---|---|---|
| Leadership metrics | Include team wellbeing in manager scorecards | Accountability and prioritization |
| Budget allocation | Dedicate recurring funding for mental health infrastructure | Sustainability and predictability |
| Risk management | Include psychological hazards in risk assessments | Prevention focus and compliance |
| Change processes | Require wellbeing impact analysis for major initiatives | Proactive harm reduction |
| Performance systems | Recognize mental health contributions alongside other outcomes | Cultural validation and behavior change |
Australian organizations increasingly recognize that strategic mental health investment generates measurable returns through reduced absence costs, improved productivity, and enhanced employer brand attractiveness.
Organizations should establish clear governance structures with designated accountability for mental health strategy oversight, implementation coordination, and outcome monitoring. Without explicit ownership, mental health initiatives compete unsuccessfully with more immediate operational priorities.
Leveraging Technology and Digital Solutions
Digital tools expand access to mental health resources, provide personalized interventions, and generate data for continuous improvement. However, technology should complement rather than replace human connection and organizational culture change.
Effective digital mental health strategies include:
- Assessment platforms: Automated wellbeing measurement with real-time reporting
- Educational content: On-demand training accessible across locations and schedules
- Therapeutic tools: Evidence-based apps supporting specific skills (mindfulness, sleep, anxiety management)
- Connection platforms: Peer support forums, virtual group programs, chat-based counseling
- Integration systems: Platforms connecting multiple resources through unified interfaces
Organizations must evaluate digital solutions rigorously, ensuring evidence quality, data privacy protection, and alignment with organizational values and culture. Not all employees prefer digital interventions, requiring hybrid approaches that accommodate diverse preferences.
Technology also enables innovative delivery models for workplace mental health training. Video resources provide scalable learning opportunities while maintaining expert-led quality and consistent messaging across distributed workforces.
Maximizing Digital Tool Effectiveness
Digital solution success depends on thoughtful implementation addressing common adoption barriers. Employees need clear guidance on which tools serve specific purposes, how to access resources, and what outcomes they can expect.
Implementation considerations include:
- User experience quality and accessibility standards
- Integration with existing workflow rather than additional burdens
- Privacy safeguards and transparent data usage policies
- Personalization options respecting individual preferences
- Technical support availability for troubleshooting
- Regular evaluation and refinement based on user feedback
Organizations should avoid overwhelming employees with excessive tool options. Curating a focused suite of high-quality, complementary resources proves more effective than offering extensive catalogs requiring significant navigation effort.
Addressing Specific Population Needs
Workplace populations demonstrate significant diversity in mental health needs, preferences, and barriers to support. Effective strategies recognize this diversity through tailored approaches for specific groups while maintaining equitable access and inclusive environments.
Populations requiring targeted consideration include:
- Remote and hybrid workers experiencing isolation and boundary challenges
- Shift workers and non-standard schedule employees facing circadian and social disruption
- Parents and caregivers managing multiple role demands
- Young workers establishing career foundations while navigating developmental challenges
- Employees from culturally diverse backgrounds with varied mental health frameworks
- Workers with lived experience of mental health conditions requiring accommodation
Inclusive program design incorporates diverse perspectives during development, pilots interventions with specific populations, and maintains feedback mechanisms ensuring ongoing responsiveness to emerging needs.
Organizations should avoid assumptions about population needs based on demographic characteristics. Individual variation within any group exceeds variation between groups, requiring personalized approaches within population-specific frameworks.
Measuring Impact and Demonstrating Value
Rigorous evaluation proves essential for demonstrating mental health program value, securing ongoing investment, and identifying improvement opportunities. Organizations should establish evaluation frameworks before implementing initiatives, ensuring appropriate baseline data collection and outcome measurement.
Comprehensive evaluation examines multiple domains:
- Reach: Participation rates across intended populations
- Satisfaction: User experience and perceived value
- Knowledge and attitudes: Awareness, understanding, and stigma reduction
- Behavior change: Application of skills and resource utilization
- Health outcomes: Wellbeing measures, symptom reduction, functioning improvement
- Organizational metrics: Absenteeism, turnover, productivity, engagement
- Return on investment: Cost-benefit analysis comparing program costs to measurable savings
Quality improvement strategies emphasize continuous measurement and iterative refinement based on emerging evidence rather than one-time evaluation after program completion.
Organizations should communicate evaluation findings transparently, acknowledging both successes and improvement areas. Honest assessment builds credibility and demonstrates genuine commitment to evidence-based practice rather than performative initiatives.
Building Evaluation Capacity
Many organizations lack internal expertise for rigorous mental health program evaluation. Building capacity through training, external partnerships, or dedicated roles ensures evaluation quality and sustainability.
Evaluation capacity requirements include:
- Research methodology knowledge for appropriate design selection
- Data collection and analysis capabilities
- Ethical frameworks protecting participant confidentiality
- Stakeholder communication skills translating findings into actionable insights
- Continuous improvement mindsets embracing iterative refinement
External partnerships with specialized organizations provide access to evaluation expertise, benchmarking data, and industry best practices. These collaborations accelerate learning while maintaining independence in outcome assessment.
Implementing comprehensive strategies to improve mental health requires sustained commitment, strategic integration, and evidence-based approaches tailored to organizational contexts. Organizations that invest in manager capability, systematic assessment, psychological safety, individual practices, accessible support pathways, and rigorous evaluation create environments where employees thrive while advancing business performance. Workplace Mental Health Institute provides specialized training programs and strategic consultation supporting organizations in developing and implementing effective workplace mental health strategies that deliver measurable outcomes for employees and organizational success.


