Depression in employees represents one of the most significant yet frequently misunderstood challenges facing modern workplaces. Organizations lose billions annually in productivity, absenteeism, and turnover costs associated with untreated mental health conditions. Yet managers and HR professionals often lack the framework to identify, support, and appropriately respond when team members struggle with depressive symptoms. This comprehensive guide provides evidence-based strategies for recognizing and addressing workplace depression while maintaining both compassion and organizational effectiveness.
Understanding Depression in the Workplace Context
Depression manifests differently in professional settings than in clinical descriptions. While diagnostic criteria focus on persistent sadness, loss of interest, and physiological symptoms, workplace presentations often appear as decreased productivity, withdrawal from colleagues, or increased irritability during meetings.
Key workplace indicators include:
- Noticeable decline in work quality or missed deadlines from previously reliable performers
- Physical absence patterns, particularly Monday absences or frequent medical appointments
- Social withdrawal from team activities, lunch breaks, or collaborative projects
- Visible changes in energy levels, concentration, or decision-making capacity
- Uncharacteristic emotional responses to routine workplace stressors
Research on employers’ attitudes toward managing employees with depression reveals significant variability in how organizations perceive and respond to mental health challenges. Many managers express uncertainty about appropriate interventions, fearing both legal implications and causing personal offense.

The Distinction Between Clinical Depression and Workplace Distress
Not every period of low mood constitutes clinical depression. Employees experience normal emotional responses to workplace challenges, organizational change, or personal life events. The critical distinction lies in duration, severity, and functional impairment.
Clinical depression typically involves symptoms persisting for at least two weeks, significantly interfering with daily functioning across multiple life domains. Workplace distress may be situational, improving when specific stressors resolve or when appropriate support is provided.
Managers need not become diagnosticians. Their role involves recognizing concerning patterns, initiating supportive conversations, and connecting employees with appropriate resources rather than determining clinical diagnoses.
The Leadership Factor in Employee Mental Health
Management behaviors substantially influence the prevalence and severity of depression in employees. Studies examining leaders’ dark personality traits demonstrate that workplace bullying and toxic leadership directly correlate with elevated depressive symptoms among team members.
| Leadership Behavior | Impact on Employee Mental Health | Protective Alternative |
|---|---|---|
| Micromanagement | Increases stress, reduces autonomy | Clear expectations with decision-making latitude |
| Public criticism | Triggers shame, isolation | Private, constructive feedback focused on growth |
| Unrealistic demands | Creates chronic overwhelm | Collaborative goal-setting with resource discussion |
| Inconsistent communication | Generates anxiety, uncertainty | Transparent, regular updates on priorities |
Research on how managers’ attitudes affect their assessment of work capacity indicates that leader perceptions significantly influence whether employees receive appropriate accommodation or face performance management procedures.
Building Psychologically Safe Management Practices
Psychological safety enables employees to disclose mental health challenges without fear of career repercussions. Organizations cultivating this environment experience earlier intervention, better treatment adherence, and faster recovery trajectories.
Practical applications include:
- Normalize mental health discussions through regular check-ins that include wellbeing alongside performance
- Model vulnerability by leaders sharing appropriate personal experiences with stress management
- Respond consistently to disclosures with empathy and solution-focused support
- Eliminate performative wellness initiatives that lack genuine organizational commitment
The Workplace Mental Health Institute offers comprehensive training programs that equip managers with practical frameworks for these conversations, moving beyond awareness to actionable skill development.
Organizational Risk Factors and Protective Elements
Certain workplace characteristics systematically elevate depression risk. Understanding these structural elements enables organizations to implement preventive strategies rather than solely reactive interventions.
High-Risk Environmental Factors
Role ambiguity creates chronic stress as employees struggle to meet unclear expectations. When combined with high demands and low control, this constellation produces particularly elevated mental health risks.
Job insecurity, whether from organizational restructuring or precarious employment arrangements, generates sustained anxiety that frequently progresses to depressive symptoms. The anticipatory stress of potential job loss often exceeds the actual experience of unemployment.
Conflict management styles significantly influence employee mental health outcomes, with emotional exhaustion serving as a mediating pathway between interpersonal workplace conflict and depressive symptoms.
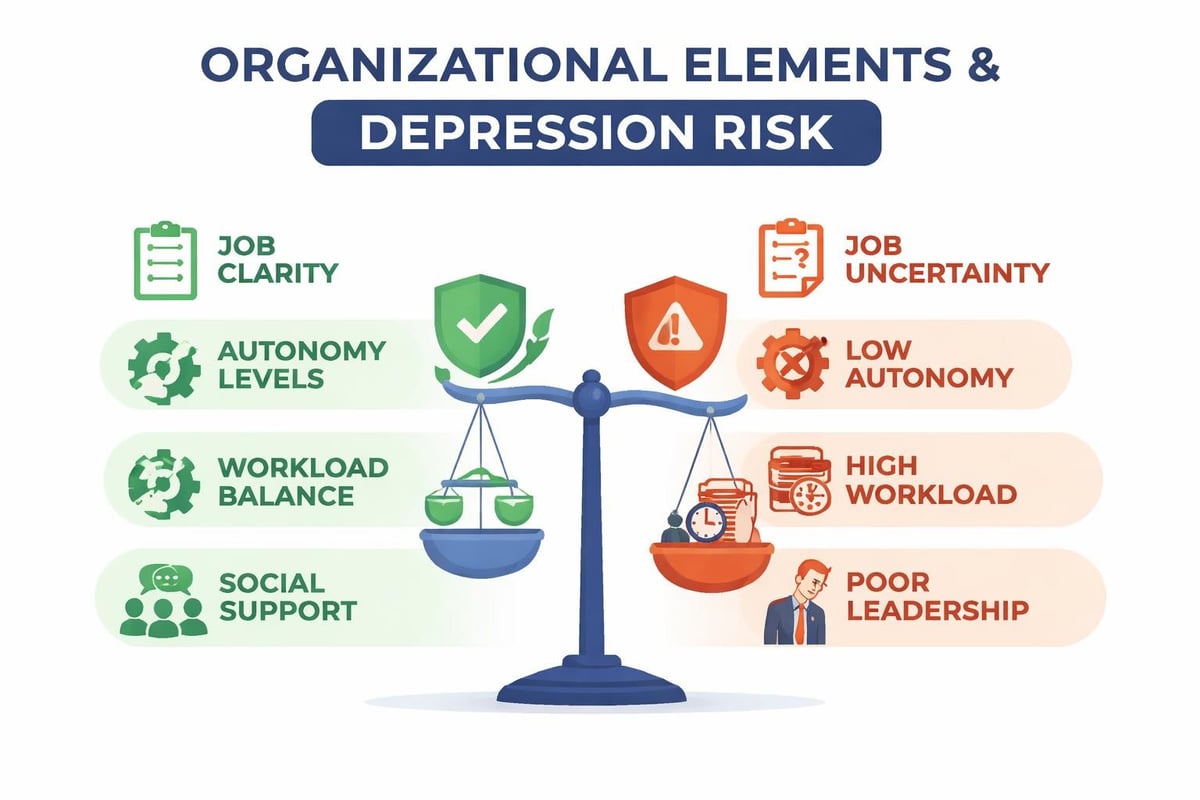
Protective Organizational Structures
Organizations with lower prevalence of depression in employees share common structural characteristics. These aren’t merely cultural aspirations but embedded operational practices.
- Clear reporting relationships that eliminate competing priorities and contradictory directives
- Adequate staffing levels allowing reasonable workload distribution and coverage for absences
- Transparent promotion criteria reducing ambiguity about career progression pathways
- Regular performance feedback providing ongoing clarity rather than annual surprises
- Accessible mental health resources integrated into health benefits with minimal barriers
Investment in these structural protections yields measurable returns through reduced presenteeism, lower turnover costs, and enhanced organizational performance.
Practical Response Frameworks for Managers
When managers suspect an employee may be experiencing depression, knowing how to initiate conversation proves crucial. Avoidance worsens outcomes, yet poorly executed conversations can damage trust and escalate distress.
The Supportive Conversation Structure
Effective conversations balance genuine concern with professional boundaries. Managers need not become therapists, but they must demonstrate authentic care while maintaining appropriate roles.
Opening the conversation:
Begin with specific, observable changes rather than diagnostic labels. “I’ve noticed you’ve seemed less engaged in team meetings lately, which is unusual for you. I wanted to check in and see how things are going” proves more effective than “Are you depressed?”
Active listening without problem-solving:
Resist the urge to immediately fix or minimize concerns. Validation precedes solutions. “That sounds incredibly difficult” acknowledges experience without rushing to remedies.
Connecting to resources:
Frame employee assistance programs, mental health benefits, or workplace accommodations as standard support tools rather than crisis interventions. “Many people find our EAP helpful for various challenges. Would it be useful for me to send you that information?”
Documentation and Privacy Considerations
Managers must balance organizational record-keeping requirements with employee privacy rights. Document observable workplace impacts (missed deadlines, attendance patterns, performance changes) without recording medical information or diagnostic speculation.
Gender differences in managerial attitudes reveal that male and female managers may approach employee mental health differently, highlighting the importance of standardized, evidence-based response protocols that transcend individual manager preferences.
Accommodation Strategies and Performance Management
Depression qualifies as a disability under most employment legislation, requiring reasonable workplace accommodations. However, determining appropriate adjustments while maintaining performance standards challenges many organizations.
| Accommodation Type | Example Implementation | Performance Expectation |
|---|---|---|
| Flexible scheduling | Core hours with flexibility for therapy appointments | Same output within adjusted timeframe |
| Modified workspace | Quieter location reducing sensory overwhelm | Maintained quality standards |
| Adjusted deadlines | Extended timelines during acute episodes | Clear milestone communication |
| Task restructuring | Temporary reduction in client-facing responsibilities | Alternate contributions of equivalent value |
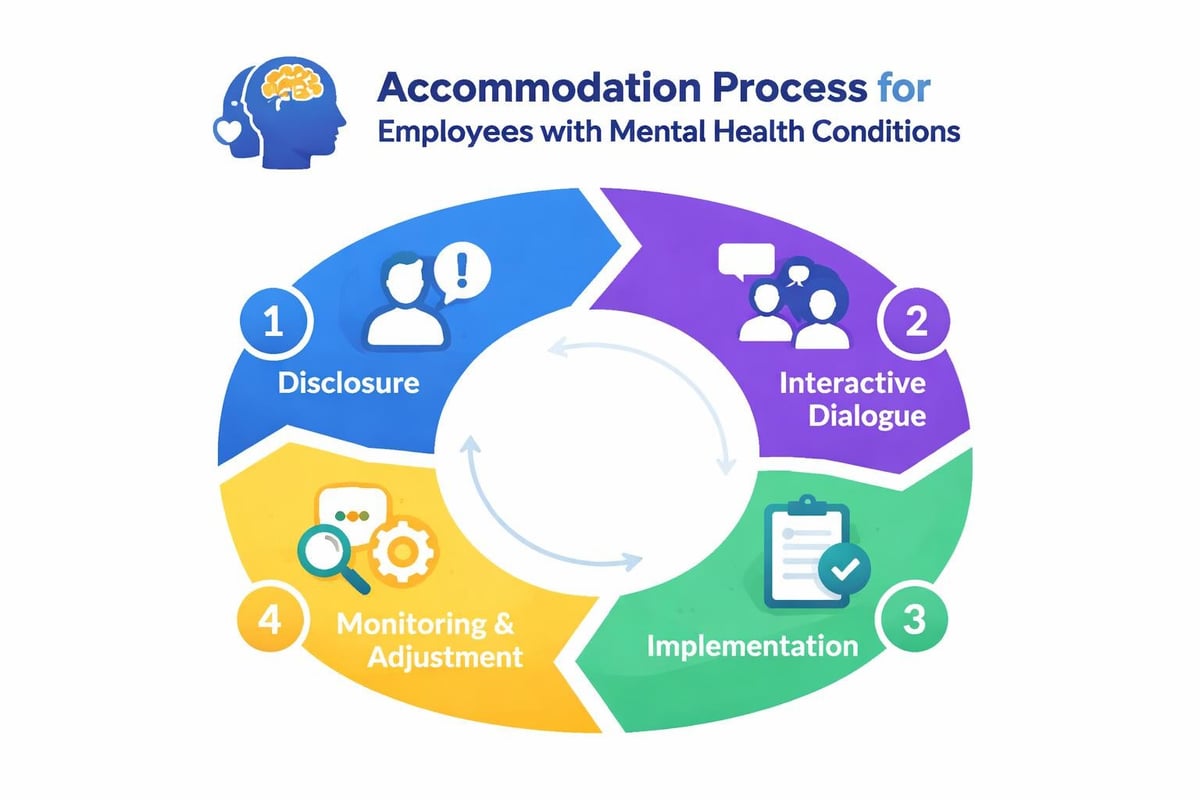
The accommodation process should:
- Begin with employee-requested adjustments rather than manager assumptions
- Involve interactive dialogue about what modifications would genuinely help
- Establish clear performance expectations within the accommodated framework
- Include regular review points to assess effectiveness and adjust as needed
- Document the process while maintaining medical information confidentially
Organizations sometimes conflate compassion with lowered standards. Effective accommodation maintains performance expectations while removing barriers to achievement.
The Absenteeism and Presenteeism Calculation
Depression impacts workplace productivity through both absence and reduced effectiveness while present. Studies on antidepressant treatment and absenteeism demonstrate that appropriate clinical intervention significantly reduces work absence, yet presenteeism costs often exceed direct absenteeism expenses.
Presenteeism, where employees attend work while functioning below capacity, proves difficult to measure yet substantially impacts organizational performance. An employee working at 60% capacity for months generates greater productivity loss than a two-week absence followed by full recovery.
Creating Return-to-Work Protocols
Structured return-to-work processes following mental health absence reduce re-occurrence rates and facilitate sustainable reintegration. Unlike physical injuries with clear healing timelines, mental health recovery follows non-linear trajectories requiring adaptive support.
Effective return protocols include:
- Pre-return conversation clarifying any ongoing accommodations or gradual schedule increases
- Designated check-in person (not necessarily direct supervisor) for first weeks back
- Explicitly addressing workload coverage to prevent immediate overwhelm
- Team communication plan respecting employee privacy preferences
- Scheduled follow-up discussions at 2 weeks, 1 month, and 3 months post-return
Manager Training and Organizational Capability Building
Research on managers’ knowledge and stigmatizing attitudes demonstrates that mental health literacy significantly reduces stigma and improves supportive responses. Organizations investing in comprehensive manager training observe measurably better employee mental health outcomes.
Effective training extends beyond awareness sessions to skill-building programs teaching specific conversation techniques, accommodation implementation, and early intervention recognition. The distinction matters: knowing depression exists differs fundamentally from confidently managing performance conversations with employees experiencing depression.
For organizations seeking evidence-based manager development, specialized training platforms offer structured curriculum combining psychological accuracy with practical workplace application. Australian organizations can access region-specific resources through tailored programs addressing local regulatory and cultural contexts.
Building Organizational Mental Health Literacy
While manager capability proves essential, organization-wide mental health literacy creates cultural shifts that reduce stigma and normalize help-seeking. When employees understand mental health conditions as treatable medical issues rather than character flaws, disclosure rates increase and intervention happens earlier.
Comprehensive literacy programs address:
- Accurate information about common mental health conditions and recovery trajectories
- Recognition that mental health exists on a continuum, not a binary healthy/ill division
- Practical self-care strategies applicable across the mental health spectrum
- Clear information about available organizational resources and access processes
- Personal stories from colleagues who’ve navigated mental health challenges successfully
Measuring Organizational Mental Health Outcomes
Organizations committed to addressing depression in employees require metrics beyond employee satisfaction surveys. Meaningful measurement tracks both prevalence indicators and intervention effectiveness.
Leading indicators (preventive focus):
- Psychological safety scores from validated instruments
- Manager confidence ratings in handling mental health conversations
- Employee assistance program utilization rates and presenting concerns
- Early intervention touchpoint completion (wellness checks, stay interviews)
Lagging indicators (outcome focus):
- Short-term disability claims for mental health conditions
- Absenteeism patterns, particularly unplanned single-day absences
- Turnover rates with exit interview mental health themes
- Workers’ compensation stress claims
- Productivity metrics correlated with team psychological safety
Advanced organizations correlate these metrics with specific interventions, identifying which programs generate measurable impact versus those consuming resources without meaningful outcomes. This evidence-based approach to workplace mental health mirrors clinical medicine’s progression toward outcome-driven care.
The Stigma Reduction Imperative
Despite decades of mental health advocacy, workplace stigma remains the primary barrier preventing employees from seeking help. Studies examining how employees with depressogenic attributional styles respond to workplace gossip reveal the complex social dynamics that either support or undermine employees experiencing depression.
Stigma operates at multiple levels: public stigma (societal discrimination), organizational stigma (workplace policies and practices that disadvantage those with mental health conditions), and self-stigma (internalized shame preventing help-seeking).
Organizational Strategies for Stigma Reduction
Effective stigma reduction requires sustained, multi-faceted approaches rather than single awareness campaigns. Organizations successfully reducing mental health stigma typically implement:
- Leadership disclosure of personal or family mental health experiences, humanizing these challenges
- Policy equity ensuring mental health conditions receive identical treatment to physical health issues
- Language guidance moving from pathologizing terminology to person-first, recovery-oriented language
- Visible resource promotion normalizing employee assistance programs as professional development tools
- Success stories highlighting employees who accessed support and successfully continued their careers
Organizations can reference research-backed approaches and video resources that demonstrate practical implementation of these strategies across various workplace contexts.
Creating Sustainable Workplace Mental Health Systems
Addressing depression in employees effectively requires systematic approaches rather than ad hoc interventions. Sustainable systems integrate mental health considerations into existing organizational processes instead of creating parallel structures.
Integration points include:
- Recruitment and onboarding providing mental health resource information alongside benefits enrollment
- Performance management incorporating wellbeing check-ins into regular supervision conversations
- Change management assessing mental health impacts of organizational restructuring
- Exit interviews gathering data on whether mental health factors influenced departure decisions
- Leadership development embedding psychological safety and mental health literacy into management competencies
This systematic integration positions mental health as a standard organizational consideration rather than a specialized HR function, distributing responsibility appropriately across leadership levels while maintaining expert support for complex situations.
Organizations that effectively address depression in employees recognize this as both an ethical imperative and a strategic advantage, combining compassionate support with measurable business outcomes. By implementing evidence-based training, creating psychologically safe environments, and establishing clear response protocols, leaders can substantially improve both employee wellbeing and organizational performance. Workplace Mental Health Institute specializes in transforming these principles into practical, sustainable workplace programs through comprehensive training, assessment tools, and strategic consultation tailored to your organizational context.


