Organizations that prioritize employee psychological wellbeing demonstrate measurably better performance outcomes across multiple domains. Mental health programs for employees have evolved from reactive crisis interventions into strategic investments that address both individual flourishing and organizational sustainability. The contemporary landscape demands evidence-informed approaches that balance compassionate support with practical implementation, recognizing that workplace mental health exists within complex systems involving leadership capability, organizational culture, and structural factors beyond individual control.
Understanding Comprehensive Mental Health Programs
Mental health programs for employees encompass structured interventions designed to prevent psychological distress, promote resilience, and provide support pathways when challenges arise. These programs represent coordinated efforts spanning multiple organizational levels rather than isolated initiatives.
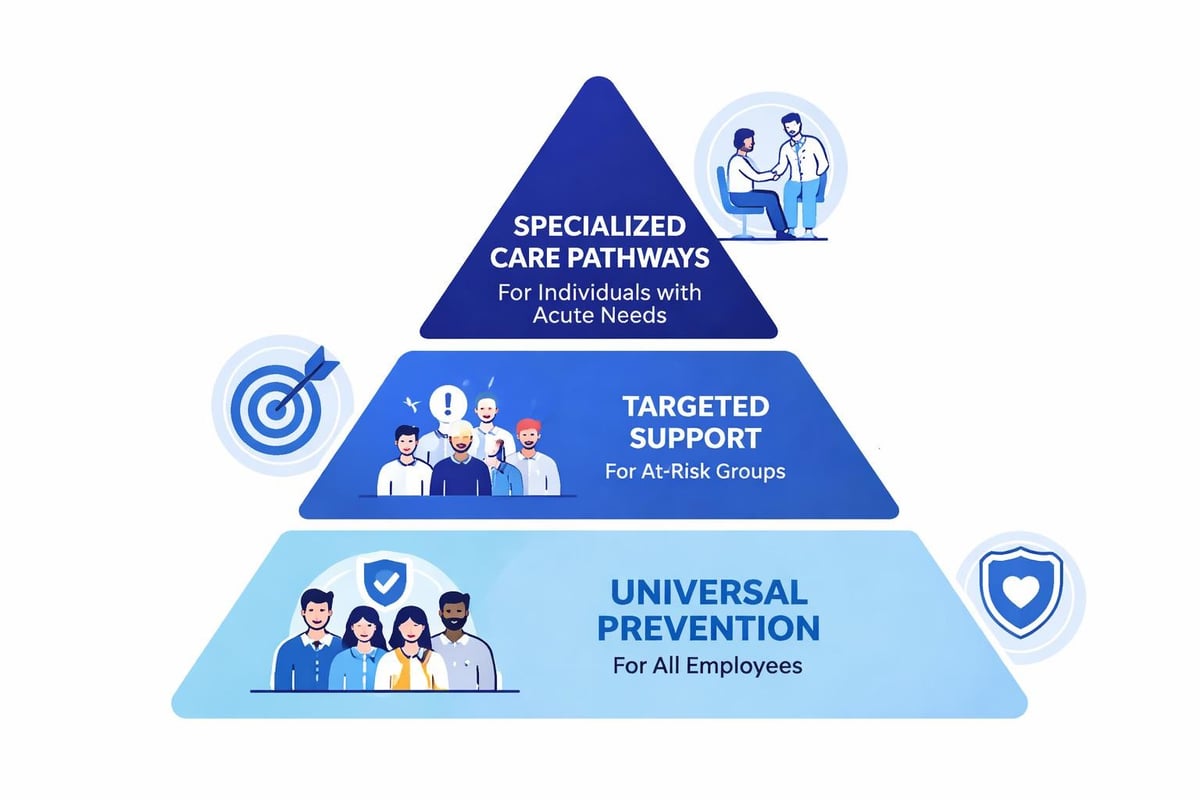
Effective programs distinguish between universal prevention strategies available to all employees, targeted interventions for at-risk populations, and indicated support for individuals experiencing acute difficulties. This tiered framework ensures resources align with varied needs while maximizing reach and impact.
Core Program Components
Organizations implementing robust mental health programs typically integrate several foundational elements:
- Leadership and manager training to recognize distress indicators and respond appropriately
- Employee education covering stress management, resilience skills, and help-seeking behaviors
- Accessible support pathways including Employee Assistance Programs and referral networks
- Environmental modifications addressing psychosocial hazards and work design factors
- Measurement systems tracking participation, satisfaction, and organizational health indicators
The American Psychiatric Association Foundation’s Center for Workplace Mental Health provides extensive resources for employers developing these multi-component approaches, emphasizing that isolated interventions rarely produce sustainable change.
Strategic Implementation Frameworks
Successful deployment of mental health programs for employees requires deliberate planning rather than ad-hoc adoption of popular initiatives. Organizations must begin with systematic assessment of existing conditions, employee needs, and capacity constraints.
Assessment and Planning Phase
| Assessment Domain | Key Questions | Data Sources |
|---|---|---|
| Current State | What support already exists? What are utilization patterns? | Program records, insurance claims, absence data |
| Employee Needs | What challenges do employees report? Which populations face elevated risk? | Surveys, focus groups, health assessments |
| Organizational Readiness | What resources are available? How supportive is leadership? | Budget review, stakeholder interviews |
| Cultural Context | How is mental health discussed? What stigma exists? | Climate surveys, employee feedback |
This foundational work prevents common implementation failures where programs mismatch actual needs or lack necessary organizational support. The Workplace Mental Health Institute specializes in conducting these workplace wellbeing assessments to establish evidence-based implementation roadmaps.
Building Leadership Capability
Manager competency represents the most critical success factor for mental health programs. Supervisors lacking confidence or skills in responding to employee distress inadvertently create barriers to help-seeking and exacerbate psychological safety concerns.
Effective training equips managers with:
- Recognition skills to identify behavioral changes indicating potential distress
- Conversation frameworks for expressing concern without diagnosing or overstepping boundaries
- Referral knowledge connecting employees to appropriate professional resources
- Boundary awareness distinguishing supportive management from therapeutic intervention
- Self-care strategies preventing vicarious trauma and burnout
Research consistently demonstrates that trained managers show greater confidence initiating mental health conversations and employees report increased willingness to disclose challenges. Training programs available through thewmhionline.com provide practical, scenario-based learning addressing real workplace situations.
Evidence-Based Program Elements
Mental health programs for employees demonstrate varying effectiveness depending on design quality and implementation fidelity. Organizations should prioritize interventions supported by rigorous evaluation evidence.
Resilience and Skills Training
Structured programs teaching specific psychological competencies produce measurable improvements in employee wellbeing and performance. Effective resilience training focuses on modifiable cognitive and behavioral patterns rather than personality transformation.
Core skill domains include:
- Cognitive flexibility techniques for reframing challenging situations
- Emotional regulation strategies managing activation and reactivity
- Problem-solving approaches addressing controllable stressors systematically
- Social connection skills strengthening workplace relationships
- Recovery practices ensuring adequate detachment from work demands
These evidence-informed approaches differ substantially from superficial “wellness tips” by providing transferable frameworks employees can apply across varied circumstances. Programs emphasizing skill acquisition and practice demonstrate superior outcomes compared to awareness-only interventions.
Employee Assistance Programs
Employee Assistance Programs (EAPs) provide confidential counseling and support services addressing personal challenges affecting workplace functioning. Contemporary EAPs extend beyond traditional short-term counseling to offer work-life resources, legal consultation, and financial guidance.
| EAP Feature | Traditional Model | Comprehensive Model |
|---|---|---|
| Service Scope | 3-6 counseling sessions | Integrated support ecosystem |
| Access Points | Phone hotline only | Multiple channels including digital |
| Utilization Rate | 3-5% annually | 15-25% with enhanced promotion |
| Manager Tools | Basic referral information | Training, consultation, critical incident response |
| Measurement | Session counts | Outcomes tracking, ROI analysis |
Maximizing EAP value requires active promotion beyond passive availability. Organizations achieving high utilization integrate EAP messaging into onboarding, manager training, and regular communications while ensuring genuinely confidential access.
Addressing Organizational Risk Factors
Individual-focused interventions alone prove insufficient when workplace conditions systematically undermine psychological health. Mental health programs for employees must address environmental and structural determinants alongside personal resilience.
Psychosocial Hazard Management
Psychosocial hazards represent aspects of work design, management, and organizational context that increase injury risk, including psychological harm. Common hazards include:
- Job demands exceeding employee capacity or control
- Role ambiguity regarding expectations and responsibilities
- Interpersonal conflict including bullying and harassment
- Low support from supervisors or colleagues
- Organizational injustice in decision-making and treatment
- Change uncertainty during restructures or transitions
The CDC emphasizes that addressing these workplace factors requires systematic risk assessment and control implementation similar to physical safety protocols. Organizations often overlook this primary prevention layer, focusing exclusively on helping employees cope with preventable stressors.
Trauma-Informed Workplace Practices
Significant proportions of employees have experienced trauma that influences workplace interactions and stress responses. Trauma-informed approaches modify organizational practices to avoid re-traumatization while supporting recovery.
Key principles include:
- Safety in physical and psychological dimensions
- Trustworthiness through transparent and consistent operations
- Peer support enabling connection and mutual assistance
- Collaboration in decision-making affecting employees
- Empowerment emphasizing strengths and skill development
- Cultural responsiveness acknowledging diverse backgrounds and experiences
Implementing trauma-informed practices doesn’t require knowing individual employee histories but rather creating environments that accommodate varied needs and avoid common triggering situations. Training programs focused on trauma-informed care help organizations operationalize these principles across policies and practices.
Measuring Program Effectiveness
Rigorous evaluation distinguishes performative mental health initiatives from substantive programs driving meaningful improvement. Organizations should establish measurement frameworks before program launch rather than attempting retrospective assessment.
Multi-Level Outcome Indicators
| Measurement Level | Example Metrics | Data Collection Method |
|---|---|---|
| Individual Wellbeing | Psychological distress, life satisfaction, burnout | Validated survey instruments |
| Workplace Functioning | Engagement, productivity, presenteeism | Performance data, self-report |
| Health Utilization | Healthcare costs, disability claims, EAP usage | Administrative records |
| Organizational Health | Turnover, absence, safety incidents | HR systems |
| Culture Indicators | Psychological safety, stigma, manager confidence | Climate surveys |
Comprehensive evaluation examines multiple indicators rather than relying on single metrics vulnerable to confounding. Mental Health America offers assessment tools and benchmarking resources helping organizations establish baseline measurements and track progress.
Return on Investment Analysis
Financial stakeholders increasingly demand evidence that mental health programs for employees generate measurable returns. While not all program value translates to monetary metrics, rigorous ROI analysis strengthens business cases for sustained investment.
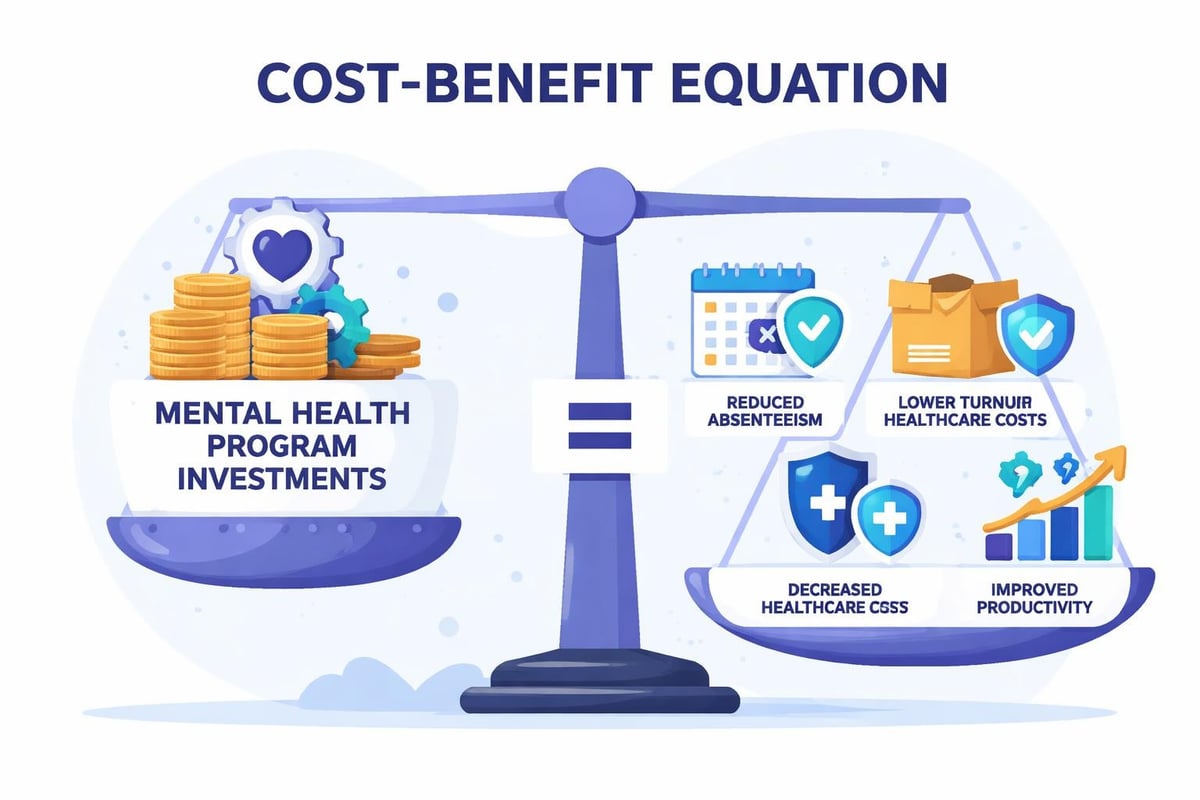
Calculable returns include:
- Reduced absenteeism costs from fewer unplanned absences
- Lower turnover expenses through improved retention
- Decreased healthcare spending from prevention and early intervention
- Enhanced productivity via reduced presenteeism
- Workers compensation savings from fewer psychological injury claims
Conservative ROI analyses typically demonstrate $3-6 return for each dollar invested in comprehensive programming, though specific returns vary by industry, program design, and measurement methodology.
Emerging Trends and Innovations
Mental health programs for employees continue evolving as technology, research, and workforce expectations advance. Organizations should monitor emerging approaches while maintaining commitment to evidence-based core programming.
Digital Mental Health Tools
Technology-enabled interventions expand access beyond traditional service delivery constraints. Validated digital tools include guided meditation apps, cognitive behavioral therapy platforms, and stress detection algorithms integrated with support systems providing real-time assistance.
Advantages of digital approaches:
- Accessibility removing geographic and scheduling barriers
- Anonymity reducing stigma concerns for some users
- Scalability serving large populations cost-effectively
- Personalization adapting content to individual needs and preferences
- Data generation enabling outcome tracking and program refinement
However, digital tools complement rather than replace human support for employees with complex needs. Organizations should integrate technology strategically within comprehensive programs rather than substituting apps for substantive investment.
Peer Support Networks
Structured peer support programs train employees to provide non-clinical assistance to colleagues experiencing difficulties. These initiatives leverage natural workplace relationships while ensuring appropriate boundaries and referral pathways exist.
Benefits include normalized help-seeking, increased early identification, and enhanced social connection. Effective peer programs provide thorough training covering active listening, resource knowledge, and scope limitations while establishing clear supervision and support for peer supporters themselves.
The updated Notice. Talk. Act.® at Work training specifically addresses peer relationship strengthening alongside manager capability development, recognizing the complementary roles different organizational actors play.
Implementation Challenges and Solutions
Organizations frequently encounter predictable obstacles when launching mental health programs for employees. Anticipating common challenges enables proactive mitigation strategies.
Overcoming Stigma Barriers
Persistent stigma surrounding mental health remains the primary barrier to program utilization despite increasing awareness. Employees fear professional consequences from disclosure and question whether organizational support claims reflect genuine commitment.
Effective stigma reduction requires multi-faceted approaches:
- Leadership disclosure when appropriate, modeling openness about mental health
- Language modification using non-stigmatizing terminology in policies and communications
- Success story sharing from employees who benefited from support
- Manager accountability for creating psychologically safe team environments
- Structural changes removing policies that inadvertently penalize help-seeking
Cultural transformation occurs gradually through consistent messaging and demonstrated organizational values rather than single awareness campaigns. Resources available through SAMHSA’s workplace mental health guidance help organizations develop comprehensive stigma reduction strategies.
Ensuring Equitable Access
Mental health programs often inadvertently serve already-advantaged employee populations while missing those facing greatest need. Equity requires deliberate design considering varied employee circumstances.
Access barriers requiring attention:
- Scheduling constraints for shift workers unable to attend standard programming
- Language limitations for employees with limited English proficiency
- Digital divides excluding those without reliable technology access
- Cultural relevance of content and delivery approaches
- Remote worker inclusion in organization-based programs
Equity audits examining program utilization across demographic categories reveal disparities requiring targeted solutions. Organizations committed to inclusive mental health support continuously refine approaches based on participation data rather than assuming universal accessibility.
Sustaining Long-Term Program Success
Initial program enthusiasm frequently wanes without deliberate sustainability planning. Mental health programs for employees require ongoing investment, adaptation, and leadership commitment extending beyond launch periods.
Building Organizational Capacity
Sustainable programs integrate mental health competency across organizational systems rather than isolating it within specialized roles. This distributed responsibility model ensures continuity despite personnel changes while normalizing psychological wellbeing as core business practice.
Capacity-building strategies include:
- Embedding mental health in existing processes like performance management and safety protocols
- Developing internal champions across departments and levels
- Creating feedback loops for continuous program improvement
- Allocating dedicated resources rather than expecting volunteer efforts
- Leadership development ensuring executives maintain commitment and accountability
Organizations in Australia can access specialized support through WMHI Australia for building sustainable workplace mental health infrastructure aligned with regional regulatory and cultural contexts.
Adapting to Changing Needs
Workforce demographics, economic conditions, and global events continuously reshape employee mental health needs. Effective programs incorporate regular review cycles adjusting priorities and approaches based on emerging evidence.
Adaptation mechanisms include annual needs assessments, employee advisory groups, benchmarking against industry standards, and monitoring utilization patterns identifying unmet needs or declining engagement with specific offerings.
Implementing effective mental health programs for employees requires strategic planning, evidence-based design, and sustained organizational commitment that extends beyond surface-level wellness initiatives. Organizations seeking to develop comprehensive approaches benefiting both employee wellbeing and business outcomes can partner with experts who understand the complexity of workplace mental health systems. Workplace Mental Health Institute provides specialized training, assessment, and consultation services designed to build practical capabilities across leadership teams while establishing measurement frameworks that demonstrate genuine impact.


