Organizations that implement comprehensive workplace strategies for mental health consistently outperform those that treat employee wellbeing as an afterthought. The business case extends beyond compliance or risk management to encompass measurable improvements in productivity, retention, and organizational resilience. For HR professionals and business leaders, understanding the difference between superficial wellness initiatives and transformative mental health strategies determines whether your organization thrives or merely survives in an increasingly complex work environment.
The Foundation: Organizational Commitment to Psychological Safety
Effective workplace strategies for mental health begin with organizational commitment that transcends policy documents. Psychological safety requires deliberate architecture at every level, from executive decision-making to front-line management practices. When employees believe they can express concerns, admit mistakes, or request support without facing negative consequences, organizations unlock unprecedented levels of engagement and innovation.
Leadership behavior sets the tone for this cultural foundation. Senior leaders who openly discuss mental health, model healthy boundaries, and visibly prioritize wellbeing create permission for managers and employees to follow suit. This top-down approach must align with bottom-up mechanisms that capture employee voice and translate feedback into actionable improvements.
Building Leadership Capacity
Managers represent the critical leverage point in any mental health strategy. Providing training for supervisors equips them to recognize early warning signs, initiate supportive conversations, and navigate complex situations with confidence rather than avoidance.
Essential leadership competencies include:
- Recognizing behavioral changes that may indicate psychological distress
- Conducting psychologically informed performance conversations
- Making reasonable adjustments to support employee needs
- Connecting employees to appropriate resources without overstepping professional boundaries
- Managing their own wellbeing to prevent burnout and maintain capacity
Training programs for managers should emphasize practical application over theoretical knowledge. Role-play scenarios, case-based learning, and ongoing supervision create sustained behavior change rather than one-off awareness sessions.

Evidence-Based Workplace Mental Health Interventions
Research consistently identifies specific interventions that demonstrate measurable impact on employee mental health outcomes. Organizations should prioritize evidence-based approaches to psychological health and safety rather than implementing fashionable but ineffective initiatives.
| Intervention Type | Primary Benefit | Implementation Complexity | Evidence Quality |
|---|---|---|---|
| Manager mental health training | Early intervention capacity | Moderate | Strong |
| Flexible work arrangements | Reduced stress, improved control | Low to Moderate | Strong |
| Job redesign for demands-control balance | Lower burnout rates | High | Strong |
| Peer support programs | Enhanced social connection | Moderate | Moderate |
| Organizational wellbeing assessments | Targeted strategy development | Low | Moderate to Strong |
Workplace wellbeing assessments provide essential baseline data that transforms generic approaches into targeted strategies. These assessments measure psychosocial hazards, organizational climate, and specific risk factors that vary significantly across industries, departments, and workforce demographics.
Trauma-Informed Workplace Practices
Trauma-informed care principles apply equally to workplace environments as to clinical settings. Organizations implementing trauma-informed approaches recognize that a substantial proportion of employees have experienced trauma and that workplace practices can either support healing or trigger re-traumatization.
Core principles of trauma-informed workplaces:
- Safety: Physical and psychological safety in all environments and interactions
- Trustworthiness: Transparent operations and consistent, reliable leadership behavior
- Peer support: Opportunities for connection and mutual support among colleagues
- Collaboration: Shared decision-making and genuine employee voice mechanisms
- Empowerment: Recognition of employee strengths and cultivation of skills
- Cultural sensitivity: Awareness of diverse backgrounds and responsive practices
These principles reshape everything from recruitment processes to performance management systems. Organizations trained in trauma-informed approaches report reduced conflict, improved retention, and stronger team cohesion.
Strategic Policy Development for Mental Health
Workplace strategies for mental health require formalization through policies that establish expectations, procedures, and accountability mechanisms. However, effective policies balance structure with flexibility, providing clear frameworks without rigid prescriptiveness that fails to account for individual circumstances.
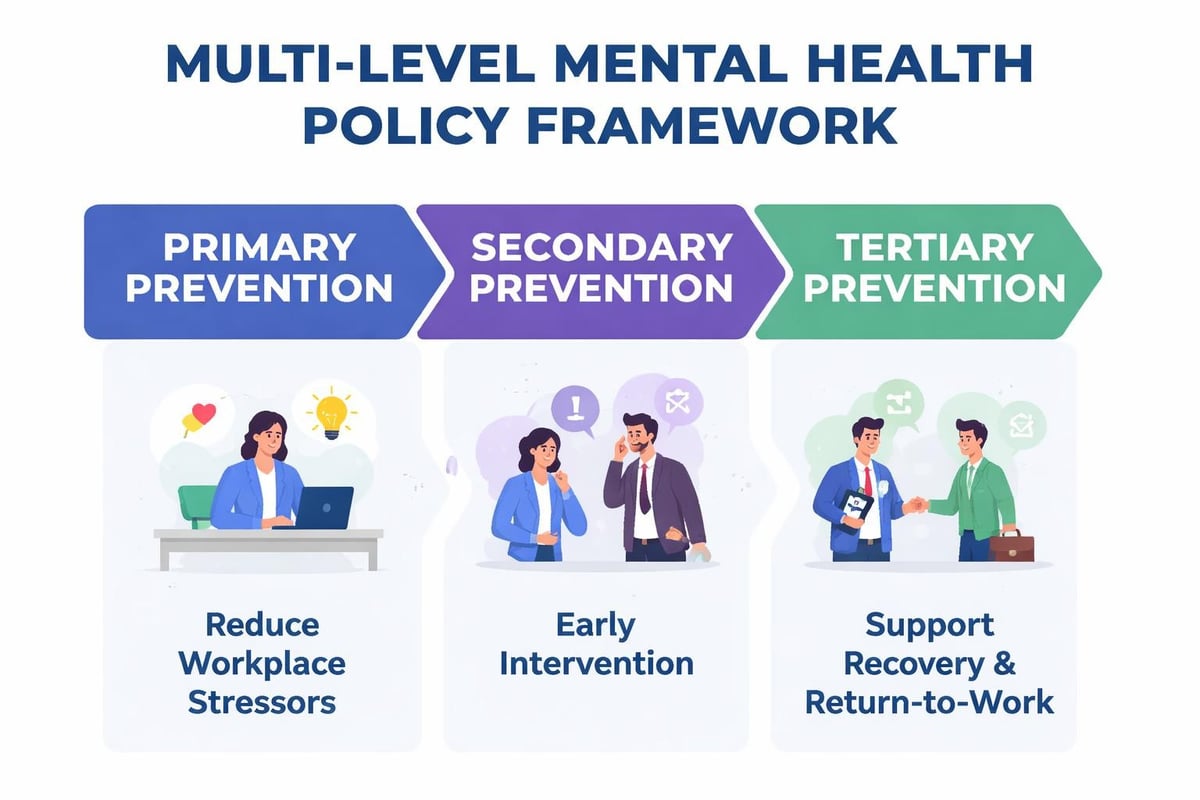
Mental health policies should address multiple levels of intervention. Primary prevention focuses on reducing risk factors and strengthening protective factors across the workforce. Secondary prevention emphasizes early identification and intervention for employees experiencing emerging difficulties. Tertiary prevention supports employees managing diagnosed conditions or recovering from mental health crises.
Creating Psychologically Safe Policies
Strategies for fostering a positive workplace culture extend beyond standalone mental health policies to encompass integrated approaches across all organizational systems. Return-to-work policies, performance management frameworks, and professional development pathways all carry mental health implications.
Consider how policies address common workplace stressors:
Workload management: Clear expectations about reasonable workloads, mechanisms for raising concerns about excessive demands, and regular reviews of resource allocation prevent chronic overwork that depletes mental resources.
Communication protocols: Boundaries around after-hours contact, meeting-free time blocks, and expectations for response times protect recovery periods essential for sustained wellbeing.
Leave entitlements: Generous and accessible leave provisions for mental health reasons, without stigmatizing language or burdensome approval processes, enable employees to seek support when needed.
Implementing Resilience-Building Programs
Resilience training represents a valuable component of comprehensive workplace strategies for mental health when implemented appropriately. However, resilience programs must complement rather than substitute for addressing organizational sources of stress. Individual resilience cannot compensate for toxic work environments or systemic dysfunction.
Effective resilience programs build specific psychological skills through structured learning and practice. These include cognitive flexibility, emotional regulation, problem-solving under pressure, and recovery strategies that prevent acute stress from becoming chronic strain.
Resilience Program Components
Programs should integrate multiple evidence-based approaches rather than relying on single methodologies. Organizational strategies to promote mental health and resilience emphasize combining individual skill development with supportive organizational practices.
- Cognitive reframing techniques: Identifying and challenging unhelpful thought patterns that amplify stress
- Mindfulness and attention regulation: Developing present-moment awareness and intentional focus
- Values clarification: Connecting daily work to deeper purpose and meaning
- Social connection skills: Building and maintaining supportive relationships
- Recovery practices: Deliberate strategies for physical and psychological restoration
Training delivery format significantly influences outcomes. Microlearning modules, practice-based workshops, and ongoing coaching or supervision demonstrate superior results compared to one-time seminars or passive e-learning.
Programs offered through platforms like WMHI Online provide structured learning pathways with practical application exercises that translate theoretical knowledge into behavioral change.
Measurement and Continuous Improvement
Workplace strategies for mental health require robust measurement frameworks that capture both process metrics and outcome indicators. Organizations should track implementation fidelity, participation rates, and employee perceptions alongside harder outcomes like absenteeism, turnover, and performance metrics.
| Metric Category | Example Indicators | Measurement Frequency |
|---|---|---|
| Process | Training completion rates, policy awareness | Quarterly |
| Perception | Psychological safety scores, manager support ratings | Biannually |
| Health outcomes | Reported stress levels, wellbeing indices | Annually |
| Organizational performance | Absenteeism rates, retention metrics, productivity | Monthly/Quarterly |
| Financial | Healthcare costs, workers compensation claims | Quarterly/Annually |
Leading indicators provide early signals about strategy effectiveness before lagging indicators like turnover or long-term absence rates reveal problems. Regular pulse surveys capture real-time employee sentiment and identify emerging concerns requiring immediate attention.
Data-Driven Strategy Refinement
Measurement serves strategy refinement rather than mere reporting compliance. Organizations should establish review cycles that examine data patterns, identify successful interventions worth expanding, and recognize ineffective approaches requiring modification or discontinuation.
Resources and strategies available through established platforms provide benchmarking opportunities that contextualize organizational data against industry standards. However, internal trends matter more than external comparisons, particularly in the early stages of strategy implementation.
Australian organizations can access specialized resources through WMHI Australia that account for regional regulatory frameworks and cultural contexts influencing workplace mental health approaches.
Specialized Considerations for High-Risk Environments
Certain industries and roles face elevated mental health risks requiring targeted workplace strategies beyond general approaches. Healthcare, emergency services, social services, and other high-stress sectors experience disproportionate rates of burnout, compassion fatigue, and trauma-related conditions.
High-risk environments benefit from specialized interventions addressing sector-specific stressors. These might include critical incident stress management protocols, regular psychological debriefing opportunities, and enhanced peer support networks with trained facilitators.
Supporting Frontline and Helping Professionals
Workers in helping professions require particular attention to vicarious trauma, moral injury, and emotional exhaustion resulting from sustained exposure to others’ suffering. Workplace strategies for mental health in these contexts emphasize containment strategies, professional boundaries, and regular clinical supervision.
Protective factors for high-risk roles:
- Reasonable caseloads that prevent chronic overextension
- Access to regular clinical or professional supervision
- Clear protocols for managing complex or high-risk situations
- Team debrief processes following critical incidents
- Structured rotation policies preventing prolonged exposure to highest-intensity work
Organizations should also prepare specialized response protocols for when employees experience acute crises. Suicide prevention skills training equips managers and colleagues to recognize warning signs and respond appropriately in potentially life-threatening situations.

Technology-Enabled Mental Health Support
Digital tools expand the reach and accessibility of workplace mental health strategies while introducing new considerations around privacy, equity, and effectiveness. Evidence-based digital interventions complement rather than replace human connection and organizational change efforts.
Innovative approaches to workplace mental health increasingly incorporate technology for early detection, real-time support, and scalable intervention delivery. However, organizations must carefully evaluate digital tools against criteria including evidence base, data security, accessibility, and integration with existing support systems.
Evaluating Digital Mental Health Tools
The proliferation of mental health apps and platforms requires discerning evaluation. Organizations should prioritize tools with published efficacy data, transparent privacy practices, and user experiences appropriate for their workforce demographics.
Selection criteria for digital mental health tools:
- Evidence base: Published research demonstrating effectiveness for target outcomes
- Clinical governance: Involvement of qualified mental health professionals in development
- Data security: Robust protections for sensitive personal information
- Accessibility: Compatibility with diverse abilities, devices, and connectivity levels
- Integration: Coordination with existing employee assistance programs and health services
- Personalization: Adaptive content responding to individual needs and preferences
Technology cannot address organizational culture issues or systemic workplace stressors. Digital tools work best as components of comprehensive strategies that simultaneously address individual, team, and organizational factors influencing mental health.
Integrating Mental Health into Business Operations
The most sustainable workplace strategies for mental health embed wellbeing considerations into core business processes rather than maintaining mental health as a separate initiative. This integration ensures consistency, reduces competing priorities, and reinforces the organizational value placed on employee wellbeing.
Mental health integration touches every business function. Human resources incorporates psychological safety into recruitment, onboarding, development, and exit processes. Operations considers mental health impacts when designing workflows, schedules, and physical environments. Finance allocates resources recognizing prevention as investment rather than cost.
Wellbeing-Informed Decision Making
Establishing wellbeing as a standard decision-making criterion transforms organizational culture. Major decisions undergo systematic analysis of potential mental health impacts, similar to financial or operational impact assessments.
This might involve asking structured questions during planning processes:
- How will this change affect employee workload and work-life balance?
- What support will employees need to adapt successfully?
- Does this decision align with our stated values around employee wellbeing?
- What are the potential unintended consequences for team psychological safety?
- How will we monitor and address any negative mental health impacts?
Organizations applying this lens consistently identify potential problems early and design more sustainable, human-centered solutions.
Addressing Stigma and Building Help-Seeking Culture
Even the most comprehensive workplace strategies for mental health fail when employees fear judgment, discrimination, or career consequences from seeking support. Stigma reduction requires sustained, multi-faceted efforts targeting attitudes, knowledge, and structural barriers simultaneously.
Effective anti-stigma approaches include:
- Senior leader disclosure and mental health advocacy
- Widespread education about mental health as normal human experience
- Visible celebration of recovery and help-seeking
- Strict enforcement of anti-discrimination protections
- Anonymous reporting mechanisms for stigma incidents
- Regular monitoring of help-seeking patterns across demographics
Language matters profoundly in stigma reduction. Organizations should adopt person-first language, avoid clinical labels in casual contexts, and emphasize strength and capability rather than deficit or dysfunction.
Research on workplace culture’s role in mental health demonstrates that supportive environments emerge from consistent messaging, modeled behavior, and genuine organizational responsiveness to employee needs.
Global Frameworks and Local Adaptation
International frameworks provide valuable guidance for developing workplace strategies for mental health while requiring thoughtful adaptation to local contexts. The WHO global plan of action for workers’ health establishes principles applicable across diverse settings while acknowledging cultural, economic, and regulatory variations.
Organizations operating across multiple jurisdictions face particular challenges balancing consistency with local relevance. Global mental health strategies establish minimum standards and shared principles while allowing regional customization addressing specific cultural norms, legal requirements, and workforce characteristics.
Cultural Competence in Mental Health Strategies
Cultural competence extends beyond awareness to actionable understanding of how cultural backgrounds shape mental health experiences, help-seeking behaviors, and intervention preferences. Workplace strategies must account for diverse perspectives on mental health, varied communication styles, and differential access to traditional support systems.
Inclusive mental health strategies involve employees from diverse backgrounds in design and delivery, ensuring programs resonate across the full workforce rather than reflecting dominant culture assumptions. This might include offering support in multiple languages, providing culturally specific resources, and partnering with community organizations serving particular employee populations.
Video resources available through Workplace Mental Health Institute’s YouTube channel demonstrate practical approaches to implementing culturally responsive mental health strategies across diverse organizational contexts.
Implementing effective workplace strategies for mental health requires sustained commitment, evidence-based approaches, and integration across all organizational systems. Success depends on leadership engagement, manager capability, supportive policies, and cultural transformation that positions employee wellbeing as fundamental to organizational performance. Workplace Mental Health Institute partners with organizations to develop comprehensive mental health training and resilience programs tailored to your specific workforce needs, delivering practical skills and measurable outcomes that enhance both employee wellbeing and organizational effectiveness.


