The landscape of organizational performance has shifted dramatically as research confirms what many leaders have long suspected: employee psychological health directly influences productivity, retention, and business outcomes. Mental wellbeing at work is no longer a peripheral concern relegated to annual awareness campaigns. It represents a strategic imperative that requires systematic intervention, informed leadership, and organizational commitment grounded in evidence rather than assumption.
Understanding Mental Wellbeing in Workplace Contexts
Mental wellbeing at work encompasses more than the absence of diagnosable mental health conditions. It reflects employees’ capacity to realize their potential, manage ordinary workplace stressors, maintain productive output, and contribute meaningfully to organizational goals.
The World Health Organization’s 2022 guidelines on mental health at work establish that workplace mental health exists on a continuum, influenced by organizational policies, management practices, work design, and psychosocial factors. Organizations that treat mental wellbeing as binary-either present or absent-miss the opportunity to create environments where employees consistently function at optimal psychological capacity.
Defining Core Components
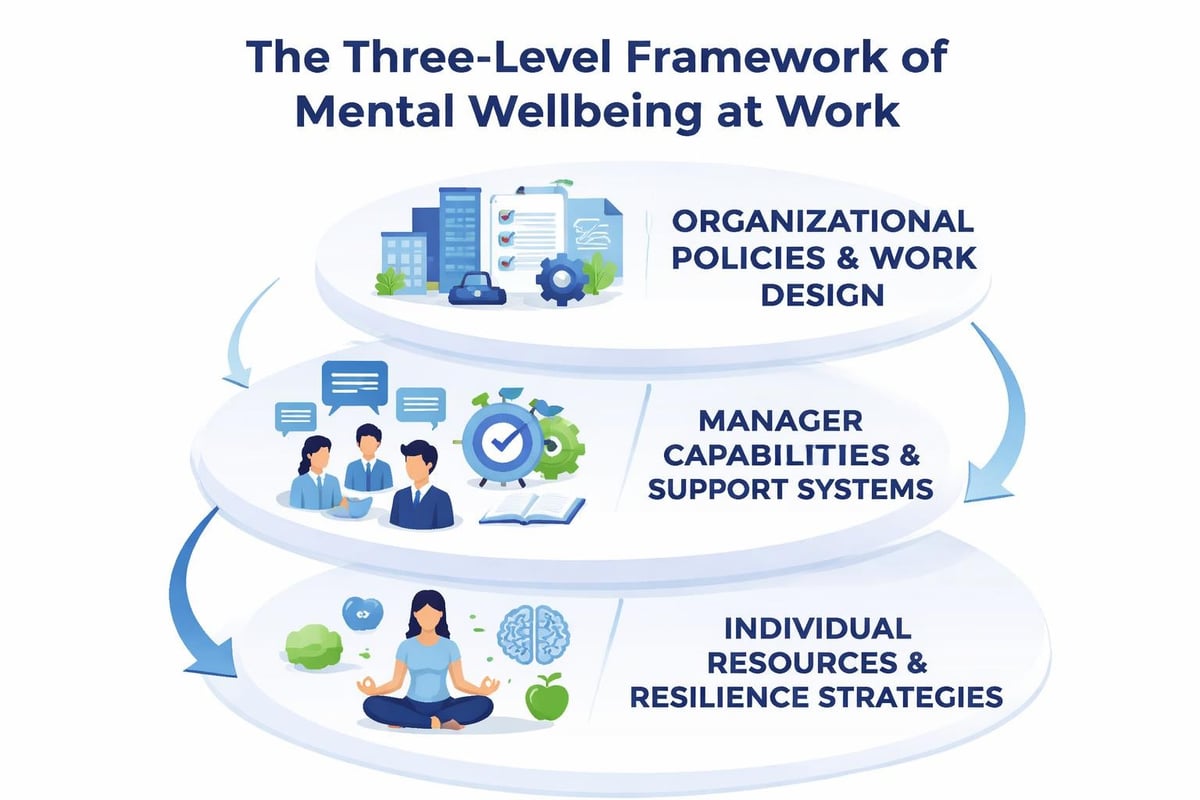
Effective approaches recognize three distinct but interconnected dimensions:
- Psychological safety: The assurance that interpersonal risks can be taken without fear of negative consequences to status or career
- Role clarity and autonomy: Clear expectations paired with appropriate decision-making authority
- Recognition and growth: Acknowledgment of contributions and access to developmental opportunities
These elements form the foundation upon which individual resilience and organizational support systems operate. Without addressing structural factors, individual interventions deliver diminished returns.
Identifying Psychosocial Risk Factors
Organizations serious about mental wellbeing at work must first understand what undermines it. Psychosocial risks in workplace settings include identifiable conditions that research has repeatedly linked to adverse mental health outcomes.
High-Risk Organizational Characteristics:
| Risk Category | Specific Manifestations | Impact on Wellbeing |
|---|---|---|
| Work Demands | Excessive workload, unrealistic deadlines, conflicting priorities | Chronic stress, burnout, anxiety |
| Control | Limited decision authority, rigid processes, micromanagement | Reduced autonomy, helplessness |
| Support | Inadequate manager training, unclear reporting structures, isolation | Increased vulnerability, poor recovery |
| Relationships | Bullying, discrimination, poor team dynamics | Psychological harm, disengagement |
| Role Issues | Ambiguous expectations, frequent restructuring, role conflict | Confusion, reduced efficacy |
| Change Management | Poor communication, inadequate consultation, unstable conditions | Uncertainty, mistrust |
The presence of multiple risk factors creates cumulative effects that exceed the sum of individual stressors. A 2023 systematic review examining workplace mental health antecedents confirms that organizations with comprehensive risk assessment processes identify problems earlier and implement more effective interventions.
Australian organizations can access specialized assessment frameworks through WMHI Australia that align with local workplace health and safety requirements while incorporating international best practices.
Assessment as Foundation
Workplace wellbeing assessments provide baseline data essential for targeted intervention. Effective assessments measure both organizational conditions and individual experiences, creating a complete picture of mental health risk and protective factors.
Regular measurement allows organizations to track intervention effectiveness, identify emerging concerns, and demonstrate accountability. Without measurement, wellbeing initiatives remain aspirational rather than operational.
Developing Manager Capability
Managers function as the primary interface between organizational policy and employee experience. Their actions, communication patterns, and responses to distress shape workplace culture more powerfully than formal programs.
Evidence on manager interventions demonstrates that training managers to recognize early warning signs, conduct supportive conversations, and make appropriate referrals produces measurable improvements in team mental health outcomes. However, manager training must extend beyond awareness to develop practical competencies.
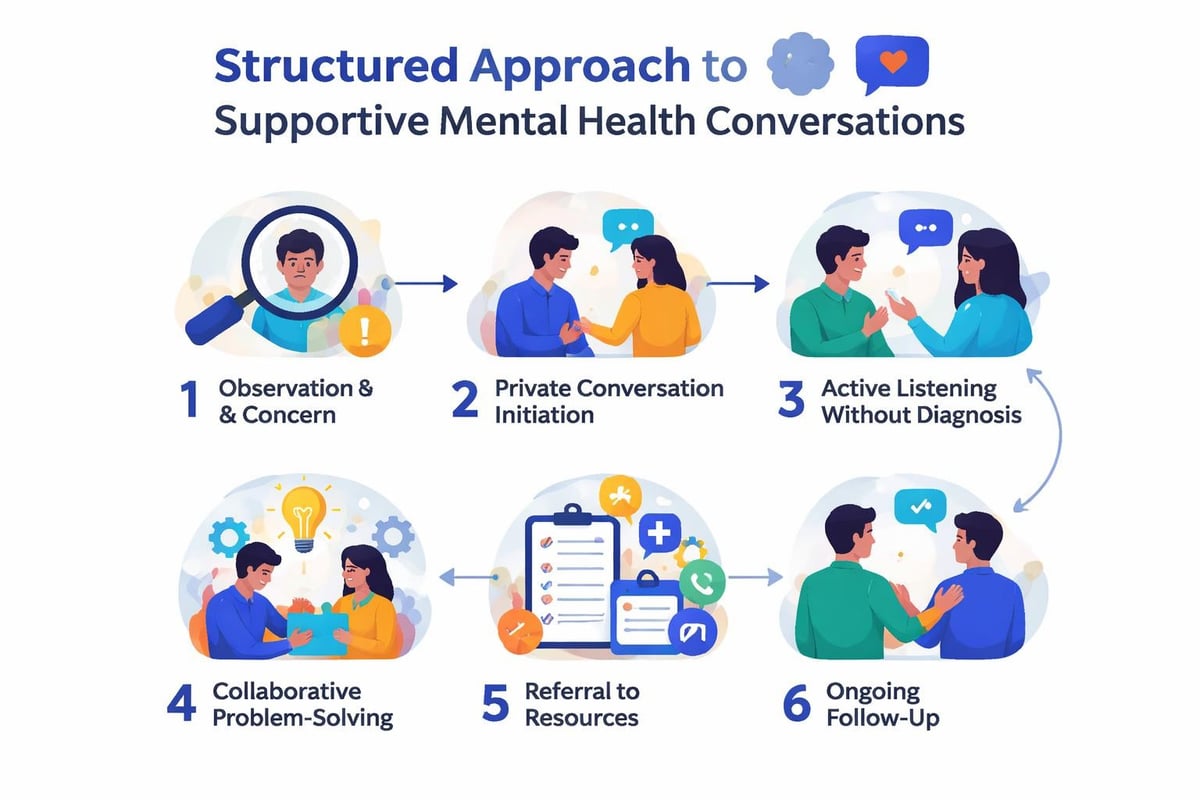
Essential Manager Competencies
- Recognizing changes in behavior or performance that may indicate declining mental wellbeing
- Initiating non-diagnostic conversations focused on support rather than clinical assessment
- Understanding reasonable adjustments and workplace accommodation options
- Maintaining appropriate boundaries between support and clinical intervention
- Accessing organizational resources and making effective referrals
Managers also require training in trauma-informed approaches, particularly in high-risk sectors or following critical incidents. Trauma-informed care training equips managers to respond to disclosure or crisis without causing additional harm through inappropriate questions or responses.
Implementing Organizational-Level Interventions
While individual support matters, organizational-level approaches address the conditions that protect or undermine mental wellbeing at work across entire workforces. These interventions modify work design, policies, and systems rather than attempting to increase individual resilience within dysfunctional environments.
Evidence-Based Organizational Strategies:
- Job redesign that increases autonomy and reduces excessive demands
- Flexible working arrangements that accommodate diverse needs
- Clear policies addressing bullying, harassment, and discrimination
- Structured return-to-work processes for employees recovering from mental health conditions
- Leadership accountability for wellbeing outcomes
Organizations frequently implement individual-level programs-such as mindfulness apps or resilience workshops-while neglecting fundamental organizational issues. This approach places responsibility for mental wellbeing entirely on employees rather than addressing systemic factors within leadership control.
Creating Supportive Structures
Effective organizational intervention requires coordinated action across multiple systems. Human resources policies, work design, performance management, and workplace culture must align to reinforce rather than contradict wellbeing objectives.
The WHO fact sheet on mental health at work emphasizes that supportive work environments benefit all employees, not just those currently experiencing mental health challenges. Universal design principles-creating conditions that support diverse needs-prove more effective than programs targeting specific groups.
Selecting Individual-Level Approaches
Individual interventions complement but cannot replace organizational action. These approaches help employees develop skills, access support, and manage mental health proactively.
Effective individual programs include:
- Employee Assistance Programs (EAPs): Confidential counseling services addressing personal and work-related concerns
- Skills-based training: Workshops on stress management, sleep hygiene, communication, or boundary-setting
- Peer support networks: Structured programs connecting employees with trained colleagues
- Digital mental health tools: Apps or platforms providing self-directed support between formal interventions
The Workplace Mental Health Institute offers comprehensive training programs that combine individual skill development with organizational capacity building, ensuring coordinated intervention across multiple levels.
Measuring Program Effectiveness
Organizations must evaluate whether interventions produce intended outcomes. Validated measures of worker wellbeing allow comparison across time and between organizational units, identifying what works and what requires adjustment.
| Measurement Approach | Purpose | Frequency |
|---|---|---|
| Engagement surveys | Track overall sentiment and identify risk areas | Quarterly or biannually |
| Absenteeism data | Monitor mental health-related leave patterns | Monthly |
| Turnover analysis | Identify retention issues linked to wellbeing | Quarterly |
| Program utilization | Assess uptake of support services | Ongoing |
| Focus groups | Gather qualitative insights on employee experience | Annually |
Data collection must respect privacy while providing sufficient detail for action. Aggregated reporting at team or department level balances confidentiality with actionable insight.
Addressing High-Risk Populations and Situations
Certain roles, industries, and employee groups experience elevated mental health risk. Targeted approaches acknowledge these differences while maintaining inclusive baseline support for all employees.
Risk-Specific Considerations
High-stress occupations-emergency services, healthcare, social services-require enhanced support structures including regular psychological screening, mandatory recovery time, and specialized trauma response protocols. Organizations in these sectors benefit from consulting services that design context-appropriate interventions rather than applying generic programs.
Employees with lived experience of mental health conditions need assurance that disclosure will not result in discrimination or career limitation. Clear policies, manager training, and demonstrable commitment from leadership create conditions where employees feel safe accessing support.
New employees, those experiencing major life transitions, and workers facing organizational change represent additional priority groups. Proactive outreach during these periods prevents escalation and demonstrates organizational commitment to mental wellbeing at work.
Building Psychologically Safe Cultures
Culture represents the accumulated patterns of behavior, communication, and decision-making that define organizational life. Psychological safety-the shared belief that the workplace is safe for interpersonal risk-taking-forms the foundation of mentally healthy cultures.
Leaders create psychological safety through consistent modeling of vulnerability, acknowledgment of mistakes, invitation of dissenting views, and visible support for employees who raise concerns. These behaviors signal that perfection is not expected and that challenges can be discussed openly.
NICE guidelines on creating supportive work environments emphasize senior leadership responsibility for establishing and maintaining cultures where mental wellbeing receives equivalent attention to physical safety and operational performance.
Practical Culture-Building Actions
Organizations move beyond statements of intent through:
- Regular leadership communication that normalizes mental health discussions
- Resource allocation demonstrating tangible commitment beyond policy documents
- Integration of wellbeing metrics into performance dashboards alongside financial and operational data
- Accountability mechanisms ensuring managers fulfill wellbeing responsibilities
- Celebration of positive examples where individuals or teams exemplify supportive practices
Culture change requires sustained effort over years rather than months. Organizations should expect gradual progress measured through improved engagement scores, reduced mental health-related absence, and increased help-seeking behavior.
Integrating Strategic Consultation
Organizations implementing comprehensive approaches to mental wellbeing at work benefit from external expertise that brings cross-industry perspective, current research knowledge, and specialized assessment capabilities.
Strategic consultation helps organizations:
- Conduct baseline assessments identifying specific risk factors and gaps
- Design intervention strategies aligned with organizational context and resources
- Train managers and leaders in evidence-based practices
- Establish measurement frameworks tracking progress toward wellbeing objectives
- Adjust approaches based on evaluation data and changing organizational needs
The Workplace Mental Health Institute provides specialized consultation services that move beyond generic recommendations to develop tailored strategies reflecting organizational size, industry risk factors, workforce demographics, and existing capabilities.
Consultation proves particularly valuable during periods of significant change, following critical incidents, or when internal data indicates declining mental health trends. External consultants offer objectivity and specialized knowledge that internal teams may lack.
Preventing Burnout Through Work Design
Burnout-characterized by exhaustion, cynicism, and reduced professional efficacy-results primarily from chronic workplace stressors rather than individual deficits. Prevention requires addressing the six areas of work-life that research identifies as burnout risk factors.
Burnout Risk Areas and Interventions:
| Risk Area | Contributing Factors | Protective Interventions |
|---|---|---|
| Workload | Excessive demands, inadequate resources | Realistic goal-setting, adequate staffing |
| Control | Limited autonomy, micromanagement | Delegated authority, participation in decisions |
| Reward | Insufficient recognition, poor compensation | Regular acknowledgment, fair pay structures |
| Community | Conflict, lack of support, isolation | Team development, collaboration opportunities |
| Fairness | Discrimination, favoritism, unclear processes | Transparent systems, consistent application |
| Values | Misalignment between personal and organizational ethics | Values clarification, ethical decision processes |
Addressing burnout requires organizational intervention rather than individual resilience programs. While personal coping strategies provide temporary relief, sustainable prevention demands modification of work conditions.
Developing Resilience Programs
Resilience programs teach practical skills that help employees navigate adversity, recover from setbacks, and maintain wellbeing during challenging periods. Effective programs focus on modifiable factors rather than suggesting employees simply work harder or think more positively.
Evidence-based resilience training covers:
- Cognitive flexibility: Recognizing and reframing unhelpful thought patterns
- Emotional regulation: Managing intense emotions without suppression or avoidance
- Problem-solving skills: Breaking complex challenges into manageable components
- Social connection: Building and maintaining supportive relationships
- Meaning and purpose: Connecting daily work to broader values and goals
Resilience programs work best when embedded within broader organizational efforts to reduce psychosocial risks. Teaching employees coping skills while maintaining excessive workloads or poor management practices creates unrealistic expectations and may increase distress.
Organizations can access resilience programs specifically designed for workplace contexts that integrate individual skill development with team-based activities and manager involvement.
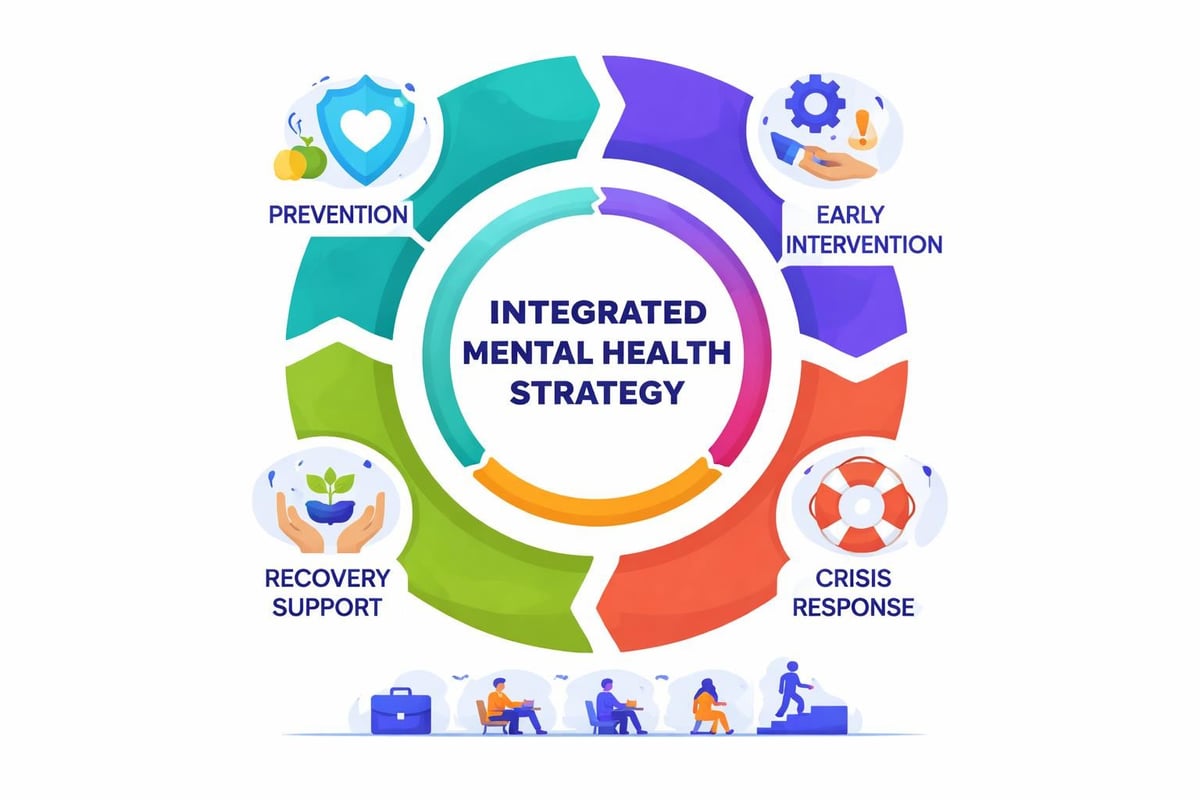
Establishing Crisis Response Protocols
Despite preventive efforts, mental health crises occur. Organizations require clear protocols ensuring rapid, appropriate responses that prioritize safety while respecting dignity.
Effective crisis protocols include:
- Clear escalation pathways so employees and managers know who to contact
- Trained response team capable of assessing risk and coordinating support
- Links to emergency services including mental health crisis teams
- Communication guidelines balancing confidentiality with need-to-know information
- Follow-up procedures supporting return to work after crisis resolution
Crisis response extends to supporting team members affected by a colleague’s mental health emergency. Managers need guidance on what to communicate, how to maintain operations during absences, and how to welcome employees back without intrusive questions.
Regular training ensures protocols remain current and response teams maintain competency. Annual reviews identify gaps and incorporate lessons from previous incidents.
Supporting Return to Work
Employees recovering from mental health conditions benefit from structured return-to-work processes that allow graduated reintegration rather than immediate resumption of full duties. Supportive return-to-work programs reduce recurrence risk and demonstrate organizational commitment to employee wellbeing.
Key elements include:
- Pre-return planning meetings involving employee, manager, and HR
- Graduated hours or duties allowing adjustment before full workload resumes
- Workplace accommodations addressing specific needs without requiring disclosure of diagnosis
- Regular check-ins monitoring adjustment and addressing concerns early
- Clear documentation protecting employee rights while ensuring consistent treatment
Return-to-work support must extend beyond the initial weeks. Some employees require ongoing accommodations or periodic adjustments as they manage chronic conditions while maintaining employment.
Visual resources from the Workplace Mental Health Institute YouTube channel provide managers with practical guidance on conducting return-to-work conversations and implementing supportive transitions.
Maintaining Confidentiality While Providing Support
Employees often hesitate to seek help due to confidentiality concerns. Organizations must establish clear policies delineating what information is shared, with whom, and under what circumstances.
Best practices include:
- Separating clinical information (held by health providers) from workplace accommodation details (shared with managers)
- Training managers to support employees without requiring diagnostic disclosure
- Establishing secure systems for health-related documentation
- Communicating confidentiality protections clearly and repeatedly
- Addressing breaches promptly and seriously
Managers require specific guidance on responding when employees disclose mental health information. The goal is providing appropriate support and accommodation while respecting privacy and avoiding intrusive questions about clinical details.
Organizations that prioritize mental wellbeing at work through evidence-based, multilevel interventions create environments where employees thrive and business outcomes improve. These strategies require sustained commitment, but deliver measurable returns in productivity, retention, and organizational reputation. The Workplace Mental Health Institute partners with organizations to assess current approaches, design tailored interventions, and build internal capability through comprehensive training programs that transform mental health from a compliance requirement into a strategic advantage.


