Understanding mental health is essential for everyone, from young people navigating their first experiences with stress to professionals managing workplace pressures and older adults addressing life transitions. This comprehensive mental health question and answer guide addresses the most frequently asked questions across all age groups, providing clear, evidence-based responses that empower individuals to take meaningful action. Whether you’re seeking information for yourself, a family member, or your workplace, these answers offer practical insights grounded in current research and best practices.
Understanding Mental Health Fundamentals
Mental health encompasses our emotional, psychological, and social wellbeing, affecting how we think, feel, and act in daily life. Many people struggle to distinguish between normal stress responses and conditions requiring professional support.
What’s the difference between mental health and mental illness?
Mental health exists on a spectrum that everyone experiences throughout their lifetime. Just as physical health fluctuates, mental health changes based on circumstances, stress levels, and life events. Mental illness refers to diagnosed conditions that significantly impact thinking, mood, or behavior and interfere with daily functioning. You can have periods of poor mental health without having a mental illness, and conversely, people with diagnosed conditions can experience periods of strong mental wellbeing with proper support and treatment.
How do I know if I need professional help?
Several indicators suggest it’s time to seek professional support:
- Persistent symptoms lasting more than two weeks that don’t improve
- Functional impairment affecting work performance, relationships, or daily activities
- Physical symptoms like changes in sleep patterns, appetite, or energy levels
- Overwhelming feelings of sadness, anxiety, or hopelessness
- Withdrawal from activities or people you previously enjoyed
- Difficulty concentrating or making decisions
Professional help isn’t reserved only for crisis situations. Early intervention often prevents conditions from worsening and leads to better outcomes. SAMHSA provides comprehensive information about when and how to seek mental health services.

Mental Health Question and Answer for Young People
Adolescents and young adults face unique mental health challenges as they navigate identity formation, academic pressures, and social relationships. These questions reflect the most common concerns in this age group.
Why do I feel anxious about things that don’t bother my friends?
Anxiety manifests differently for everyone due to individual brain chemistry, past experiences, and genetic factors. What feels overwhelming to you might not register as stressful for someone else, and this variation is completely normal. Your sensitivity isn’t a weakness but rather reflects how your unique nervous system processes information. Many young people benefit from learning coping strategies like deep breathing, progressive muscle relaxation, and cognitive reframing to manage anxiety effectively.
Is it normal to feel sad sometimes, or does that mean I’m depressed?
Sadness is a normal human emotion that everyone experiences in response to disappointment, loss, or difficult situations. Depression, however, involves persistent low mood combined with other symptoms that last for weeks or months. The key differences include:
| Normal Sadness | Depression |
|---|---|
| Tied to specific events | Pervasive regardless of circumstances |
| Improves within days | Lasts two weeks or longer |
| Doesn’t prevent daily activities | Interferes with school, work, relationships |
| Responds to support from friends | May not improve with typical support |
If sadness persists and interferes with your life, speaking with a school counselor or mental health professional provides clarity and support.
Can social media affect my mental health?
Research consistently shows that excessive social media use correlates with increased anxiety, depression, and poor sleep quality, particularly among teenagers. The comparison culture, cyberbullying, and constant connectivity can overwhelm developing brains. Setting boundaries like designated phone-free times, curating your feed to include positive content, and prioritizing in-person connections helps protect mental wellbeing while still enjoying social media’s benefits.
Workplace Mental Health Questions
Workplace mental health has become increasingly important as organizations recognize the connection between employee wellbeing and productivity. These mental health question and answer pairs address common workplace concerns.
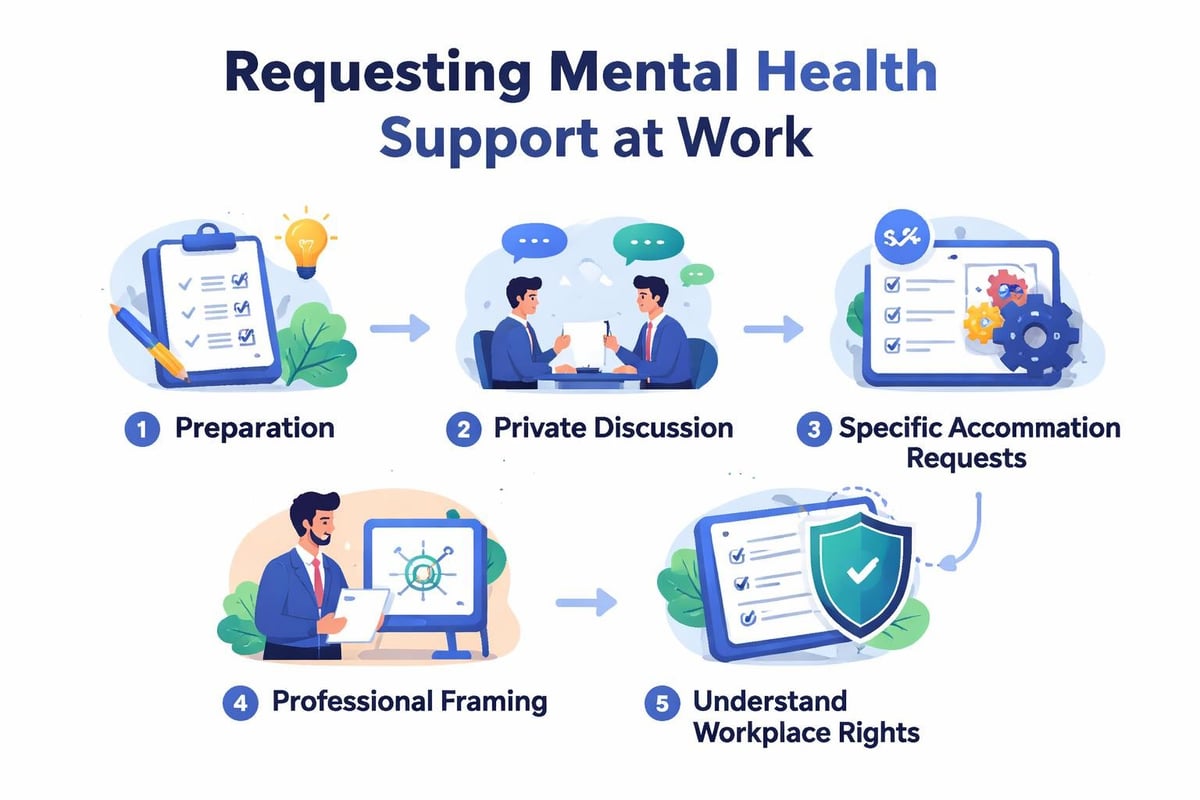
How can I talk to my manager about mental health struggles?
Approaching your manager requires preparation and clarity about what support you need. Consider these steps:
- Schedule a private meeting rather than bringing it up spontaneously
- Focus on specific accommodations you’re requesting rather than detailed diagnoses
- Frame it professionally by emphasizing your commitment to your work
- Know your rights regarding workplace accommodations and privacy
- Prepare documentation if requesting formal accommodations
You’re not obligated to disclose specific diagnoses, but explaining how you’re affected and what adjustments would help demonstrates professionalism while protecting your privacy. Many organizations now offer employee assistance programs specifically designed to support mental health needs.
What if my workplace doesn’t take mental health seriously?
Unfortunately, not all organizations prioritize mental health equally. If your workplace lacks adequate support, several options exist:
- Utilize external resources like personal therapy or community mental health services
- Connect with HR to understand available benefits you might not know about
- Build peer support by connecting with colleagues facing similar challenges
- Document concerns if you feel discrimination occurs based on mental health
- Advocate for change by suggesting training programs or policy improvements
Organizations that invest in comprehensive mental health training often see reduced absenteeism and improved team performance. Advocating for such programs benefits everyone in the workplace.
How do I manage burnout without quitting my job?
Burnout results from chronic workplace stress that hasn’t been successfully managed, characterized by exhaustion, cynicism, and reduced professional efficacy. Recovery requires multiple strategies:
Immediate actions:
- Set firm boundaries between work and personal time
- Take regular breaks throughout the day
- Prioritize sleep and physical activity
- Use vacation time for genuine rest
Longer-term solutions:
- Evaluate workload distribution with your supervisor
- Identify aspects of your role that energize you and increase them
- Develop skills for stress management and resilience
- Consider whether your current role aligns with your values
Burnout indicates a mismatch between job demands and available resources. Addressing it requires both personal coping strategies and potential workplace adjustments.
Mental Health Question and Answer for Parents and Caregivers
Parents frequently worry about their children’s mental health while managing their own wellbeing. These questions reflect common parental concerns across different developmental stages.
How do I know if my child’s behavior is normal or a mental health concern?
Children express distress differently than adults, often through behavioral changes rather than verbal communication. Warning signs vary by age but generally include:
- Regression to earlier developmental behaviors (bedwetting, separation anxiety)
- Academic decline not explained by learning difficulties
- Social withdrawal from friends or previously enjoyed activities
- Physical complaints without medical explanation
- Extreme reactions that seem disproportionate to situations
- Changes in eating or sleeping patterns lasting more than two weeks
Trust your instincts as a parent. If something feels off, consulting your pediatrician or a child mental health professional provides peace of mind and early intervention if needed. Beyond Blue offers guidance on finding credible mental health information to support these conversations.
Should I talk to my kids about mental health even if they seem fine?
Absolutely. Proactive mental health conversations normalize the topic and make children more likely to seek help when they need it. Just as you discuss physical health, nutrition, and safety, mental health deserves regular attention. Approach these conversations naturally by:
- Sharing age-appropriate information about emotions and coping
- Modeling healthy stress management in your own life
- Asking open-ended questions about their feelings regularly
- Reading books or watching shows that address mental health themes together
- Creating a judgment-free environment for discussing difficult topics
These ongoing conversations build emotional literacy and resilience that serve children throughout their lives.
Questions About Specific Mental Health Conditions
Understanding specific conditions helps people recognize symptoms in themselves or others and seek appropriate support. This mental health question and answer section addresses common diagnostic questions.
What’s the difference between anxiety and an anxiety disorder?
Everyone experiences anxiety as a normal response to stress or perceived threats. This adaptive emotion helps us stay safe and perform well under pressure. An anxiety disorder, however, involves excessive, persistent worry that occurs even without real danger and significantly interferes with daily life. Anxiety disorders include generalized anxiety disorder, social anxiety, panic disorder, and specific phobias.
The clinical threshold is reached when anxiety:
- Persists for six months or longer
- Causes significant distress or impairment
- Doesn’t respond to normal coping strategies
- Occurs in situations that don’t warrant such intense reactions
Treatment typically involves therapy (particularly cognitive-behavioral therapy), lifestyle modifications, and sometimes medication, all of which prove highly effective for most people.
Can you have depression and anxiety at the same time?
Yes, depression and anxiety frequently co-occur, affecting approximately 60% of people with either condition. This combination, sometimes called “mixed anxiety-depressive disorder,” presents unique challenges because symptoms can compound each other. The worry characteristic of anxiety can contribute to depressive rumination, while the low energy of depression can make anxiety feel more overwhelming.
Fortunately, many treatments effectively address both conditions simultaneously. Cognitive-behavioral therapy, for instance, teaches skills applicable to both anxiety and depression. Understanding that these conditions often overlap helps people seek comprehensive treatment rather than addressing only one aspect of their mental health.
Is ADHD just difficulty focusing, or is it more complex?
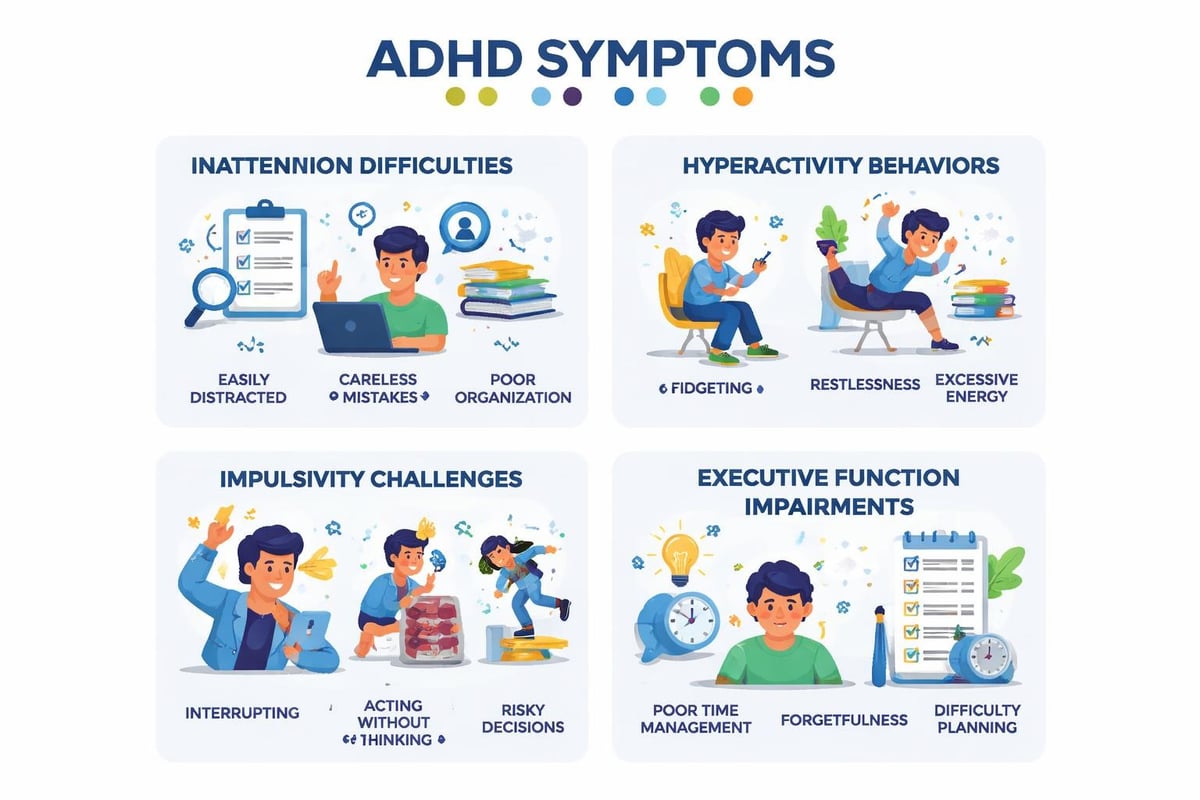
Attention-deficit/hyperactivity disorder (ADHD) extends far beyond occasional focus problems. This neurodevelopmental condition affects executive functioning, the brain’s management system controlling planning, organization, time management, emotional regulation, and impulse control. ADHD presents in three types: predominantly inattentive, predominantly hyperactive-impulsive, and combined presentation.
| ADHD Symptom Category | Examples |
|---|---|
| Inattention | Difficulty sustaining focus, frequent careless mistakes, losing items, forgetfulness |
| Hyperactivity | Fidgeting, difficulty staying seated, excessive talking, feeling restless |
| Impulsivity | Interrupting others, difficulty waiting turns, making decisions without considering consequences |
| Executive Dysfunction | Poor time management, difficulty prioritizing, emotional dysregulation |
ADHD affects people across the lifespan, though symptoms may change with age. Adults with ADHD often struggle with workplace organization, relationship management, and completing tasks despite strong capabilities.
Mental Health Questions for Older Adults
Mental health needs evolve throughout life, and older adults face distinct challenges related to retirement, health changes, and loss. These questions address common concerns in this population.
Is memory loss a normal part of aging or a mental health issue?
Some cognitive changes accompany normal aging, including occasional difficulty finding words, slower processing speed, and needing more time to learn new information. However, significant memory loss that interferes with daily functioning isn’t a normal part of aging and warrants medical evaluation.
Concerning signs include:
- Forgetting recently learned information frequently
- Difficulty completing familiar tasks
- Confusion about time or place
- Changes in judgment or decision-making
- Withdrawal from work or social activities
- Mood and personality changes
Depression, anxiety, medication side effects, vitamin deficiencies, and thyroid problems can all cause memory difficulties that improve with treatment. Early evaluation distinguishes between treatable conditions and progressive disorders, allowing for timely intervention.
Why do I feel depressed after retiring when I should be happy?
Retirement represents a major life transition that affects identity, daily structure, social connections, and purpose. Many retirees experience unexpected depression as they adjust to these changes. This reaction is common and doesn’t mean something is wrong with you.
Contributing factors include:
- Loss of work-related identity and purpose
- Reduced social interaction from workplace relationships
- Financial concerns or adjustment to fixed income
- Physical health changes becoming more apparent
- Grief over this life stage ending
Building a new routine, cultivating social connections, engaging in meaningful activities, and maintaining physical health all support mental wellbeing during this transition. If depressive symptoms persist beyond six months or feel overwhelming, professional support helps navigate this adjustment more smoothly.
Finding Reliable Mental Health Information
With abundant mental health information available online, distinguishing credible sources from misinformation is crucial. The CDC provides comprehensive data sources that inform evidence-based mental health discussions.
How do I evaluate mental health information I find online?
Reliable mental health information shares several characteristics:
Source credibility:
- Published by established organizations, universities, or government agencies
- Written or reviewed by qualified mental health professionals
- Contains citations to peer-reviewed research
- Clearly states funding sources and potential conflicts of interest
Content quality:
- Provides balanced information rather than promoting single solutions
- Acknowledges complexity and individual variation
- Updated recently (within the past three years for general information)
- Uses clear language without excessive jargon
- Distinguishes opinion from evidence-based facts
Organizations like Ventura Counseling & Wellness Center outline effective strategies for identifying reliable mental health resources that support informed decision-making.
When should I trust my own experience over expert information?
Both personal experience and expert knowledge contribute valuable perspectives on mental health. Your lived experience provides irreplaceable insights into what works for your unique situation, while expert information offers evidence-based approaches that help many people. The most effective approach integrates both.
Trust your experience when:
- A recommended treatment doesn’t feel right for you after giving it a fair try
- Your symptoms don’t match typical descriptions but still cause distress
- Cultural or personal factors make standard advice less applicable
Seek expert guidance when:
- Your situation feels unmanageable despite self-help efforts
- You’re making important treatment decisions
- Symptoms worsen or don’t improve with initial strategies
- You need help distinguishing normal variation from clinical concerns
The best mental health care happens through collaborative relationships where professionals provide expertise while respecting your knowledge of yourself.
Supporting Others with Mental Health Challenges
Many people want to help loved ones struggling with mental health issues but feel uncertain about the right approach. These questions address common concerns about providing support.
What should I say to someone who’s struggling with their mental health?
Supportive conversations focus on listening, validating feelings, and offering practical help rather than trying to fix problems or provide solutions. Effective approaches include:
- “I’ve noticed you seem [observation]. I’m concerned about you.” Opens conversation without assumptions
- “That sounds really difficult. Thank you for telling me.” Validates their experience
- “What would be most helpful right now?” Empowers them to identify needs
- “I’m here for you, whatever you need.” Offers ongoing support
- “Would you like help finding someone to talk to?” Suggests professional support without pressure
Avoid minimizing phrases like “just think positive,” “others have it worse,” or “you’ll get over it,” which invalidate genuine struggles and create distance.
How do I help without becoming overwhelmed myself?
Supporting someone with mental health challenges can be emotionally draining, making self-care essential for sustainable support. Establish clear boundaries around:
Time and availability:
- Communicate when you’re available to talk and when you need personal time
- Don’t sacrifice your own mental health trying to be constantly available
- Encourage multiple sources of support rather than being their only confidant
Emotional capacity:
- Recognize you’re not responsible for fixing their problems
- Practice compassion while maintaining emotional boundaries
- Seek your own support through friends, therapy, or support groups
Practical help:
- Offer specific assistance you can realistically provide
- Know your limits and don’t overcommit
- Share responsibility with other supporters when possible
Remember that professional mental health providers exist specifically because supporting mental health challenges requires specialized training and emotional distance that friends and family members can’t always provide.
Can I force someone to get help if they refuse?
Generally, you cannot force competent adults to seek mental health treatment unless they pose immediate danger to themselves or others. However, several approaches can encourage voluntary help-seeking:
- Express specific concerns using concrete examples of changed behaviors
- Explain impact on relationships or functioning without blame
- Offer to help with appointment scheduling, transportation, or accompaniment
- Provide information about available resources without pressure
- Set boundaries about behaviors you can’t tolerate while maintaining relationship
If someone poses imminent danger through suicidal intent or plans to harm others, emergency intervention becomes necessary. Contact crisis services, emergency services, or take them to an emergency room for immediate evaluation.
Accessing Mental Health Support and Resources
Understanding how to access appropriate mental health support empowers people to take action when needed. This final mental health question and answer section addresses practical access questions.
How do I find a mental health professional who’s right for me?
Finding the right mental health provider often requires trying several options. Consider these factors:
Practical considerations:
- Insurance coverage and cost
- Location and availability
- Specialization in your specific concerns
- Preferred treatment approach (medication, therapy type, holistic methods)
Personal fit:
- Communication style that feels comfortable
- Cultural competency and understanding of your background
- Gender preference if relevant
- Therapeutic relationship quality (should feel safe and understood)
Don’t hesitate to interview potential providers or try several before committing long-term. The therapeutic relationship significantly impacts outcomes, so finding someone you trust and connect with matters enormously.
What’s the difference between psychiatrists, psychologists, counselors, and therapists?
Mental health professionals have different training, credentials, and approaches:
| Professional | Education | Primary Focus | Prescribing Rights |
|---|---|---|---|
| Psychiatrist | Medical degree (MD/DO) plus psychiatry residency | Diagnosis and medication management | Yes |
| Psychologist | Doctoral degree (PhD/PsyD) in psychology | Psychological testing and therapy | Limited (in some states) |
| Licensed Counselor/Therapist | Master’s degree in counseling or social work | Psychotherapy and counseling | No |
| Psychiatric Nurse Practitioner | Nursing degree plus psychiatric specialization | Assessment and medication management | Yes |
Many people benefit from combined care, such as a psychiatrist for medication management and a therapist for regular counseling. Your primary care provider can help determine which professional(s) best suit your needs.
Are mental health apps and online therapy as effective as in-person treatment?
Digital mental health resources vary widely in quality and effectiveness. Research shows that evidence-based online therapy programs can be as effective as in-person treatment for certain conditions, particularly mild to moderate anxiety and depression. However, several factors influence appropriateness:
When digital resources work well:
- Mild to moderate symptoms without crisis risk
- High motivation for self-directed work
- Limited access to in-person services
- Preference for flexibility and convenience
- Supplementing in-person treatment
When in-person treatment is better:
- Severe symptoms or crisis situations
- Complex diagnoses requiring comprehensive assessment
- Need for medication management
- Preference for face-to-face connection
- Limited technology access or comfort
Many people benefit from combining approaches, using apps for daily skill practice while maintaining regular therapy appointments for deeper work.
Mental health question and answer resources provide valuable starting points for understanding and addressing mental health concerns across all life stages. Whether you’re navigating personal challenges, supporting loved ones, or managing workplace wellbeing, access to accurate information empowers informed decisions and effective action. The Workplace Mental Health Institute offers comprehensive training programs that equip managers and employees with practical mental health skills, creating psychologically safe workplaces where everyone can thrive. Their evidence-based approaches to workplace mental health reduce stigma, improve performance, and build resilient teams prepared to support mental wellbeing at every level.


