The landscape of workplace mental health has evolved dramatically, with organizations recognizing that investing in behavioral health training represents both an ethical imperative and a strategic business decision. As mental health challenges continue affecting workforce productivity and employee wellbeing, leaders face increasing pressure to develop competencies that extend beyond traditional management skills. Behavioral health training equips professionals with evidence-based tools to recognize psychological distress, respond appropriately to mental health crises, and create environments where psychological safety becomes the foundation for high performance.
Understanding Behavioral Health Training in Professional Contexts
Behavioral health training encompasses systematic education focused on understanding, recognizing, and responding to mental health conditions, substance use disorders, and psychological wellbeing factors within organizational settings. Unlike clinical training designed for healthcare providers, workplace-focused programs emphasize practical application for managers, HR professionals, and employees who support colleagues experiencing psychological challenges.
The Agency for Healthcare Research and Quality defines behavioral health broadly to include mental health and substance use services, providing a framework that helps organizations understand the scope of training requirements. This comprehensive approach ensures professionals develop competencies across multiple dimensions rather than focusing narrowly on crisis intervention alone.
Core Components That Define Effective Programs
Successful behavioral health training programs integrate several foundational elements that distinguish them from generic mental health awareness sessions:
- Theoretical foundations grounded in psychological research and clinical evidence
- Skill-based practice with realistic scenarios and role-playing exercises
- Cultural competency addressing diverse populations and intersectional identities
- Legal and ethical frameworks clarifying boundaries and responsibilities
- Self-care strategies preventing burnout among those supporting others
Organizations seeking comprehensive solutions should evaluate whether programs address these components systematically rather than superficially. The depth of content directly correlates with participant confidence and capability when applying knowledge in real-world situations.

Evidence-Based Approaches to Workplace Mental Health Education
Research consistently demonstrates that structured behavioral health training produces measurable outcomes when programs incorporate adult learning principles and experiential methodologies. Leaders benefit most from interactive formats that challenge assumptions, build empathy, and develop practical judgment rather than memorizing diagnostic criteria or clinical terminology.
Trauma-Informed Care as a Training Foundation
Trauma-informed approaches have emerged as essential frameworks within modern behavioral health training, recognizing that adverse experiences shape behavior, relationships, and workplace interactions. This perspective shifts focus from “what’s wrong with this person” to “what happened to this person,” fundamentally changing how managers interpret and respond to challenging behaviors.
Training in trauma-informed principles teaches professionals to:
- Recognize trauma’s widespread impact on employee populations
- Identify signs and symptoms of trauma responses in workplace contexts
- Integrate knowledge about trauma into policies and procedures
- Actively resist re-traumatization through thoughtful practices
- Build organizational cultures emphasizing safety and trustworthiness
The Behavioral Health Institute at the University of Washington offers resources demonstrating how trauma-informed frameworks apply across diverse professional settings. Organizations implementing these principles report improved employee engagement, reduced conflict, and enhanced psychological safety metrics.
Psychological First Aid and Crisis Response Skills
Behavioral health training must prepare workplace leaders to respond effectively during acute mental health crises while recognizing professional limitations. Psychological first aid provides a structured approach for initial support following traumatic events or during acute distress, emphasizing human connection over clinical intervention.
| Training Component | Traditional Approach | Evidence-Based Approach |
|---|---|---|
| Crisis identification | Waiting for obvious signs | Recognizing early warning indicators |
| Initial response | Offering generic advice | Providing psychological first aid |
| Referral process | Suggesting “get help” | Facilitating specific resource connections |
| Follow-up support | Assuming professionals handle it | Maintaining appropriate contact |
| Documentation | Minimal or excessive | Balanced, confidential record-keeping |
Programs that teach these distinctions help managers navigate the complex space between supportive leadership and inappropriate clinical intervention. Clear boundaries protect both employees and organizations while ensuring individuals receive appropriate care.
Building Organizational Capacity Through Systematic Training
Organizations achieve sustainable mental health outcomes when behavioral health training extends beyond isolated workshops to become integrated into professional development frameworks. This systematic approach requires careful planning, resource allocation, and ongoing evaluation to ensure training translates into meaningful behavioral change.
Developing Manager Competencies in Mental Health Conversations
Managers consistently report anxiety about initiating mental health conversations, fearing they’ll say the wrong thing or overstep professional boundaries. Effective behavioral health training addresses this discomfort directly through structured conversation frameworks and supervised practice opportunities.
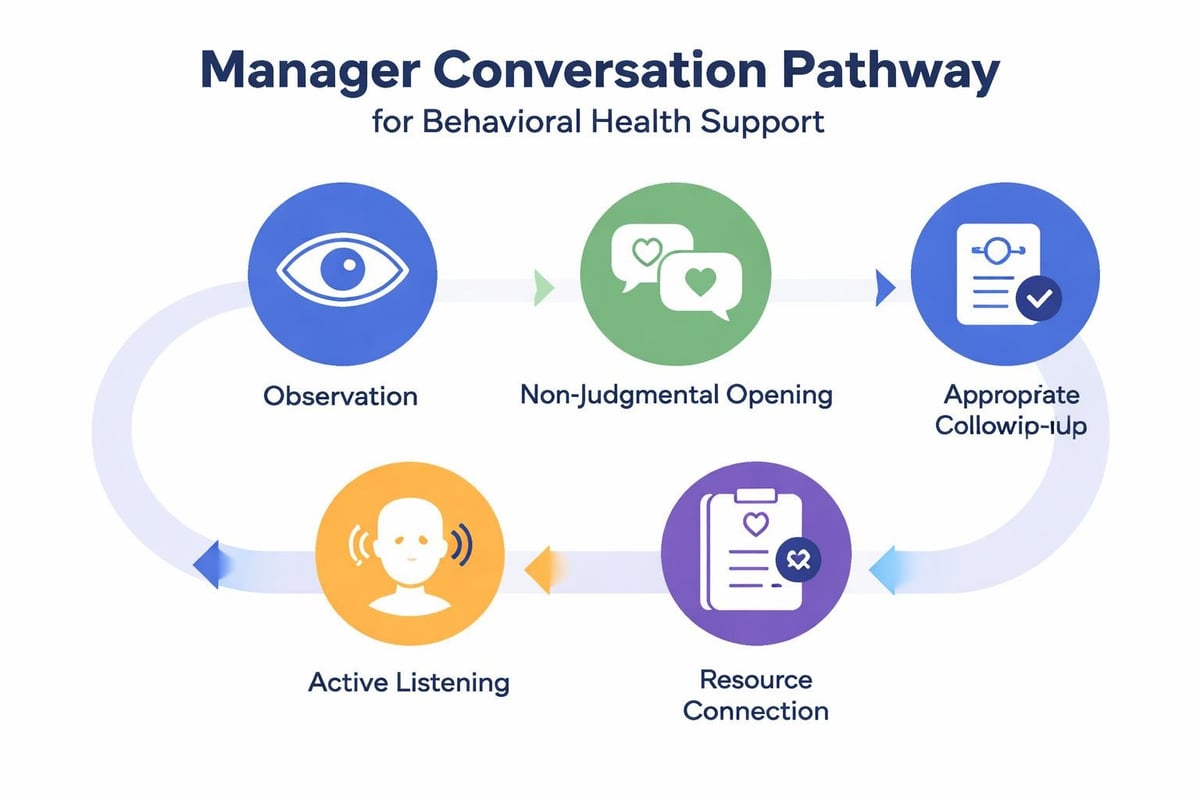
Research-backed training programs teach managers to:
- Open conversations using non-judgmental, observation-based statements
- Listen actively without attempting to diagnose or solve psychological problems
- Ask questions that clarify support needs rather than probe clinical details
- Connect employees with appropriate resources while maintaining confidentiality
- Follow up appropriately without creating surveillance or pressure
The Workplace Mental Health Institute specializes in building these competencies through practical, scenario-based training that reflects real workplace challenges. Participants develop confidence through guided practice rather than abstract theory alone.
Creating Peer Support Networks Through Targeted Education
Peer support represents a powerful complement to formal behavioral health services, with trained colleagues providing relatable assistance that reduces stigma and increases help-seeking behavior. Behavioral health training for peer supporters differs from manager-focused programs, emphasizing lived experience validation and boundary maintenance.
Effective peer support training covers:
- Foundational knowledge about common mental health conditions and recovery principles
- Communication skills specific to non-clinical, experience-based support
- Boundary awareness preventing inappropriate relationships or clinical overreach
- Self-care practices protecting peer supporters from vicarious trauma
- Resource knowledge enabling effective referrals to professional services
Recent developments in AI-assisted peer support, such as those explored in research on PeerCoPilot, demonstrate how technology can enhance rather than replace human connection in peer support contexts. Training programs should address both traditional and emerging support modalities.
Measuring Training Effectiveness and Organizational Impact
Organizations investing in behavioral health training require clear metrics demonstrating return on investment and program effectiveness. Evaluation frameworks should extend beyond participant satisfaction to measure behavioral application, organizational culture shifts, and business outcomes.
Assessment Strategies for Knowledge and Skill Development
Comprehensive evaluation begins with measuring whether participants actually acquired intended knowledge and skills. Pre- and post-training assessments reveal learning gains, while delayed assessments determine knowledge retention over time.
Effective measurement approaches include:
- Knowledge tests covering key concepts and frameworks
- Skill demonstrations through role-play assessments
- Case study analyses revealing applied judgment
- Self-efficacy ratings tracking confidence changes
- Behavioral observation in workplace settings
The research resources compiled by Arizona State University provide access to validated assessment instruments that organizations can adapt for their specific behavioral health training initiatives. Using established measures enhances credibility and enables benchmarking against broader datasets.
Organizational Metrics Linking Training to Business Outcomes
Leadership teams require evidence connecting behavioral health training investments to tangible organizational benefits. Effective measurement frameworks track both leading indicators (cultural shifts, help-seeking behavior) and lagging indicators (absenteeism, turnover, performance metrics).
| Metric Category | Specific Indicators | Measurement Timeline |
|---|---|---|
| Engagement | Help-seeking rates, EAP utilization | Monthly tracking |
| Performance | Productivity scores, quality metrics | Quarterly analysis |
| Retention | Voluntary turnover, tenure patterns | Annual evaluation |
| Wellbeing | Stress assessments, safety perceptions | Bi-annual surveys |
| Costs | Healthcare utilization, workers’ compensation | Annual review |
Organizations should establish baseline measurements before implementing behavioral health training, enabling accurate assessment of program impact. Research on risk assessment models like HARBOR illustrates how sophisticated analytics can predict outcomes and guide resource allocation in behavioral health contexts.
Addressing Implementation Challenges and Workforce Development
Despite growing recognition of behavioral health training’s importance, organizations face significant implementation barriers ranging from resource constraints to cultural resistance. Successful programs anticipate these challenges and develop strategic responses that build sustainable capacity.
Overcoming Stigma and Cultural Barriers
Workplace cultures often inadvertently discourage mental health disclosure through subtle messages about strength, resilience, and professional expectations. Behavioral health training must address these cultural factors explicitly rather than assuming education alone changes deeply embedded attitudes.
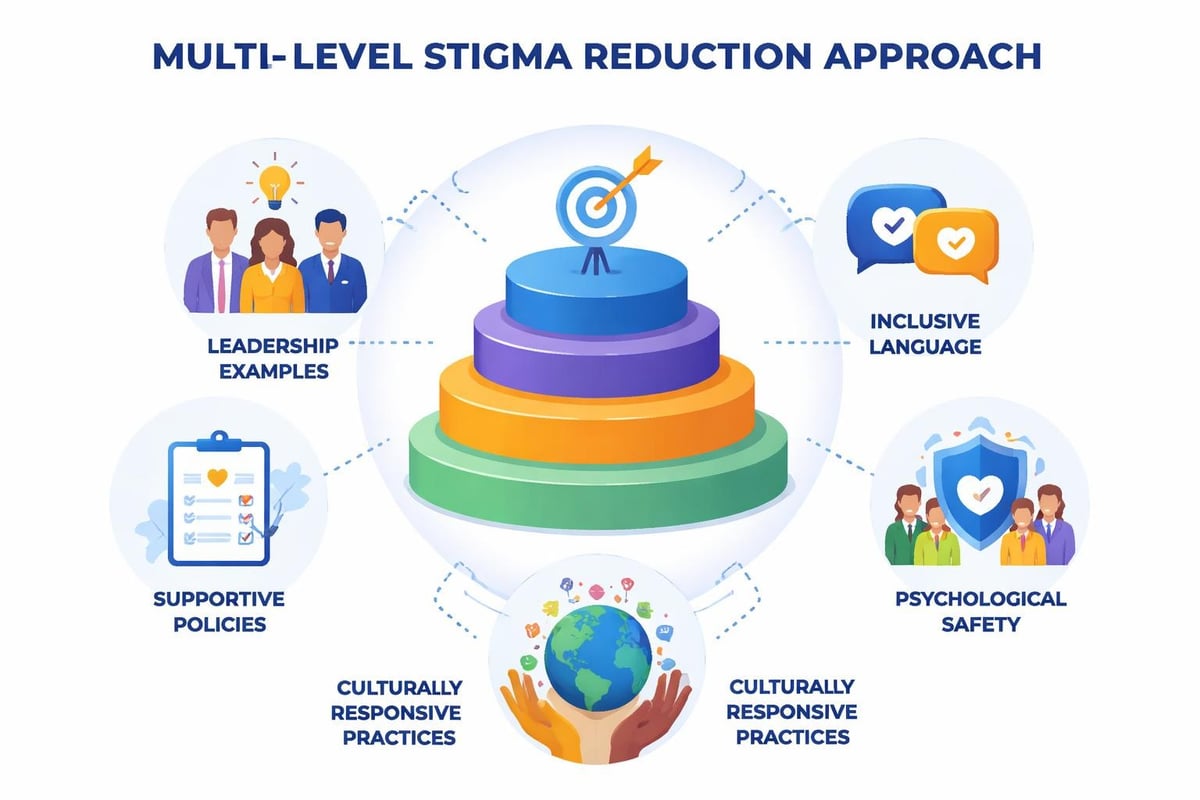
Strategic approaches include:
- Leadership modeling where executives share appropriate mental health experiences
- Language audits identifying and replacing stigmatizing terminology
- Policy alignment ensuring HR practices support rather than contradict training messages
- Psychological safety building creating conditions where vulnerability feels acceptable
- Inclusive design ensuring training reflects diverse cultural perspectives and experiences
Organizations serving diverse populations benefit from resources like those available through Australian Workplace Mental Health Institute programs, which address cultural factors specific to different regional and demographic contexts.
Building Sustainable Training Infrastructure
One-time workshops rarely produce lasting organizational change. Sustainable behavioral health training requires infrastructure supporting ongoing learning, skill reinforcement, and program evolution as organizational needs change.
Infrastructure elements include:
- Trainer development creating internal capacity to deliver programs consistently
- Resource libraries providing ongoing access to tools, templates, and reference materials
- Community practices facilitating peer learning and problem-solving among trained professionals
- Refresher mechanisms ensuring skills remain current through periodic updates
- Integration systems embedding training content into onboarding, performance reviews, and leadership development
The framework for implementing behavioral health training programs provides detailed guidance on building these sustainable systems, particularly in contexts addressing workforce shortages and capacity constraints.
Specialized Training for Diverse Professional Roles
Behavioral health training requirements vary significantly across organizational roles, with frontline employees, middle managers, and senior leaders needing different competencies. Effective programs differentiate content and delivery methods based on role-specific responsibilities and decision-making authority.
Frontline Employee Education and Resilience Building
Frontline staff benefit most from behavioral health training focused on personal resilience, peer support skills, and basic mental health literacy. These programs emphasize self-awareness, stress management, and recognizing when to seek professional support rather than diagnostic knowledge or intervention skills.
Training priorities for frontline employees:
- Recognizing personal stress responses and early warning signs
- Implementing evidence-based stress reduction techniques
- Supporting colleagues through empathetic listening and resource sharing
- Accessing organizational mental health resources confidently
- Maintaining work-life boundaries that protect wellbeing
Programs targeting this audience should use accessible language, emphasize practical application, and create safe environments for sharing challenges without fear of professional consequences.
Executive and Senior Leader Strategic Competencies
Senior leaders require behavioral health training that enables strategic decision-making about organizational mental health investments, policy development, and culture shaping. While basic mental health literacy remains important, executive programs emphasize business case development, systems thinking, and resource allocation strategies.
Executive training should address:
- Quantifying mental health’s impact on organizational performance and profitability
- Developing comprehensive wellbeing strategies aligned with business objectives
- Allocating resources effectively across prevention, intervention, and support services
- Modeling psychological safety and vulnerability-based leadership
- Evaluating vendor proposals and program quality standards
Organizations can explore advanced strategic training through Workplace Mental Health Institute online courses, which provide flexible learning options for busy executives requiring evidence-based guidance without extensive time commitments.
Regulatory and Professional Standards Shaping Training Requirements
Behavioral health training increasingly operates within frameworks established by regulatory bodies, professional associations, and accreditation organizations. Understanding these standards helps organizations ensure compliance while developing programs that meet recognized quality benchmarks.
Professional Credentialing and Certification Pathways
Certain behavioral health roles require specific training credentials, particularly positions involving direct service delivery or clinical consultation. The role of licensed behavior analysts illustrates how professional standards define educational requirements, supervised experience, and ongoing competency maintenance.
Organizations should clarify whether positions require:
- Specific professional licenses or certifications
- Continuing education in behavioral health topics
- Supervision by credentialed mental health professionals
- Documented competency in particular intervention models
- Ethical training addressing confidentiality and boundaries
These requirements vary by jurisdiction, organizational context, and role responsibilities. HR professionals developing position descriptions benefit from consulting regulatory guidelines specific to their location and industry.
Ethical Considerations in Workplace Mental Health Training
Behavioral health training must address ethical complexities that emerge when colleagues provide mental health support within hierarchical workplace structures. Power dynamics, confidentiality limits, and dual relationship risks require explicit discussion rather than implicit assumptions about appropriate behavior.
Key ethical topics include:
| Ethical Domain | Training Content | Practice Application |
|---|---|---|
| Confidentiality | Legal limits and organizational policies | Knowing when information must be shared |
| Boundaries | Professional vs. personal relationships | Maintaining appropriate distance while caring |
| Competence | Scope of practice and referral obligations | Recognizing when professional help is needed |
| Documentation | What to record and how to protect records | Balancing accountability with privacy |
| Dual relationships | Managing multiple roles with same person | Avoiding conflicts of interest |
Training that addresses these considerations reduces organizational liability while protecting both employees seeking support and colleagues providing assistance. Clear ethical frameworks enable confident action rather than avoidance driven by uncertainty.
Integrating Technology and Digital Learning Platforms
Digital transformation has expanded behavioral health training access while creating new quality assurance challenges. Organizations must evaluate technology-enhanced programs carefully, ensuring convenience doesn’t compromise learning effectiveness or practical skill development.
Advantages and Limitations of Online Training Delivery
Virtual behavioral health training offers significant benefits including geographic accessibility, scheduling flexibility, and cost efficiency. However, certain competencies require in-person practice and interpersonal feedback that purely digital formats struggle to replicate effectively.
Online training works well for:
- Knowledge acquisition covering theoretical concepts and research findings
- Self-paced learning accommodating diverse schedules and learning speeds
- Global team access ensuring consistent training across distributed workforces
- Resource efficiency reducing travel and facility costs
- Multimedia engagement using video, interactive modules, and varied formats
In-person training excels at:
- Skill practice requiring real-time feedback and coaching
- Emotional connection building empathy through direct interaction
- Complex scenario navigation with nuanced judgment development
- Trust building creating psychological safety for vulnerable sharing
- Immediate question resolution addressing confusion as it emerges
Optimal approaches often combine both modalities, using online platforms for knowledge transfer while reserving in-person sessions for skill application and relationship building. Organizations can explore this blended approach through video resources available at the Workplace Mental Health Institute YouTube channel, which supplements formal training with accessible educational content.
Quality Standards for Digital Behavioral Health Education
As digital training proliferates, organizations need criteria for evaluating program quality and effectiveness. Not all online behavioral health training delivers equivalent outcomes, with significant variation in evidence base, instructional design, and learner support.
Evaluation criteria should include:
- Evidence foundation documenting research supporting content and methods
- Instructional design incorporating adult learning principles and engagement strategies
- Skill practice opportunities providing application beyond passive content consumption
- Assessment rigor measuring actual learning rather than completion alone
- Technical accessibility ensuring platforms work across devices and connection speeds
- Support availability offering assistance when learners encounter difficulties
Organizations committed to quality should request evidence demonstrating these elements before committing to digital behavioral health training platforms.
Future Directions in Workplace Mental Health Education
The field of behavioral health training continues evolving rapidly, with emerging research, technological capabilities, and workforce expectations shaping program development. Organizations positioning themselves for long-term success monitor these trends while maintaining focus on evidence-based fundamentals.
Personalization and Adaptive Learning Technologies
Emerging technologies enable behavioral health training customization based on individual learning needs, prior knowledge, and role-specific requirements. Adaptive platforms adjust content difficulty, pacing, and practice opportunities based on learner performance, potentially improving both efficiency and outcomes.
Personalization advantages include:
- Accelerated learning for participants with relevant background knowledge
- Additional support for learners requiring more time with complex concepts
- Role-specific content prioritization focusing on most relevant competencies
- Learning path recommendations based on assessment results and goals
- Engagement improvements through appropriately challenging material
However, personalization requires sophisticated technology infrastructure and careful design to avoid creating fragmented learning experiences that sacrifice shared organizational knowledge.
Integrating Behavioral Health Across Organizational Systems
Leading organizations recognize that isolated behavioral health training produces limited impact without corresponding changes in policies, procedures, and performance expectations. Future approaches emphasize integration, embedding mental health considerations throughout organizational systems rather than treating wellbeing as a separate initiative.
Integration strategies include:
- Performance management incorporating psychological safety and wellbeing behaviors
- Leadership selection emphasizing mental health competencies alongside traditional criteria
- Risk assessment integrating behavioral health factors into operational planning
- Communication training including mental health conversation skills as core competencies
- Change management addressing psychological impact of organizational transitions
This systems-level approach requires behavioral health training for diverse stakeholder groups rather than concentrating education solely within HR or wellness departments. Sustainable culture change emerges when mental health competencies become expected across all professional roles and organizational levels.
Behavioral health training represents a strategic investment that protects both human wellbeing and organizational performance when designed with evidence-based rigor and delivered systematically across professional roles. Organizations seeking to develop comprehensive capabilities benefit from partnering with specialists who understand both clinical foundations and workplace application. Workplace Mental Health Institute provides tailored training programs, strategic consultation, and ongoing support that builds sustainable mental health competency throughout your organization, equipping leaders and employees with practical skills that translate directly into improved workplace outcomes.


