Mental illness and the workplace represent two spheres that organizations can no longer afford to keep separate. With one in five adults experiencing mental illness annually, the likelihood that your workforce includes employees managing psychiatric conditions is statistical certainty rather than possibility. The question for leaders and human resources professionals is not whether mental illness exists within your organization, but how effectively your systems, policies, and culture support those who are navigating these challenges while contributing to organizational success.
Understanding Mental Illness in Organizational Contexts
Mental illness encompasses a broad spectrum of conditions affecting mood, thinking, and behavior. These include depression, anxiety disorders, bipolar disorder, post-traumatic stress disorder, schizophrenia, and numerous other diagnosable conditions that significantly impact daily functioning.
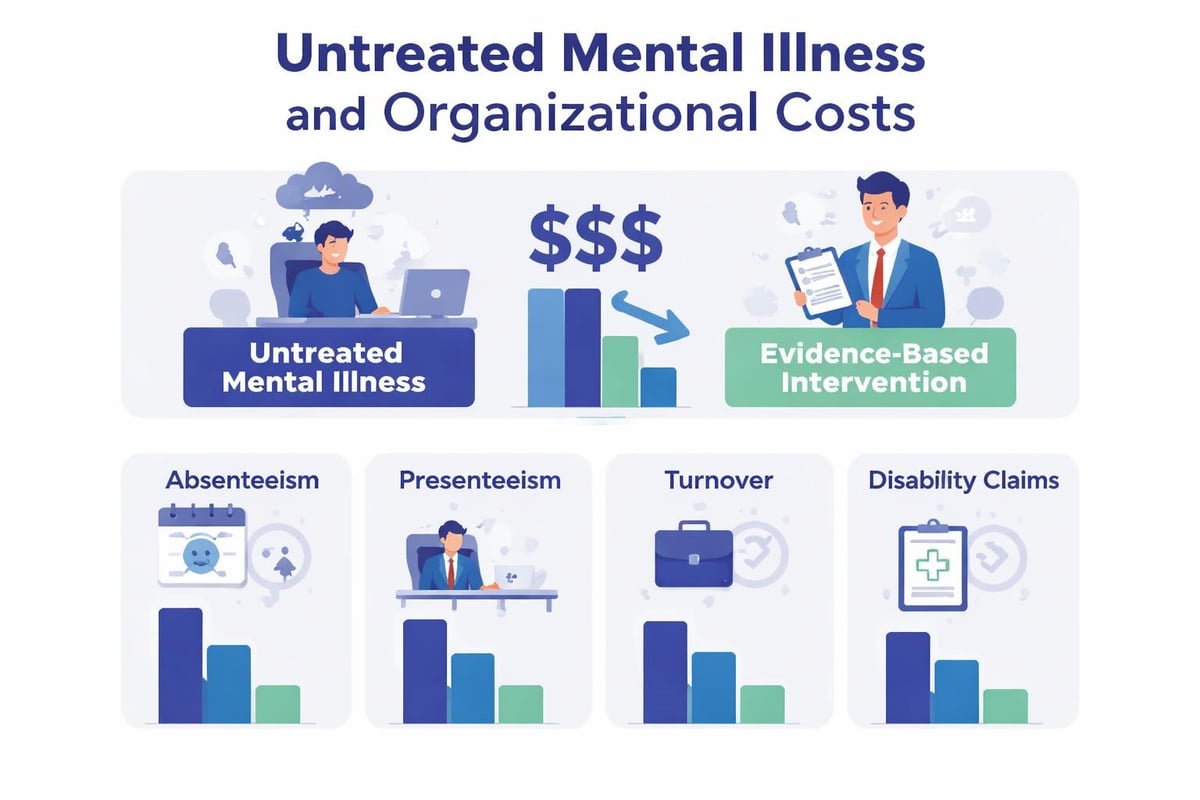
The workplace implications extend far beyond individual experience. Research on mental illness prevalence demonstrates that psychiatric conditions cost organizations billions annually through reduced productivity, increased absenteeism, and higher healthcare expenditures.
Prevalence and Economic Impact
Consider these essential data points for strategic planning:
- Approximately 20% of working adults experience mental illness in any given year
- Depression and anxiety alone cost the global economy $1 trillion annually in lost productivity
- Employees with untreated mental health conditions have 7-12 more disability days per year
- Presenteeism (reduced on-the-job performance) often exceeds absenteeism costs by three-fold
Organizations that treat mental health as a strategic priority rather than an individual problem see measurable returns. Studies consistently demonstrate that comprehensive workplace mental health programs deliver $4 in improved health and productivity for every $1 invested.
The Disclosure Dilemma and Psychological Safety
The challenges surrounding disclosure of mental illness represent one of the most complex dynamics in modern workplaces. Employees face difficult calculations when deciding whether to disclose psychiatric conditions to managers or colleagues.
This decision involves weighing potential benefits against very real risks:
Potential Benefits:
- Access to workplace accommodations
- Reduced need to hide symptoms or treatment
- Opportunity for schedule flexibility
- Connection with supportive colleagues
Perceived Risks:
- Discrimination in advancement opportunities
- Changed perceptions of competence
- Informal exclusion from projects or decisions
- Termination or constructive dismissal
Research examining workers’ perspectives on disclosure reveals that employer response patterns heavily influence whether disclosure leads to positive or negative outcomes. Organizations with established psychological safety, clear accommodation processes, and trained managers see significantly better disclosure experiences.
Creating Disclosure-Safe Environments
Building cultures where employees feel safe discussing mental health requires systematic attention to multiple organizational layers:
- Policy frameworks that explicitly protect employees from discrimination based on mental health conditions
- Manager training that equips supervisors with response protocols and reduces harmful reactions
- Accommodation processes that are clear, confidential, and consistently applied
- Leadership modeling that normalizes mental health discussions through appropriate self-disclosure
The objective is not to pressure disclosure but to ensure that when employees choose to share, they encounter supportive rather than punishing responses. Organizations can explore comprehensive approaches through Workplace Mental Health Institute training programs designed specifically for manager capability development.
Strategic Accommodation and Job Performance
Mental illness and the workplace intersect most visibly in accommodation requests and performance management scenarios. Effective organizations distinguish between supporting employees and compromising operational standards.
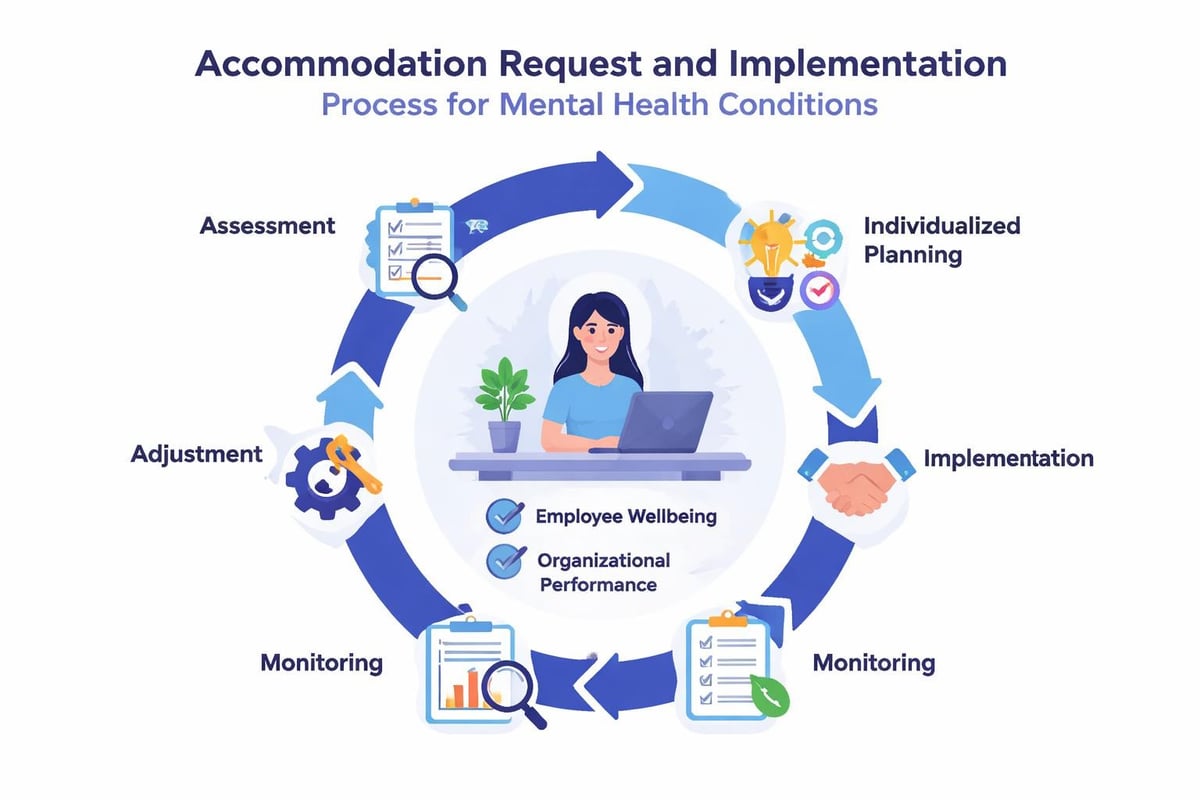
Evidence-Based Accommodation Strategies
| Accommodation Type | Mental Health Application | Implementation Considerations |
|---|---|---|
| Schedule flexibility | Attend therapy appointments, manage medication timing | Core hours with variable start/end times |
| Modified break schedules | Manage anxiety symptoms, prevent burnout | Structured breaks with clear coverage protocols |
| Quiet workspace options | Reduce sensory overwhelm, improve concentration | Hot-desking systems with reserved quiet zones |
| Remote work arrangements | Reduce commute stress, manage symptoms | Clear deliverables with outcome-based evaluation |
| Temporary workload adjustment | Support during acute episodes, prevent deterioration | Time-limited with structured return-to-full-capacity plans |
The most effective accommodations are individualized, time-bound, and linked to specific functional limitations rather than diagnostic labels. An employee with depression might need schedule modifications during a depressive episode but function without accommodation during stable periods.
Mental health accommodations often cost less than physical disability accommodations while delivering substantial retention benefits. The CDC’s guidance on workplace mental health emphasizes that early intervention through reasonable accommodation prevents more costly disability claims and turnover.
Manager Capability as Foundation
Frontline managers serve as the primary interface between organizational mental health policy and employee experience. Yet most managers receive minimal preparation for these responsibilities.
Core Manager Competencies
Effective support for employees experiencing mental illness requires managers to develop specific, trainable capabilities:
- Recognition skills to identify potential mental health concerns through performance or behavior changes
- Conversation frameworks that express concern without diagnosing or overstepping professional boundaries
- Referral knowledge to connect employees with appropriate internal and external resources
- Accommodation implementation abilities to translate medical recommendations into practical workplace adjustments
- Confidentiality management to protect employee privacy while coordinating necessary support
Organizations can access structured manager development through programs at WMHI Online, which provide practical frameworks rather than clinical training.
The distinction matters. Managers are not therapists and should not attempt clinical intervention. Instead, they create conditions where employees can access professional help while maintaining employment stability.
Addressing Stigma Through Systems Change
Stigma operates at three distinct levels within organizations, each requiring different intervention approaches:
Public Stigma
Negative attitudes and discriminatory behaviors directed toward people with mental illness by others in the workplace. This manifests through exclusion from informal networks, skepticism about capabilities, and attribution of performance issues to character rather than health.
Self-Stigma
Internalized negative beliefs that employees with mental illness hold about themselves, leading to reduced help-seeking, lower career aspirations, and decreased self-efficacy.
Structural Stigma
Organizational policies, practices, and norms that inadvertently disadvantage employees with mental health conditions, such as rigid attendance policies that penalize medical appointments or promotion criteria that reward unsustainable work patterns.
Effective stigma reduction targets all three levels simultaneously rather than focusing exclusively on attitude change campaigns. Comprehensive workplace mental health research demonstrates that structural changes often drive cultural shifts more effectively than awareness programs alone.
| Stigma Level | Ineffective Approach | Evidence-Based Approach |
|---|---|---|
| Public | Annual awareness email | Manager training with accountability metrics |
| Self | Inspirational posters | Peer support programs with lived experience |
| Structural | Existing policies assumed adequate | Policy audit with mental health equity lens |
Organizations in Australia can access specialized regional expertise through WMHI Australia for locally relevant approaches.
Performance Management and Mental Illness
Mental illness and the workplace create tension points in performance management systems. Organizations must maintain legitimate performance standards while acknowledging that mental health conditions can temporarily affect job performance.
Distinguishing Performance Issues from Health Conditions
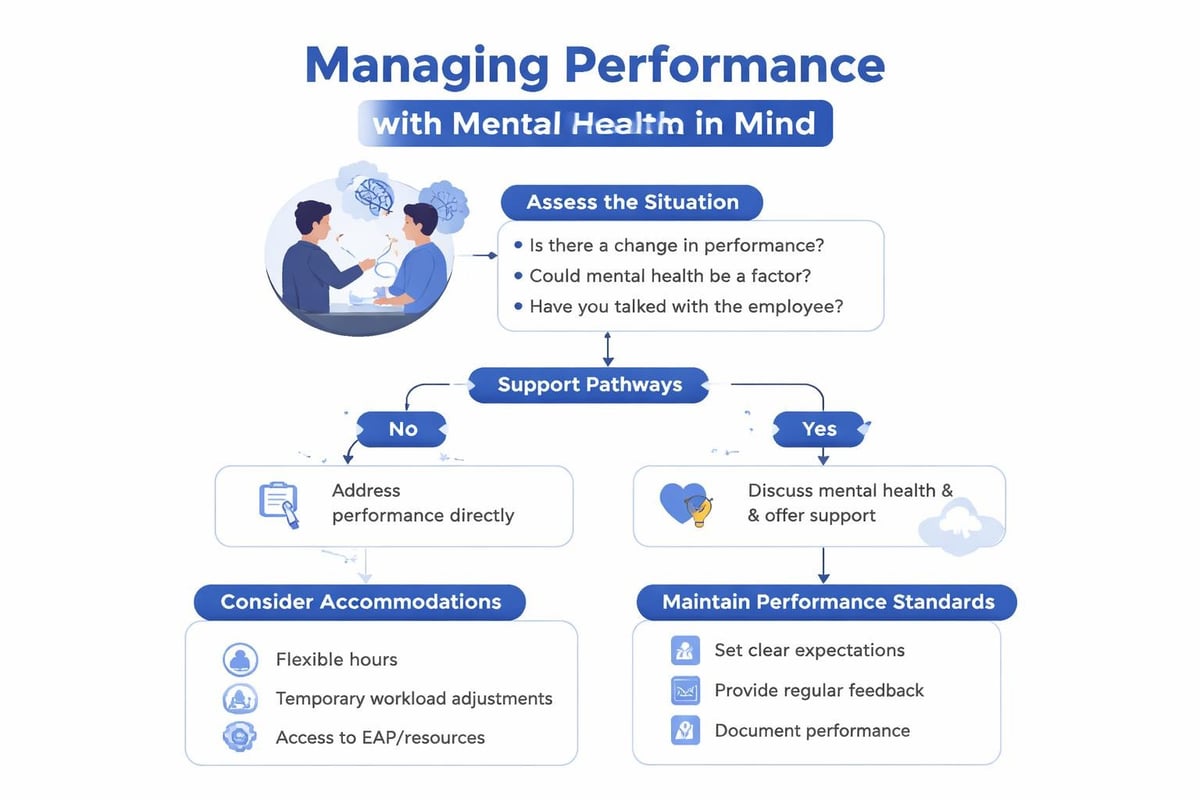
The critical question is not whether mental illness affects performance, but how organizations respond when it does:
Appropriate responses include:
- Documenting specific performance gaps without attributing causation
- Asking open-ended questions about support needs
- Offering Employee Assistance Program resources
- Exploring temporary accommodations during acute episodes
- Maintaining clear performance expectations alongside health support
Inappropriate responses include:
- Speculating about mental health status based on performance
- Demanding medical disclosure as condition of employment continuance
- Treating accommodation requests as performance improvement plan triggers
- Lowering standards indefinitely without structured review
High-performing organizations create parallel tracks where performance management and health support operate simultaneously. An employee can receive performance feedback while also accessing mental health accommodations. The accommodation addresses functional limitations; the performance management addresses job requirements.
Building Preventive Cultures
Reactive responses to mental health crises represent only partial solutions. Strategic organizations invest in preventive approaches that reduce the incidence and severity of workplace-related mental health deterioration.
Primary Prevention Strategies
These interventions target entire workforces to reduce risk factors before mental health problems emerge:
- Job design that provides autonomy, variety, and appropriate demand levels
- Workload management systems that prevent chronic overwork and burnout
- Psychosocial risk assessments that identify and modify high-stress work conditions
- Manager selection processes that screen for interpersonal competencies alongside technical skills
Managing employee mental health in organizational settings requires attention to work environment factors that research consistently links to mental health outcomes. Control over work methods, social support from supervisors and colleagues, and reasonable job demands predict mental health status more reliably than individual resilience characteristics.
Secondary Prevention Approaches
These target early identification and intervention when mental health symptoms first emerge:
- Train managers in early warning sign recognition
- Implement regular wellbeing check-ins as standard practice
- Reduce barriers to Employee Assistance Program access
- Create peer support networks for normalized help-seeking
- Offer mental health literacy training for all employees
The Workplace Mental Health Institute specializes in these capability-building programs, with resources available through their YouTube channel demonstrating practical implementation approaches.
Legal and Ethical Frameworks
Mental illness and the workplace exist within complex legal landscapes that vary by jurisdiction but share common principles. Organizations must navigate disability discrimination laws, privacy regulations, and duty of care obligations.
Core Legal Obligations
Reasonable Accommodation Requirements:
Most jurisdictions require employers to provide reasonable accommodations for qualified individuals with disabilities, including mental health conditions, unless doing so creates undue hardship. “Reasonable” and “undue hardship” are determined case-by-case based on organizational size, resources, and operational requirements.
Confidentiality Protections:
Medical information, including mental health disclosures, must be maintained separately from personnel files with access limited to those with legitimate business need. Unauthorized disclosure can create liability even when well-intentioned.
Anti-Discrimination Provisions:
Employees cannot be terminated, demoted, or otherwise disadvantaged solely because of mental health conditions. Actions must be based on legitimate performance or conduct issues, with accommodation exploration preceding adverse employment actions.
Organizations should consult legal counsel for jurisdiction-specific requirements, but legal compliance represents the minimum threshold rather than best practice aspiration.
Return-to-Work and Ongoing Management
Employees who take medical leave for mental health conditions require structured return-to-work processes that support sustainable reintegration.
Effective Return-to-Work Elements
- Pre-return communication between manager and employee to discuss accommodations and expectations
- Graduated return schedules that allow progressive reintegration rather than immediate full-time resumption
- Modified duties during initial return period to rebuild confidence and capacity
- Regular check-ins with decreasing frequency as stability returns
- Clear success metrics that define both employee and organizational responsibilities
The most successful returns occur when organizations treat mental health leaves identically to physical health leaves, avoiding special scrutiny or lowered expectations that paradoxically increase stigma.
Training as Strategic Investment
Organizations serious about mental illness and the workplace invest in systematic capability development rather than relying on manager intuition or reactive crisis responses. Healthcare settings demonstrate that structured conversations about mental health become normalized through training and practice.
Training Priorities by Organizational Role
Senior Leaders:
- Business case for mental health investment
- Strategic integration with organizational objectives
- Culture setting through appropriate disclosure and modeling
- Resource allocation for systemic approaches
Human Resources:
- Accommodation process management
- Policy development and compliance
- Manager consultation and support
- Return-to-work coordination
Managers:
- Conversation skills for mental health discussions
- Performance management with accommodation
- Referral pathways and resource awareness
- Confidentiality and documentation requirements
All Employees:
- Mental health literacy and stigma reduction
- Self-care and help-seeking skills
- Peer support capabilities
- Resource awareness
Comprehensive training catalogs addressing these levels are available through specialized providers focused exclusively on workplace applications rather than clinical treatment.
Measuring Impact and Continuous Improvement
Strategic mental health approaches require measurement frameworks that demonstrate value and guide refinement. Organizations should track leading indicators that predict future problems alongside lagging indicators that measure past outcomes.
Comprehensive Measurement Dashboard
| Metric Category | Example Measures | Strategic Value |
|---|---|---|
| Utilization | EAP engagement rates, accommodation requests | Early problem identification |
| Culture | Psychological safety survey scores, disclosure comfort levels | Environmental health assessment |
| Outcomes | Absenteeism rates, disability claim frequency, turnover in high-risk groups | Program effectiveness validation |
| Capability | Manager training completion, confidence in handling mental health scenarios | Organizational readiness evaluation |
| Performance | Productivity metrics, quality indicators, customer satisfaction | Business case validation |
Data should inform action rather than merely documenting problems. Regular review cycles that translate metrics into specific improvement initiatives demonstrate commitment beyond measurement for compliance purposes.
Organizations can access assessment tools and benchmarking data through specialized consultancies that understand workplace-specific applications rather than clinical measurement frameworks.
Integration with Broader Wellbeing Strategies
Mental illness and the workplace cannot be separated from physical health, financial wellbeing, and organizational culture initiatives. The most sophisticated organizations create integrated wellbeing strategies where mental health represents one element within comprehensive employee support systems.
This integration prevents siloed programs that duplicate efforts or create contradictory messages. When mental health initiatives align with leadership development, diversity and inclusion programs, and operational excellence efforts, they achieve deeper penetration and sustainability than standalone mental health campaigns.
Strategic wellbeing frameworks recognize that workplace factors influence mental health as powerfully as individual characteristics. Addressing work design, management practices, and organizational culture creates conditions where fewer employees develop workplace-induced mental health problems while supporting those managing pre-existing conditions.
Addressing mental illness and the workplace effectively requires organizations to move beyond awareness campaigns toward systematic capability building, policy development, and culture change that makes mental health support an operational reality rather than aspirational statement. The Workplace Mental Health Institute provides evidence-based training programs, assessment tools, and strategic consultation that help organizations build these capabilities systematically, with measurable outcomes that demonstrate both human and business value.


