The landscape of professional mental health practice continues to evolve rapidly, creating an urgent need for specialized, evidence-based trainings for mental health professionals. Practitioners today face increasingly complex workplace scenarios, from managing collective trauma to addressing systemic barriers to psychological safety. Effective training programs equip clinicians, counselors, and organizational mental health specialists with the practical skills, theoretical frameworks, and ethical foundations necessary to deliver meaningful outcomes across diverse settings.
Core Competencies in Contemporary Mental Health Training
Professional development for mental health practitioners extends far beyond initial credentialing. The field demands continuous skill acquisition across multiple domains, including assessment methodologies, intervention strategies, cultural competency, and emerging therapeutic modalities.
Foundational training areas include:
- Clinical assessment and differential diagnosis techniques
- Evidence-based therapeutic interventions
- Ethical decision-making frameworks
- Cultural humility and diversity-responsive care
- Trauma-informed practice principles
- Crisis intervention and risk management
The American Psychiatric Association provides educational resources that establish baseline standards for psychiatric training, though workplace-focused mental health professionals often require additional specialized preparation beyond traditional clinical models.
Workplace-Specific Mental Health Training Demands
Organizations increasingly recognize that clinical training alone does not prepare mental health professionals for the unique challenges of workplace environments. Corporate settings, employee assistance programs, and organizational wellness initiatives require practitioners who understand business operations, leadership dynamics, and systemic change methodologies.
Trainings for mental health professionals working in organizational contexts must address implementation realities, stakeholder engagement, and measurable business outcomes alongside therapeutic effectiveness.

Specialized Certification Programs and Advanced Training
Professional advancement often requires targeted certifications that demonstrate expertise in specific practice areas. These credentials validate competency, enhance professional credibility, and frequently satisfy continuing education requirements mandated by licensing boards.
| Certification Type | Primary Focus | Typical Duration | Target Audience |
|---|---|---|---|
| Trauma-Informed Care | Understanding trauma impact across populations | 20-40 hours | All mental health practitioners |
| Workplace Mental Health | Organizational interventions and consultation | 30-60 hours | EAP counselors, organizational psychologists |
| Mental Health First Aid | Initial response and referral skills | 8 hours | Managers, HR professionals, peer supporters |
| Resilience Training | Building adaptive capacity | 15-25 hours | Coaches, trainers, wellness professionals |
Organizations like The National Council for Mental Wellbeing offers transformative trainings that address middle management, whole health approaches, and integrated care models particularly relevant to workplace applications.
Evidence-Based Therapeutic Modalities
Trainings for mental health professionals must emphasize interventions with demonstrated research support. Cognitive Behavioral Therapy (CBT), Acceptance and Commitment Therapy (ACT), and Eye Movement Desensitization and Reprocessing (EMDR) represent gold-standard approaches with robust empirical backing.
However, workplace applications often require adaptation of these modalities to brief intervention formats, group settings, and preventive rather than treatment-focused frameworks. Professional training programs should specifically address translating clinical evidence into organizational contexts where extended therapeutic relationships may not be feasible.
Advanced modality training considerations:
- Assess alignment between therapeutic approach and workplace applications
- Evaluate evidence quality specific to employed populations
- Consider scalability and group delivery formats
- Review supervision requirements and ongoing consultation needs
- Confirm compatibility with organizational culture and values
Trauma-Informed Care Training Essentials
Understanding trauma's pervasive impact on workplace functioning has become non-negotiable for mental health professionals. Trauma-informed frameworks acknowledge that experiences of adversity, violence, chronic stress, and systemic oppression shape employee wellbeing, performance, and interpersonal dynamics.
Comprehensive trauma-informed care training addresses neurobiological impacts, recognizes re-traumatization risks, and emphasizes physical and psychological safety creation. The Substance Abuse and Mental Health Services Administration provides resources outlining trauma-informed principles applicable across service delivery systems.
Implementing Trauma-Informed Organizational Practices
Mental health professionals require practical skills for translating trauma-informed principles into workplace policies, communication practices, and leadership approaches. This includes training organizational stakeholders who may lack clinical backgrounds.
Effective programs teach practitioners to:
- Conduct organizational trauma-informed assessments
- Design psychologically safe communication protocols
- Identify and modify potentially re-traumatizing policies
- Coach leaders in trauma-responsive supervision
- Create peer support structures that honor trauma experiences
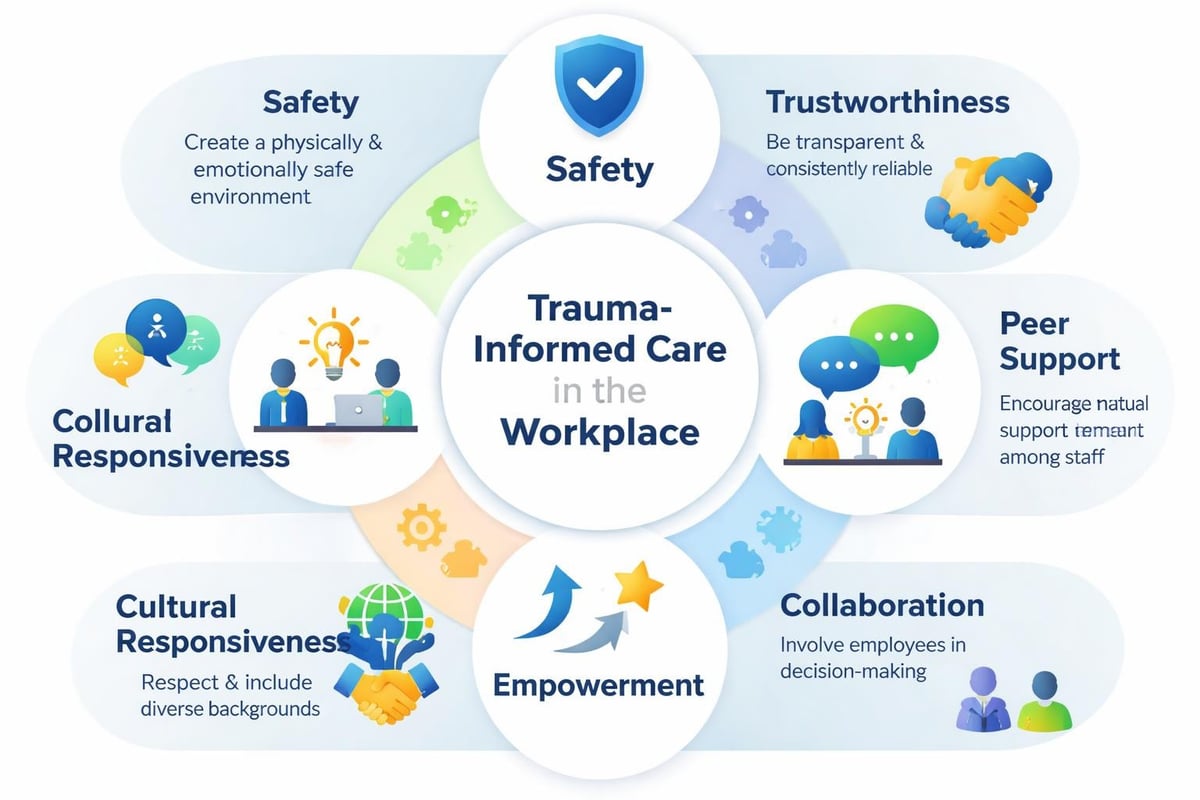
The building resilience at work programs offered through specialized institutes demonstrate how trauma-informed frameworks integrate with organizational resilience initiatives to create comprehensive support systems.
Continuing Education Requirements and Best Practices
Professional licensing boards mandate ongoing education to maintain credentials, with requirements varying substantially across jurisdictions and credential types. Most mental health professionals need between 20 and 40 continuing education hours biennially, though specific requirements depend on licensure category.
Common continuing education mandates include:
- Ethics and professional boundaries (typically 3-6 hours)
- Cultural competency and diversity training (2-4 hours)
- Suicide prevention and crisis intervention (2-6 hours)
- Supervision training for senior practitioners (10-20 hours)
- Specialty area updates relevant to practice focus
Therapy Trainings® offers affordable, board-approved online continuing education courses covering essential topics like trauma-informed care, ethics, and specialized assessment protocols, providing accessible options for busy professionals.
Selecting High-Quality Training Programs
Not all trainings for mental health professionals deliver equivalent value. Practitioners should evaluate programs based on instructor credentials, evidence foundations, practical application opportunities, and post-training support availability.
| Evaluation Criterion | Quality Indicators | Red Flags |
|---|---|---|
| Instructor Expertise | Advanced credentials, active practice, published research | Generic biographies, unclear qualifications |
| Evidence Base | Cited research, transparent methodology | Vague claims, proprietary "systems" without validation |
| Practical Application | Case examples, skill practice, implementation tools | Purely theoretical, no actionable strategies |
| Post-Training Support | Consultation access, resource libraries, community | No follow-up, limited materials |
Specialized Training for Workplace Mental Health Contexts
Mental health professionals supporting organizational wellbeing require distinct competencies beyond traditional clinical practice. These include understanding organizational behavior, change management principles, data-driven program evaluation, and stakeholder engagement strategies.
Workplace-focused training programs address consultation skills, needs assessment methodologies, and strategic planning for mental health initiatives. Practitioners learn to navigate complex organizational politics, secure leadership buy-in, and demonstrate return on investment for mental health programming.
Manager and Leadership Training Components
Many mental health professionals now train managers and organizational leaders rather than providing direct clinical services. This requires developing training design skills, facilitation competencies, and the ability to translate complex psychological concepts into accessible, actionable guidance.
Effective manager training programs created by mental health professionals typically cover:
- Recognizing mental health concerns in team members
- Conducting supportive conversations without overstepping boundaries
- Appropriate referral pathways and resource connection
- Creating psychologically safe team environments
- Managing their own wellbeing and preventing burnout
The American Mental Wellness Association provides education and training programs, including Mental Health First Aid, which many organizations now require for managers and HR professionals.
Specialized institutes offer keynotes and presentations on mental health and wellbeing that help mental health professionals develop their own facilitation and presentation capabilities for organizational audiences.
Digital Delivery and Online Training Platforms
The shift toward digital learning accelerated dramatically, creating both opportunities and quality concerns for trainings for mental health professionals. Online platforms enable geographic flexibility, cost reduction, and asynchronous learning, yet risk diminished engagement and reduced skill practice opportunities.
High-quality online training programs incorporate interactive elements, breakout discussions, case-based learning, and competency assessments rather than relying solely on recorded lectures. Hybrid models combining self-paced content with live skill practice sessions often deliver optimal outcomes.
Evaluating Online Training Credibility
Mental health professionals should verify that online training providers maintain appropriate accreditation, offer board-approved continuing education credits, and employ qualified instructors with relevant expertise. MentalHealth.gov offers comprehensive information helping professionals identify legitimate training resources.
Digital training quality markers:
- Clear accreditation documentation
- Interactive learning components
- Accessible instructor contact
- Peer interaction opportunities
- Technical support availability
- Mobile-responsive platforms
Professional training platforms like those available through https://thewmhionline.com demonstrate how specialized organizations deliver comprehensive online mental health training with workplace applications, practical tools, and ongoing resource access.
Measuring Training Effectiveness and Implementation
Completing trainings for mental health professionals represents only the initial step. True professional development requires translating acquired knowledge into sustained practice changes, measurable skill improvements, and enhanced client outcomes.
Effective training programs include implementation planning, post-training coaching, and outcome measurement frameworks. Practitioners should expect opportunities to practice new skills, receive feedback, and access ongoing consultation as they integrate training content into their work.
Creating Personal Professional Development Plans
Strategic professional development requires intentional planning aligned with career goals, practice setting demands, and identified skill gaps. Mental health professionals benefit from annual professional development planning that identifies priority training areas, allocates resources, and establishes accountability mechanisms.
Professional development planning steps:
- Assess current competencies against practice requirements
- Identify emerging trends and future skill demands
- Prioritize training areas based on impact and urgency
- Budget time and financial resources appropriately
- Schedule training completion and implementation milestones
- Arrange supervision or consultation for skill integration
- Evaluate outcomes and adjust plans accordingly
The Region IV Public Health Training Center offers mental health resources, including trainings, toolkits, and webinars supporting systematic professional development for public health professionals addressing mental health concerns in community and workplace settings.
Peer-Informed and Lived Experience Training Models
Contemporary best practices increasingly emphasize incorporating lived experience perspectives into trainings for mental health professionals. Programs designed and delivered by individuals with personal mental health experiences offer unique insights, reduce stigma, and enhance cultural humility among practitioners.
PMHCA and Youth MOVE PA provide engaging, peer-informed trainings for mental health professionals, peer workers, families, and community partners, demonstrating how lived experience expertise enriches professional development.
Cultural Responsiveness and Anti-Oppressive Practice
Training programs must address how systemic oppression, discrimination, and marginalization impact mental health while examining practitioners' own biases and privilege. Cultural responsiveness extends beyond surface-level diversity awareness to encompass structural competency and anti-oppressive practice commitments.
Effective cultural responsiveness training challenges mental health professionals to:
- Examine personal assumptions and implicit biases
- Understand historical trauma and systemic oppression
- Recognize power dynamics in therapeutic relationships
- Adapt interventions for cultural relevance
- Advocate for systemic change beyond individual treatment
Organizations serving diverse populations, including Australian organizations, increasingly require demonstrated cultural competency training for mental health professionals working in multicultural workplace environments.
Supervision and Advanced Practice Training
Experienced mental health professionals often transition into supervisory, training, or consultation roles requiring distinct competencies. Clinical supervision training addresses developmental supervision models, ethical supervision practices, and skills for cultivating supervisee growth.
Advanced practice training prepares professionals for specialized roles including program development, organizational consultation, research translation, and policy advocacy. These trainings emphasize leadership skills, strategic thinking, and systems-level intervention approaches beyond individual clinical work.
| Training Level | Focus Areas | Career Applications |
|---|---|---|
| Foundational | Clinical skills, ethics, assessment | Direct service provision |
| Intermediate | Specialized modalities, populations | Advanced clinical roles, team leadership |
| Advanced | Supervision, consultation, program design | Organizational roles, training delivery |
| Expert | Research, policy, systems change | Thought leadership, strategic influence |
For video resources demonstrating advanced workplace mental health training approaches, professionals can explore content available at https://www.youtube.com/@WorkplaceMentalHealthInstitute.
Selecting appropriate trainings for mental health professionals requires careful evaluation of program quality, relevance to practice context, and alignment with professional development goals. Prioritizing evidence-based content, practical skill development, and ongoing implementation support maximizes training investments. Workplace Mental Health Institute delivers comprehensive mental health training programs specifically designed for organizational contexts, equipping professionals with the specialized competencies needed to create psychologically healthy workplaces, support managers in their wellbeing responsibilities, and drive measurable improvements in employee mental health outcomes.


