The rapid expansion of remote mental health services has transformed how organizations support employee wellbeing, creating an urgent need for specialized competencies among mental health professionals. Telemental health training has evolved from a supplementary skill to a fundamental requirement for practitioners delivering workplace mental health programs, assessments, and interventions through digital platforms. This professional development addresses technical proficiency, therapeutic adaptation, ethical considerations, and the unique challenges of supporting employees in virtual environments where traditional in-person cues and rapport-building strategies require recalibration.
Understanding Telemental Health Training Requirements
Telemental health training encompasses a comprehensive skill set that extends far beyond basic video conferencing capabilities. Mental health professionals supporting workplace populations must master platform-specific technologies, understand regulatory frameworks governing virtual care, and develop specialized techniques for building therapeutic alliances without physical presence.
The core competency framework includes technical proficiency with HIPAA-compliant platforms, clinical adaptation of assessment and intervention strategies, crisis management protocols for remote settings, and documentation practices that meet both legal and ethical standards. Organizations implementing workplace mental health programs increasingly recognize that effective virtual support requires practitioners who have received systematic training in telemental health delivery methods.
Essential Competencies for Workplace Applications
Mental health professionals working with organizational clients face distinct challenges compared to traditional clinical settings. Employees accessing telemental health services may be connecting from home offices, shared workspaces, or mobile devices during breaks, creating unique privacy considerations and environmental variables.
Training programs must address:
- Boundary management in workplace contexts where professional and personal spaces overlap
- Confidentiality protocols when employees share environments with colleagues or family members
- Cultural competency for geographically dispersed or international workforce populations
- Technology troubleshooting to minimize disruption and maintain therapeutic continuity
- Asynchronous communication strategies for supporting employees across time zones

Organizations like Workplace Mental Health Institute recognize that comprehensive training must prepare practitioners for the specific dynamics of supporting employees remotely, including the intersection of workplace stressors, personal challenges, and the therapeutic relationship mediated through screens.
Clinical Adaptation Strategies for Virtual Environments
The therapeutic skills that prove effective in face-to-face settings require intentional modification for telemental health contexts. Practitioners cannot rely on the same nonverbal cues, physical proximity, or environmental control that characterize traditional office-based sessions.
Effective telemental health training teaches professionals to compensate for reduced sensory information by sharpening attention to vocal tone variations, micro-expressions visible on camera, and linguistic patterns that indicate emotional states. The implementation of structured telemental health programs demonstrates measurable improvements when practitioners receive specialized instruction in these adaptive techniques.
Assessment and Diagnostic Considerations
Mental health assessments conducted through telemental health platforms introduce both opportunities and constraints. Video conferencing enables observation of home environments, potentially revealing information about living conditions, support systems, and stressors that might not emerge in office settings. However, videoconferencing and telephone-based mental health care requires practitioners to adjust standard assessment protocols.
| Assessment Component | In-Person Approach | Telemental Health Adaptation |
|---|---|---|
| Suicide risk evaluation | Physical environment scan, removal of means | Verbal assessment, safety planning with remote supports |
| Substance use screening | Behavioral observation, physiological indicators | Self-report emphasis, contextual questioning |
| Anxiety presentation | Full body language, physical manifestations | Focused facial expression analysis, verbal descriptors |
| Workplace stress assessment | Generic environmental discussion | Direct observation of work-from-home setting when appropriate |
Training must equip professionals to recognize when virtual assessment proves insufficient and establish clear protocols for transitioning to in-person evaluation or higher levels of care.
Technology Proficiency and Platform Selection
Competent telemental health delivery requires more than knowing how to initiate a video call. Practitioners need comprehensive understanding of platform capabilities, security features, troubleshooting procedures, and backup communication methods when technical failures occur.
Professional training should include hands-on experience with:
- Platform security audits to verify HIPAA or equivalent compliance standards
- Screen sharing capabilities for collaborative document review or skill-building exercises
- Recording features and their legal/ethical implications in different jurisdictions
- Breakout room functions for group supervision or multi-party consultations
- Mobile application interfaces to support employees accessing services via smartphones
- Accessibility features ensuring services reach employees with disabilities
The technical infrastructure supporting workplace mental health programs must accommodate diverse employee technology capabilities while maintaining consistent security standards. Organizations implementing telemental health services benefit from comprehensive training programs that address both practitioner competencies and organizational system requirements.
Privacy and Confidentiality in Digital Spaces
Protecting employee confidentiality in telemental health contexts demands heightened awareness and proactive strategies. Unlike controlled office environments with soundproofing and waiting room protocols, virtual sessions occur in spaces where privacy cannot be guaranteed.
Practitioners must be trained to:
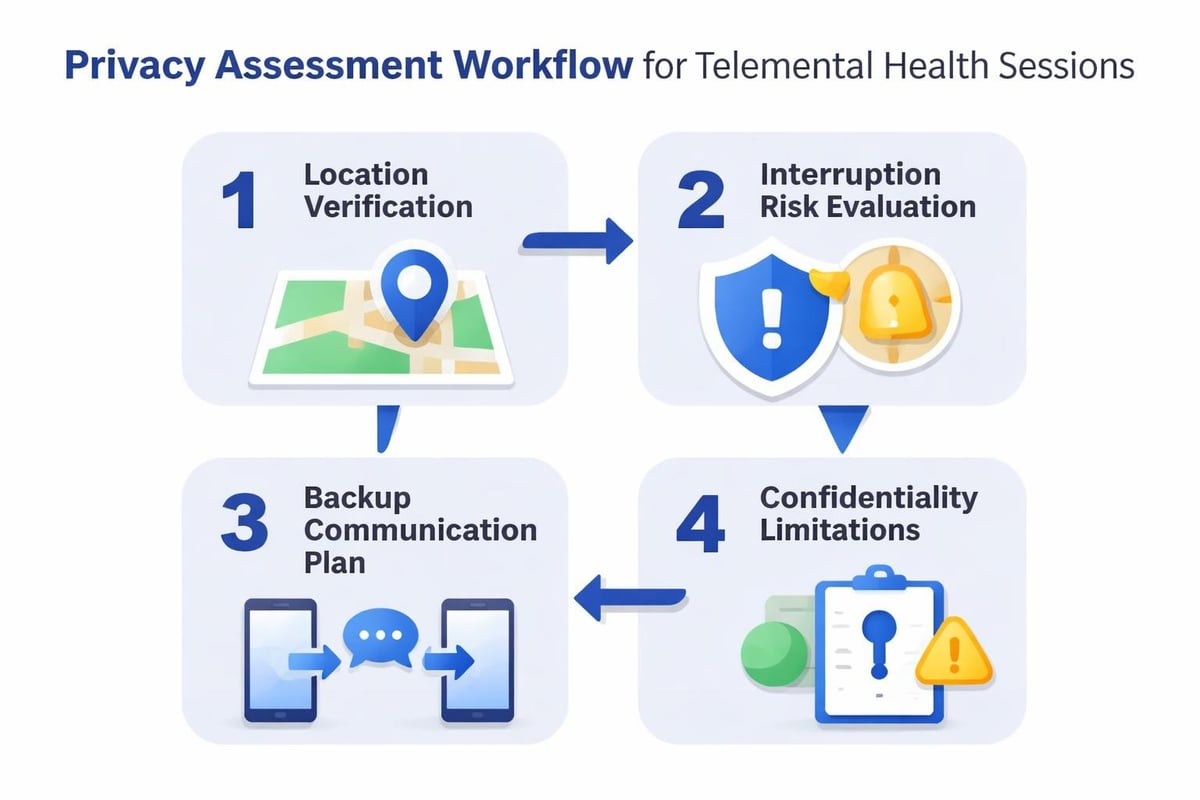
- Conduct privacy assessments at session initiation, verifying employee's current location and potential for interruption
- Develop code word systems allowing employees to quickly signal compromised privacy
- Create alternative communication plans when video sessions prove inappropriate due to privacy constraints
- Document privacy limitations and their potential impact on treatment planning
Organizations investing in workplace mental health capacity should ensure their practitioners understand the intersection of privacy law, workplace policies, and ethical obligations that govern telemental health delivery.
Crisis Intervention and Risk Management Protocols
Risk assessment and crisis intervention through telemental health platforms represent among the most challenging aspects of virtual care delivery. Training programs must prepare practitioners for scenarios where an employee presents with acute suicidal ideation, experiences a medical emergency during a session, or discloses information suggesting imminent harm.
The absence of physical proximity fundamentally alters crisis response options. Practitioners cannot physically secure an environment, accompany an employee to emergency services, or directly intervene in unfolding situations.
Comprehensive telemental health training addresses:
- Pre-session emergency contact collection to enable rapid coordination with local resources
- Geolocation protocols ensuring practitioners can direct emergency services to employee locations
- Collaboration templates for engaging emergency contacts without breaching confidentiality inappropriately
- De-escalation techniques optimized for virtual environments where physical grounding exercises may prove less effective
- Documentation standards for crisis episodes occurring through telemental health platforms
Research examining telemental health interventions for specific populations highlights the importance of establishing clear risk management protocols before initiating virtual services, particularly when serving employees experiencing chronic stress or mental health conditions.
Building Therapeutic Alliance Through Screens
The therapeutic relationship serves as a foundational element of effective mental health support, regardless of delivery modality. Telemental health training must explicitly address alliance-building strategies adapted for virtual contexts where traditional rapport-building approaches require modification.
Practitioners report that creating connection through screens demands increased intentionality around verbal affirmations, consistent eye contact with cameras rather than screens, and explicit acknowledgment of the unique dynamics introduced by technology-mediated communication. Training experiences during rapid telemental health adoption revealed that practitioners initially struggled with these adaptations before developing compensatory strategies through focused skill development.
Engagement Strategies for Workplace Populations
Employees accessing mental health support through workplace programs may experience additional barriers to engagement compared to individuals seeking services independently. Concerns about employer knowledge, workplace stigma, and career implications can complicate the therapeutic relationship even when strong confidentiality protections exist.
Effective telemental health training for workplace contexts includes:
- Transparency about information sharing protocols between practitioners and organizational clients
- Strategies for separating workplace mental health support from performance management
- Cultural awareness regarding different employee populations' comfort with virtual disclosure
- Techniques for establishing trust when employees perceive limited privacy in home environments
Organizations can support these efforts by selecting training programs that specifically address the unique considerations of workplace telemental health delivery, ensuring practitioners develop competencies aligned with organizational mental health program objectives.
Ethical Frameworks and Professional Standards
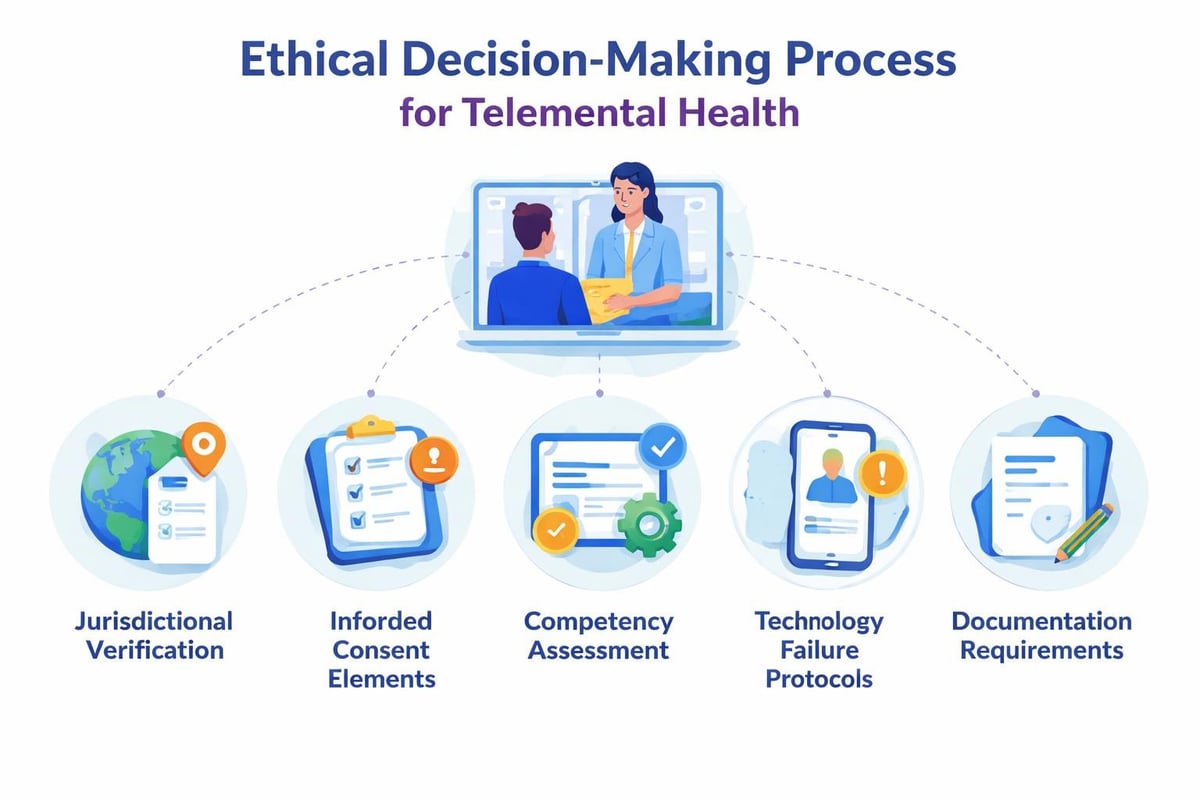
Telemental health practice operates within evolving ethical guidelines that address jurisdictional licensing, informed consent, technology failures, and boundary management in digital spaces. Training programs must equip practitioners with frameworks for navigating these complex considerations while maintaining the highest professional standards.
Key ethical domains include:
| Ethical Domain | Primary Considerations | Training Requirements |
|---|---|---|
| Jurisdictional practice | Licensure requirements across state/national boundaries | Understanding of jurisdiction-specific regulations governing telehealth |
| Informed consent | Technology risks, privacy limitations, emergency protocols | Development of comprehensive telemental health consent procedures |
| Competency boundaries | Platform-specific skills, population-specific adaptations | Ongoing assessment of practitioner competence with virtual modalities |
| Professional development | Emerging technologies, evolving best practices | Commitment to continuing education in telemental health advances |
The American Psychiatric Nurses Association’s telemental health toolkit provides valuable resources for practitioners developing ethical frameworks appropriate to virtual care contexts, addressing policy considerations, equity concerns, and educational foundations.
Documentation and Record-Keeping Standards
Electronic health records and session documentation require particular attention in telemental health contexts. Practitioners must document not only clinical content but also technology-related information, privacy assessments, and any factors unique to virtual service delivery.
Training should address documentation of technical failures, session interruptions, privacy compromises, and decisions to modify treatment approaches based on platform limitations. These records serve both clinical continuity and risk management functions, creating an evidence base for clinical decision-making while protecting practitioners and organizations from potential liability.
Specialized Applications for Organizational Mental Health
Workplace mental health programs extend beyond individual therapy to include manager training, resilience workshops, trauma-informed care initiatives, and organizational consultations. Telemental health training must prepare practitioners to adapt these diverse services for virtual delivery while maintaining program effectiveness.
Group facilitation through video platforms introduces logistical complexities around participant engagement, confidentiality in multi-party settings, and management of group dynamics when participants cannot easily read room energy or sidebar conversations. Training programs addressing these challenges prepare practitioners to leverage platform features like breakout rooms, polling functions, and chat capabilities to enhance group experiences.
Training Delivery and Skill Development
Organizations implementing comprehensive mental health training programs for managers and employees increasingly deliver content through virtual platforms, requiring facilitators to maintain engagement across potential distractions and varying technology capabilities among participants.
Effective telemental health training for organizational contexts includes:
- Interactive facilitation techniques that prevent passive viewing and encourage active participation
- Assessment strategies to evaluate skill acquisition when traditional in-person role-playing proves impractical
- Technology equity considerations ensuring all employees can access training regardless of device or connectivity limitations
- Asynchronous learning integration to accommodate shift workers, international teams, and varied schedules
- Breakout room utilization for small group discussions and peer learning opportunities
The shift toward virtual training delivery creates opportunities for broader organizational reach while demanding facilitator competencies specific to digital learning environments.
Implementation Science and Program Development
Establishing successful telemental health programs within organizations requires systematic planning, stakeholder engagement, and attention to implementation science principles. Training for mental health professionals should include not only clinical competencies but also understanding of how to launch, sustain, and continuously improve virtual services.
Implementation science methodology applied to telemental health demonstrates the value of structured approaches that address organizational readiness, champion identification, workflow integration, and outcome measurement. Mental health professionals supporting workplace populations benefit from training that positions them as strategic partners in program development rather than solely service providers.
Quality Assurance and Outcome Measurement
Telemental health programs require ongoing evaluation to ensure they meet employee needs, achieve organizational objectives, and maintain clinical effectiveness. Training should prepare practitioners to participate in quality assurance processes through outcome tracking, satisfaction monitoring, and continuous program refinement.
Key measurement areas include employee engagement rates, clinical outcomes for common workplace mental health concerns, technology-related barriers, and cost-effectiveness compared to traditional service delivery models. Practitioners trained in these evaluation methods contribute valuable insights that strengthen organizational mental health initiatives.
Trauma-Informed Approaches in Virtual Settings
Delivering trauma-informed care through telemental health platforms presents both opportunities and challenges. The ability for employees to access support from familiar, safe environments can reduce activation compared to traveling to unfamiliar clinical settings. However, practitioners must remain vigilant to trauma responses triggered by technology, screen-mediated interaction, or home environments that may hold traumatic associations.
Specialized telemental health training for trauma work includes understanding how virtual platforms can support grounding techniques, safety planning, and gradual exposure while recognizing when platform limitations compromise trauma treatment effectiveness. Organizations supporting employees who have experienced workplace trauma, critical incidents, or personal traumatic events benefit from practitioners with specific training in trauma-informed telemental health delivery.
Trauma-informed telemental health competencies include:
- Recognition of technology-related triggers and appropriate accommodation strategies
- Adaptation of somatic interventions for virtual delivery
- Environmental safety assessment considering home-based session locations
- Collaboration with on-site supports when employees require immediate grounding assistance
- Cultural considerations around privacy, disclosure, and help-seeking in trauma contexts
Regional and Cultural Considerations
Telemental health training must address the cultural contexts within which practitioners operate, recognizing that effective virtual care requires awareness of regional attitudes toward mental health, technology access disparities, and cultural communication norms. Programs serving geographically distributed workforces or culturally diverse regions require practitioners trained to navigate these complexities.
For organizations operating in Australia, specialized platforms and training through WMHI Australia address region-specific regulatory requirements, cultural considerations for Aboriginal and Torres Strait Islander employees, and integration with Australian workplace mental health frameworks.
Cultural competency in telemental health extends beyond demographic awareness to include understanding of digital literacy variations, technology access inequities, and cultural norms around screen-based communication that influence therapeutic relationships and intervention effectiveness.
Continuing Education and Professional Development
The rapidly evolving nature of telemental health technology, emerging research on virtual intervention effectiveness, and changing regulatory landscapes demand ongoing professional development. Initial telemental health training provides foundational competencies, but practitioners must commit to continuous learning to maintain currency with best practices.
Professional development pathways include participation in specialized workshops, engagement with peer consultation groups focused on telemental health challenges, review of emerging research literature, and experimentation with new platform capabilities that enhance service delivery. Organizations benefit from creating cultures that support practitioner learning and allocate resources for continuing education.
The Workplace Mental Health Institute’s video resources provide accessible continuing education content addressing evolving workplace mental health topics, including telemental health applications, that practitioners can integrate into ongoing professional development.
Effective telemental health training equips workplace mental health professionals with the clinical, technical, and ethical competencies required to deliver high-quality virtual services that support employee wellbeing and organizational performance. Organizations seeking to strengthen their mental health capacity through evidence-based telemental health programs can partner with Workplace Mental Health Institute to access comprehensive training, strategic consultation, and practical tools that translate virtual care competencies into measurable workplace outcomes.


