The modern workplace faces unprecedented challenges in supporting employee mental health. Organizations that prioritize creating mentally healthy workplaces don't just improve individual wellbeing-they build resilient, high-performing cultures that attract talent, reduce costs, and drive sustainable business outcomes. Understanding the practical elements that constitute psychologically safe environments requires moving beyond superficial wellness initiatives toward systematic, evidence-informed approaches that embed mental health support into organizational DNA.
What Defines Mentally Healthy Workplaces
Mentally healthy workplaces are organizational environments where psychological safety, proactive support systems, and clear mental health policies combine to protect and promote employee wellbeing. These workplaces recognize that mental health exists on a continuum and requires both preventative measures and responsive interventions.
The foundation rests on leadership commitment that translates into tangible resources, training, and accountability. When executives visibly prioritize mental health and allocate budget accordingly, they signal that wellbeing is a core business priority rather than a compliance exercise.
Core Components of Psychological Safety
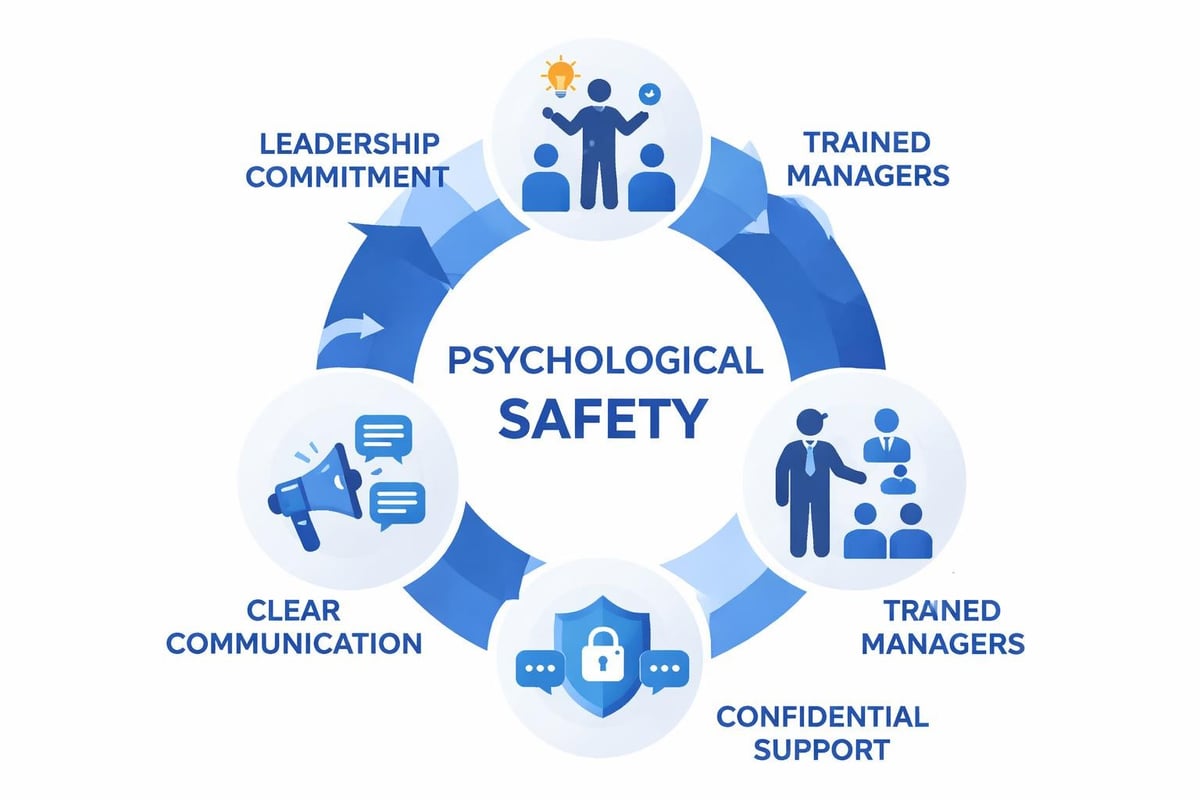
Psychologically safe environments allow employees to express concerns, admit mistakes, and seek help without fear of negative consequences. This requires:
- Clear communication channels that employees understand and trust
- Trained managers who can recognize distress signals and respond appropriately
- Non-punitive policies that encourage disclosure rather than concealment
- Confidential support pathways that protect privacy while enabling intervention
Research indicates that psychological safety directly correlates with innovation, engagement, and retention. Organizations must measure these factors systematically rather than relying on assumptions about workplace culture.
Building Preventative Infrastructure
Prevention requires systematic approaches that address organizational factors contributing to psychological harm. The government framework for measuring what matters provides structured guidance for assessing current state and implementing improvements.
| Prevention Layer | Key Actions | Expected Outcomes |
|---|---|---|
| Organizational Design | Reasonable workloads, role clarity, manageable deadlines | Reduced burnout, improved productivity |
| Social Environment | Respectful communication, conflict resolution, team cohesion | Enhanced collaboration, lower turnover |
| Physical Workspace | Ergonomic design, quiet spaces, natural light | Decreased stress, better focus |
| Growth Opportunities | Career development, skill building, meaningful work | Increased engagement, retention |
Workplace Mental Health Institute emphasizes that effective prevention stems from understanding workplace-specific risk factors through comprehensive wellbeing assessments. Generic programs rarely address the nuanced challenges facing particular industries or organizational contexts.
Implementing Early Intervention Systems
Early intervention prevents minor concerns from escalating into serious mental health conditions. This requires training managers to notice behavioral changes, performance shifts, or attendance patterns that may signal distress.
Effective systems include regular check-ins, structured return-to-work protocols, and accessible Employee Assistance Programs (EAPs) that employees actually use. Many EAPs fail because employees don't know they exist or perceive them as ineffective.
Training should equip managers with conversation frameworks that balance concern with professional boundaries. The goal is connecting employees with appropriate support, not amateur therapy.
Manager Capability and Mental Health Literacy
Managers serve as the primary interface between organizational mental health policy and employee experience. Their capability directly determines whether mentally healthy workplaces become reality or remain aspirational statements.
Mental health literacy for managers encompasses recognition, response, and referral skills. Managers must understand common presentations of mental health challenges, know how to initiate supportive conversations, and connect employees with professional resources.
Essential Manager Competencies
Training programs should develop these specific capabilities:
- Recognizing distress indicators including changes in work quality, communication patterns, or interpersonal interactions
- Conducting supportive conversations using non-judgmental language and active listening
- Understanding legal obligations regarding reasonable adjustments and discrimination
- Managing boundaries between support and clinical intervention
- Accessing organizational resources including HR, EAP, and occupational health services
The Workplace Mental Health Institute provides evidence-based manager training that emphasizes practical skill development over theoretical knowledge. Managers need actionable frameworks they can apply immediately when supporting distressed team members.
Small businesses face unique challenges in developing manager capability. The practical guide for small businesses offers accessible approaches that don't require extensive resources or specialized expertise.
Measurement and Continuous Improvement
Organizations cannot improve what they don't measure. Mentally healthy workplaces implement systematic measurement that tracks both leading indicators (preventative factors) and lagging indicators (outcomes like absenteeism or workers' compensation claims).
Leading indicators include:
- Manager mental health literacy scores
- Employee perceptions of psychological safety
- Utilization rates of mental health resources
- Policy awareness across the organization
Lagging indicators include:
- Absenteeism and presenteeism rates
- Turnover attributed to workplace stress
- Mental health-related workers' compensation claims
- Engagement scores and satisfaction metrics
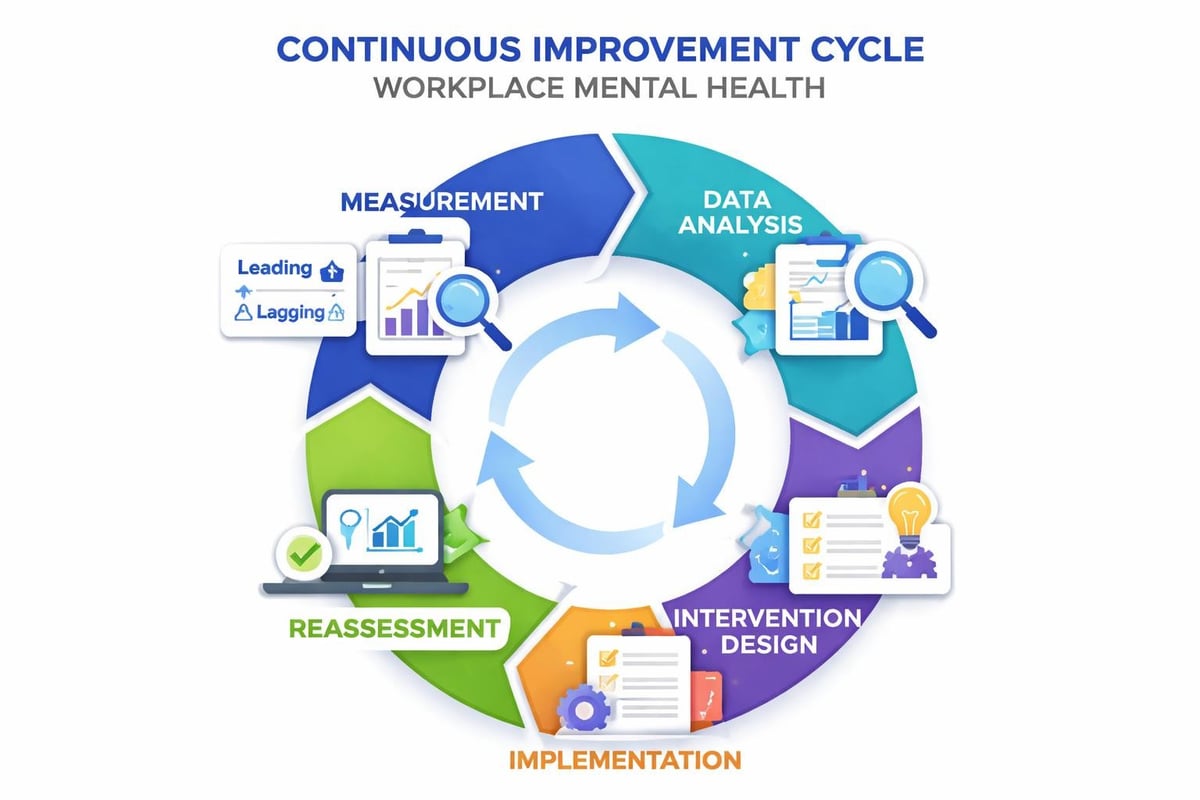
Creating Measurement Systems
Organizations should establish baseline metrics before implementing new initiatives. This enables accurate assessment of program effectiveness rather than assuming interventions work.
| Measurement Approach | Best For | Frequency |
|---|---|---|
| Anonymous surveys | Psychological safety, culture, stigma | Quarterly or bi-annually |
| Utilization data | EAP uptake, training completion | Monthly |
| Focus groups | Qualitative insights, program feedback | Annually |
| HR analytics | Absenteeism, turnover, claims | Monthly |
| Manager assessments | Individual capability, confidence | Pre/post training |
The Society for Human Resource Management offers a comprehensive checklist for mentally healthy workplaces that helps organizations audit current practices against best-practice standards.
Policy Framework and Legal Compliance
Robust mental health policies provide clear expectations, processes, and protections for both employees and employers. Effective policies address prevention, early intervention, accommodation, and return-to-work pathways.
Policies must align with legal obligations while exceeding minimum compliance standards. Organizations demonstrate commitment through policies that are accessible, regularly reviewed, and actually implemented rather than filed away.
Essential Policy Elements
Comprehensive mental health policies include:
- Clear definitions of mental health, psychological safety, and workplace responsibilities
- Confidentiality protections with transparent limitations (mandatory reporting situations)
- Reasonable adjustment processes for employees experiencing mental health challenges
- Return-to-work protocols that support gradual reintegration
- Accountability mechanisms ensuring policy implementation across all levels
Policies fail when they exist only on paper. Implementation requires training, resources, and leadership modeling. When executives discuss their own mental health or flexible working arrangements, they normalize conversations that policies merely permit.
The connection between psychologically healthy workplaces and population mental health underscores that organizational mental health initiatives contribute to broader societal wellbeing beyond individual workplaces.
Trauma-Informed Workplace Practices
Trauma-informed approaches recognize that many employees have experienced significant adversity that affects their workplace functioning. Organizations that implement trauma-informed practices create environments where survivors can thrive without requiring disclosure.
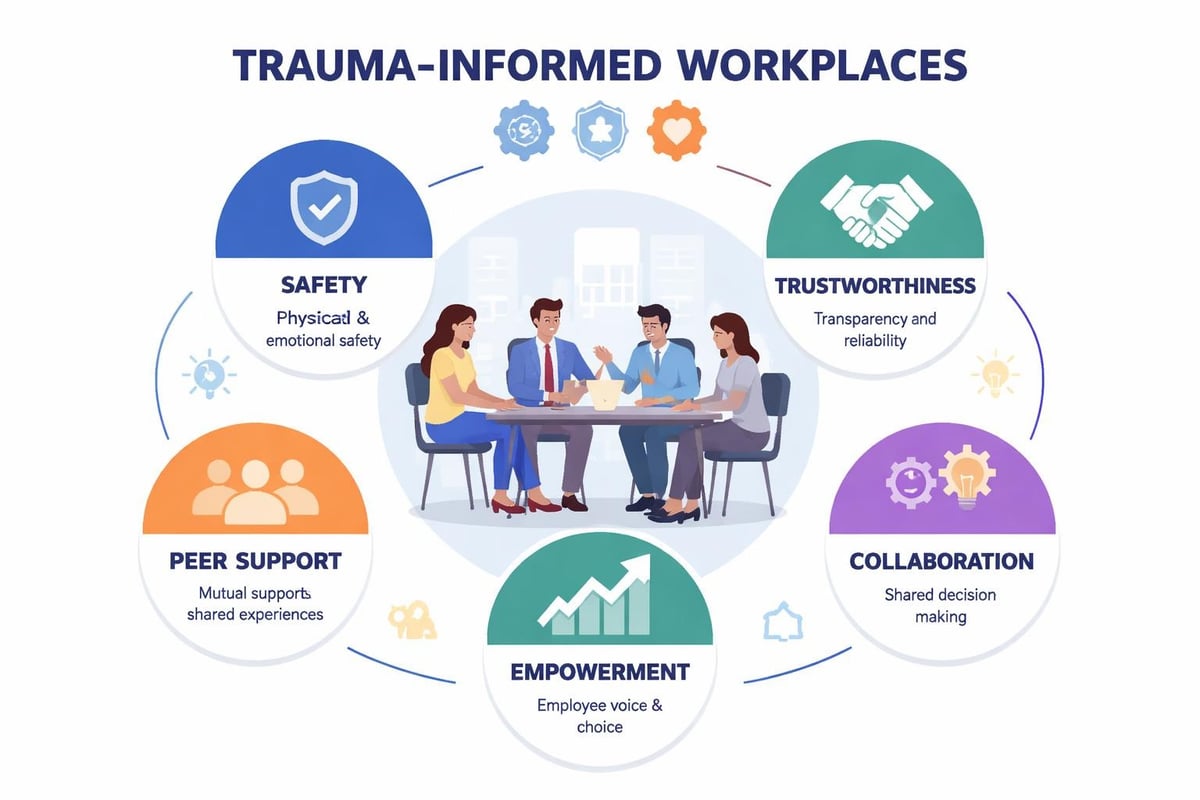
Principles of Trauma-Informed Workplaces
Safety: Physical and psychological safety form the foundation, with predictable environments and transparent communication.
Trustworthiness: Consistent policies, follow-through on commitments, and clear boundaries build organizational trust.
Peer support: Connecting employees with lived experience creates validation and reduces isolation.
Collaboration: Shared decision-making and employee input ensure programs meet actual needs.
Empowerment: Skill-building and choice recognize employee strengths rather than focusing solely on deficits.
Trauma-informed training helps managers understand how past experiences may influence current behavior without requiring employees to disclose personal histories. This awareness prevents retraumatization through insensitive management practices.
Australian organizations can access specialized resources through WMHI Australia that address region-specific workplace considerations and regulatory frameworks.
Strategic Implementation Roadmap
Transforming organizational culture requires phased implementation rather than attempting comprehensive change simultaneously. Strategic roadmaps sequence initiatives to build capability progressively.
Phase 1: Assessment and Planning (Months 1-3)
- Conduct baseline wellbeing assessment
- Review existing policies and identify gaps
- Secure leadership commitment and budget
- Establish measurement framework
Phase 2: Foundation Building (Months 4-9)
- Implement core manager training
- Update or create mental health policies
- Launch awareness campaigns
- Establish support pathways
Phase 3: Embedding and Optimization (Months 10-18)
- Advanced manager development
- Refine programs based on data
- Address identified risk factors
- Scale successful initiatives
Phase 4: Sustaining and Evolving (Ongoing)
- Regular measurement and reporting
- Continuous improvement cycles
- Emerging issue response
- Cultural reinforcement
Organizations often underestimate the time required for cultural change. Sustainable mentally healthy workplaces emerge through consistent effort over years, not quick fixes or one-time interventions.
Role of Learning and Development
Comprehensive training programs equip employees at all levels with mental health literacy, self-care strategies, and help-seeking skills. Effective learning goes beyond awareness to develop practical capabilities.
Training should differentiate between:
- General employee programs covering mental health literacy, stress management, and resource awareness
- Manager-specific training focused on recognition, response, and referral competencies
- Executive education emphasizing strategic mental health integration and organizational accountability
- Specialized roles including HR, health and safety, and wellbeing coordinators
Online training platforms provide scalable delivery while maintaining quality and consistency across geographically dispersed workplaces. Digital learning enables self-paced progression with certification tracking.
Interactive components including case studies, role plays, and scenario-based learning develop applied skills rather than passive knowledge. Employees must practice difficult conversations and decision-making in low-stakes environments before facing real situations.
Addressing Stigma and Cultural Change
Stigma remains the primary barrier preventing employees from seeking help or disclosing mental health challenges. Organizations must actively counter stigma through visible leadership commitment, education, and policy enforcement.
Cultural change requires:
- Leadership disclosure when appropriate, modeling help-seeking behavior
- Language shifts moving from "mental illness" to "mental health and wellbeing"
- Success stories highlighting recovery and accommodation
- Zero-tolerance policies for discrimination or harassment
- Consistent messaging across all organizational communications
Video resources from the Workplace Mental Health Institute YouTube channel provide accessible content that normalizes mental health conversations and demonstrates practical strategies.
Return-to-Work and Ongoing Support
Supporting employees returning from mental health-related absence requires structured processes that facilitate successful reintegration while protecting privacy and dignity.
| Return-to-Work Element | Purpose | Key Considerations |
|---|---|---|
| Pre-return planning | Coordinate adjustments and expectations | Involve employee, manager, HR, treating providers |
| Graduated schedule | Enable adjustment without overwhelming | Flexibility based on individual recovery |
| Role modifications | Temporarily adjust duties if needed | Clear timeframes and review points |
| Regular check-ins | Monitor progress and address concerns | Balance support with autonomy |
| Accommodation reviews | Assess ongoing needs | Document and evaluate effectiveness |
Employees fear that disclosure will limit career progression or mark them as unreliable. Organizations must demonstrate through actions that seeking support strengthens rather than jeopardizes employment relationships.
Integration with Broader Wellbeing Strategies
Mental health initiatives achieve maximum impact when integrated with comprehensive wellbeing strategies addressing physical health, financial security, social connection, and professional development.
Siloed programs create confusion and reduce utilization. Integrated approaches recognize that wellbeing factors interact, with financial stress affecting mental health, poor sleep impacting performance, and social isolation exacerbating psychological distress.
Effective integration coordinates:
- Physical health programs including exercise, nutrition, and preventative care
- Financial wellbeing through education, resources, and fair compensation
- Social connection via team-building, mentoring, and community involvement
- Work-life integration supporting flexibility and boundary management
- Purpose and meaning connecting individual roles to organizational mission
Organizations should audit all wellbeing initiatives to identify redundancies, gaps, and opportunities for synergy. Employees appreciate streamlined, coherent programs over fragmented offerings requiring separate navigation.
Evaluating Program Effectiveness
Rigorous evaluation determines whether investments in mentally healthy workplaces generate expected returns. Evaluation should assess process measures (implementation quality), outcome measures (wellbeing improvements), and impact measures (business results).
Process evaluation questions:
- Are programs implemented as designed?
- Do participation rates meet targets?
- Are resources accessible and utilized?
Outcome evaluation questions:
- Have employee wellbeing scores improved?
- Has psychological safety increased?
- Do employees feel supported?
Impact evaluation questions:
- Have absenteeism rates decreased?
- Has productivity improved?
- Are retention metrics favorable?
Organizations should use control groups or matched comparisons when feasible to attribute changes specifically to mental health programs rather than external factors. While randomized controlled trials rarely occur in workplace settings, quasi-experimental designs strengthen causal inferences.
Qualitative data from interviews and focus groups provides context that quantitative metrics miss. Employees can explain why programs work or fail, offering insights for continuous improvement.
Building mentally healthy workplaces requires strategic commitment, evidence-informed practices, and sustained implementation that extends beyond superficial wellness initiatives. Organizations that invest in comprehensive approaches reap benefits including enhanced performance, reduced costs, and strengthened employer brand while fulfilling ethical obligations to protect employee wellbeing. Workplace Mental Health Institute offers specialized training, assessment tools, and strategic consultation that help organizations translate mental health commitments into measurable outcomes through practical, resilience-focused programs designed for real-world workplace contexts.


