The quality of mental health discussions within an organization fundamentally shapes workplace culture, employee wellbeing, and operational performance. Leaders and HR professionals who develop the capacity to facilitate these conversations with skill and authenticity create environments where psychological safety becomes the foundation for innovation, collaboration, and resilience. Yet many organizations struggle to move beyond superficial acknowledgment of mental health toward substantive dialogue that generates meaningful change. Understanding how to initiate, sustain, and deepen mental health discussions requires both psychological literacy and organizational courage.
The Critical Role of Mental Health Literacy in Workplace Dialogue
Mental health literacy serves as the foundation for productive workplace conversations. Without a shared understanding of mental health concepts, symptoms, and support pathways, discussions often devolve into confusion, stigma, or well-intentioned but ineffective responses.
Foundational knowledge areas for workplace mental health discussions include:
- Recognition of common mental health conditions and their workplace manifestations
- Understanding of protective factors and risk indicators
- Awareness of support resources and referral pathways
- Competency in psychological first aid principles
- Knowledge of legal obligations and confidentiality boundaries
Organizations that invest in building this baseline literacy create conditions where mental health discussions can occur without constant fear of saying the wrong thing. The National Institute of Mental Health provides comprehensive information on mental disorders and treatments that can inform organizational education efforts.
Distinguishing Mental Health Awareness from Actionable Knowledge
Many organizations confuse awareness campaigns with genuine capability building. Distributing posters about mental health or hosting one-time speakers rarely translates into improved conversation quality or support outcomes.
Effective mental health training for managers and employees requires structured skill development. This includes practice scenarios, feedback mechanisms, and ongoing reinforcement rather than passive information consumption.

| Awareness Level | Conversation Capacity | Organizational Impact |
|---|---|---|
| Surface awareness | Acknowledges mental health exists | Minimal behavior change |
| Basic literacy | Can identify distress signals | Increased help-seeking |
| Applied competency | Conducts supportive conversations | Reduced presenteeism |
| Strategic integration | Embeds mental health in operations | Cultural transformation |
The shift from awareness to competency represents the difference between organizations that talk about mental health and those that effectively support it through meaningful dialogue.
Psychological Safety as the Prerequisite for Authentic Dialogue
Mental health discussions cannot flourish in psychologically unsafe environments. When employees perceive that disclosure carries professional risk, conversations remain superficial or nonexistent regardless of organizational policy statements.
Psychological safety emerges from consistent leadership behavior, not aspirational values statements. Leaders demonstrate safety through response patterns: how they handle vulnerability, whether they acknowledge their own challenges, and how they respond when employees share difficulties.
Observable indicators of psychological safety for mental health discussions:
- Leaders share appropriate personal experiences with challenges
- Mistakes and setbacks are framed as learning opportunities
- Vulnerability is met with support rather than judgment
- Workload and expectations adjust based on capacity conversations
- Privacy and confidentiality are rigorously protected
Organizations often underestimate how quickly trust erodes when confidentiality breaches occur or when disclosure leads to career consequences. A single incident of mishandled mental health information can silence an entire team for years.
Creating Conversational Architecture That Supports Disclosure
The structural elements of how conversations happen matter as much as the content. Mental health discussions benefit from intentional design around timing, privacy, and follow-through.
One-on-one conversations in private settings with adequate time allocation demonstrate respect for the significance of mental health topics. Rushed conversations in public spaces communicate the opposite, regardless of verbal assurances.
Regular check-ins that include wellbeing as a standard agenda item normalize mental health discussions rather than making them special events that signal crisis. This routine integration reduces the activation energy required for employees to raise concerns.
Training Managers to Facilitate Mental Health Discussions
Managers serve as the critical interface for workplace mental health discussions, yet most receive inadequate preparation for this responsibility. The gap between expectations and capability creates anxiety for managers and missed support opportunities for employees.
Effective manager training programs move beyond theoretical knowledge to develop practical conversational skills. Mental health first aid training provides structured frameworks that build confidence and competence in these pivotal conversations.
Core Competencies for Managers in Mental Health Conversations
Managers require specific skills that differ from general communication training. Mental health discussions demand particular attention to emotional regulation, boundary management, and resource connection.
Essential manager capabilities include:
- Initiating conversations when observing changes in performance, behavior, or wellbeing
- Active listening without rushing to fix, advise, or minimize concerns
- Validating experiences while maintaining appropriate professional boundaries
- Assessing risk levels to determine urgency of response
- Connecting to resources through clear referral pathways
- Following up consistently without becoming a therapeutic relationship
Many managers struggle most with the transition from listening to action. They either become overly involved in attempting to solve psychological issues beyond their scope, or they disengage entirely after initial conversation, leaving employees unsupported.
The skill of knowing what not to say often proves as important as knowing what to say. Managers trained to avoid minimizing language, unwanted advice, and premature problem-solving create space for authentic disclosure.
Addressing Stigma Through Intentional Language and Framing
Language choices in mental health discussions either reinforce or reduce stigma. Many organizations unknowingly perpetuate stigmatizing frameworks through casual terminology, deficit-focused framing, or separation of mental and physical health.
Person-first language that recognizes individuals beyond their mental health experiences represents one dimension of stigma reduction. Describing someone as “experiencing depression” rather than “a depressive” maintains dignity and acknowledges the distinction between identity and current state.
Strategic Communication Approaches That Normalize Mental Health
Organizations that successfully reduce stigma through mental health discussions employ consistent communication strategies across all levels. Beyond Blue provides guidelines on identifying trustworthy information and language frameworks that support constructive dialogue.
Effective framing strategies include:
- Integrating mental health with physical health in wellbeing communications
- Highlighting recovery and management rather than only challenges
- Sharing diverse stories that reflect various experiences and outcomes
- Using clinical terminology accurately rather than colloquialisms
- Emphasizing commonality of mental health experiences across populations
The shift from “mental health problems” to “mental health experiences” or “mental health conditions” represents subtle but meaningful linguistic evolution that reduces pathologizing undertones.
Organizations can assess their communication patterns by reviewing internal documents, email language, and meeting discussions for inadvertent stigmatizing content. This audit often reveals surprising patterns that undermine stated commitments to mental health support.
Navigating Confidentiality, Privacy, and Information Sharing
Confidentiality concerns represent one of the most significant barriers to open mental health discussions in workplace settings. Employees hesitate to disclose when boundaries around information sharing remain unclear or when previous experiences demonstrated inadequate privacy protection.
Leaders must establish and communicate explicit frameworks that outline what information remains confidential, what requires sharing for safety or accommodation purposes, and who has access to mental health-related information.
Confidentiality framework considerations:
| Scenario | Confidentiality Status | Sharing Protocol |
|---|---|---|
| Employee discloses stress | Fully confidential | No sharing without consent |
| Employee requests accommodation | Limited disclosure | Share only necessary details with relevant parties |
| Safety risk identified | Confidentiality limited | Immediate response team activation |
| Workers compensation claim | Documented disclosure | Follows legal requirements |
The principle of minimum necessary disclosure guides ethical information sharing. When accommodation or support requires informing others, only the specific information needed for that purpose should be shared, not comprehensive mental health details.
Balancing Duty of Care with Privacy Protection
Organizations face genuine tension between privacy obligations and duty of care responsibilities. This tension intensifies when employees resist support despite concerning indicators or when safety considerations emerge.
Clear policies established before crisis situations provide frameworks for these difficult decisions. Employees benefit from understanding in advance what circumstances might necessitate confidentiality limitations, rather than discovering boundaries during vulnerable moments.
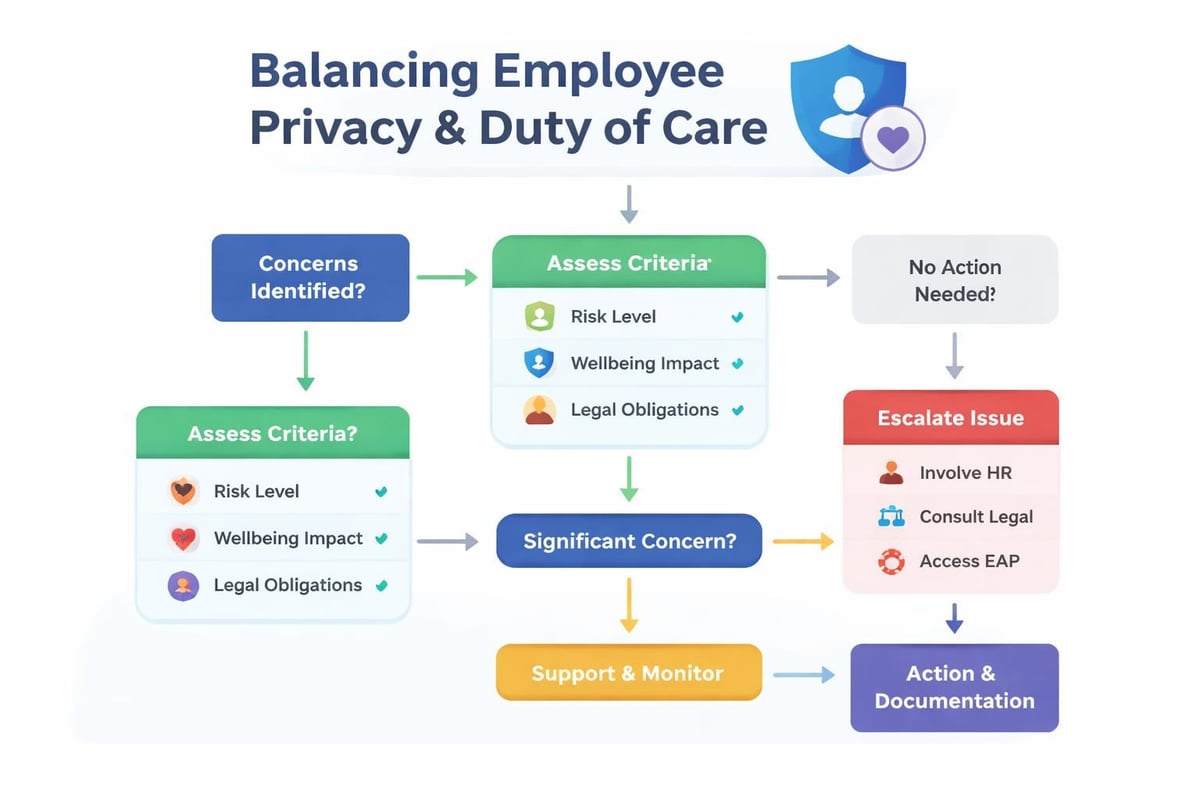
Transparency about these boundaries actually increases trust when communicated proactively. Employees appreciate knowing the parameters within which their disclosures will be protected and when organizational responsibility might require intervention.
Building Organizational Capacity Through Systematic Training
Individual capability matters less than systemic capacity when creating sustainable cultures of mental health discussion. Organizations that rely on a few trained champions create fragile systems vulnerable to turnover and inconsistent support quality.
Systematic training approaches ensure that mental health conversational competency exists throughout the organizational hierarchy. This includes executive leadership, middle management, frontline supervisors, and peer support networks.
Layered training architecture for mental health discussions:
- Executive awareness sessions focusing on strategic importance and resource allocation
- Manager skill development providing practical conversation frameworks and response protocols
- Employee education building recognition skills and help-seeking confidence
- Peer supporter training creating informal support networks within teams
- Specialist development for HR, wellbeing coordinators, and designated mental health roles
The U.S. Surgeon General’s Advisory highlights the importance of comprehensive approaches to mental health support that extend beyond individual interventions to organizational systems.
Measuring Quality and Impact of Mental Health Discussions
Organizations serious about mental health discussions implement measurement systems that track both conversation quality and downstream outcomes. Metrics provide accountability and identify improvement opportunities.
Quantitative measures might include help-seeking rates, Employee Assistance Program utilization, accommodation requests, and psychological safety survey results. These indicate whether the organizational environment supports disclosure and help-seeking.
Qualitative feedback through focus groups, exit interviews, and employee stories provides richness that numbers cannot capture. Employees can articulate whether mental health discussions feel genuine or performative, supportive or stigmatizing.
Creating Structured Opportunities for Mental Health Dialogue
While spontaneous mental health discussions matter, organizations benefit from creating intentional forums where these conversations are explicitly welcomed and structured for psychological safety.
Regular team check-ins that include wellbeing as a standard component normalize mental health as an ongoing consideration rather than a crisis response. These brief exchanges build relational foundation that makes deeper conversations possible when needed.
Structured mental health discussion forums:
- Weekly one-on-one meetings with wellbeing check-in protocols
- Monthly team wellbeing conversations focusing on workload and support
- Quarterly organizational listening sessions gathering employee input
- Annual wellbeing surveys with action planning based on results
- Peer support circles for voluntary participation and shared experience
The mindfulness practices integrated into workplace routines create natural entry points for mental health discussions by establishing contemplative space within the workday.
Leveraging Technology While Maintaining Human Connection
Digital platforms expand access to mental health discussions through chat-based support, virtual counseling, and asynchronous communication options. These tools particularly benefit employees who find face-to-face disclosure challenging.
However, technology should enhance rather than replace human connection in mental health discussions. The nuance, empathy, and relational trust that emerge through direct conversation cannot be fully replicated through digital interfaces.
Organizations achieve optimal outcomes by offering multiple pathways for mental health discussions that accommodate different preferences, needs, and comfort levels. Some employees will always prefer in-person conversation while others find digital channels more accessible.
Addressing Mental Health Discussions Across Diverse Workforces
Cultural background, gender identity, age, neurodiversity, and other dimensions of difference significantly influence how employees experience and engage with mental health discussions. One-size-fits-all approaches fail to create inclusive environments for these conversations.
Understanding cultural variations in mental health conceptualization, help-seeking patterns, and communication preferences enables leaders to adapt their approaches. What feels supportive in one cultural context may feel invasive or inappropriate in another.
Considerations for inclusive mental health discussions:
- Language accessibility for multilingual workforces
- Cultural humility regarding mental health beliefs and practices
- Gender-sensitive approaches that recognize different socialization patterns
- Generational differences in mental health literacy and disclosure comfort
- Neurodiversity-affirming communication that accommodates different processing styles
- Recognition of intersectionality and compounding marginalization
Organizations can partner with diverse employee resource groups to understand how mental health discussions land across different communities and what adaptations would increase accessibility and psychological safety.
Trauma-Informed Approaches to Workplace Conversations
Many employees carry trauma histories that shape how they experience workplace mental health discussions. Trauma-informed conversation practices recognize this reality and minimize potential for re-traumatization through organizational interactions.
Providing choice and control in conversation format, pacing, and disclosure level respects autonomy and reduces power dynamics that can feel threatening. Allowing employees to lead the conversation rather than extracting information through interrogation demonstrates trauma-informed practice.
The keynotes and presentations offered by mental health specialists can educate organizational leaders on trauma-informed frameworks that enhance conversation quality and safety.
Integrating Mental Health Discussions into Performance Management
The intersection of mental health discussions and performance management creates particular complexity. Organizations must address performance concerns while simultaneously supporting employee wellbeing, a balance that requires sophistication and care.
Separating performance conversations from mental health support discussions often serves both purposes better than attempting to address both simultaneously. When performance feedback occurs in the same conversation as mental health disclosure, employees may perceive their honesty as professionally risky.
Framework for addressing performance and mental health:
| Conversation Type | Purpose | Timing | Confidentiality |
|---|---|---|---|
| Performance feedback | Address work quality/output | Scheduled reviews | Standard performance records |
| Wellbeing check-in | Assess support needs | Regular intervals | Confidential to manager |
| Accommodation discussion | Explore adjustments | As needed | Limited disclosure |
| Support planning | Connect to resources | Following disclosure | Highly confidential |
When performance challenges stem from mental health conditions, the accommodation process provides a structured pathway that protects both employee rights and organizational needs. This formal process includes documentation requirements and involves HR expertise.
Prevention Through Workload and Culture Management
The most effective mental health discussions address systemic workplace stressors rather than only individual coping. Leaders who examine how workload, deadlines, resources, and culture contribute to mental health challenges demonstrate genuine commitment beyond surface-level support.
Regular conversations about team capacity, work distribution, and stress points enable proactive adjustment before performance deteriorates or mental health crises emerge. These discussions normalize acknowledging limits and requesting support as professional strengths rather than weaknesses.
Resources available through mental health training programs provide frameworks for these preventive conversations and organizational assessments.
Sustaining Mental Health Discussions Over Time
Initial enthusiasm for mental health discussions often wanes as competing priorities emerge and organizational attention shifts. Sustaining these conversations requires intentional systems that embed them into operational routines rather than treating them as temporary initiatives.
Leadership accountability mechanisms ensure that mental health discussions remain priorities even when other pressures intensify. Including wellbeing conversation quality in leadership performance expectations signals genuine organizational commitment.
Sustainability strategies for mental health discussions:
- Integrate wellbeing metrics into business performance dashboards
- Include mental health conversation skills in leadership development programs
- Allocate dedicated time in meeting agendas for wellbeing discussions
- Celebrate and recognize leaders who excel at these conversations
- Continuously refresh training as staff turns over and best practices evolve
The Behavioral Health Barometer provides data on mental health indicators that can inform organizational tracking and improvement efforts over time.
Organizations that view mental health discussions as fundamental to operational excellence rather than supplementary wellbeing programming achieve deeper integration and longer-term sustainability. When these conversations connect directly to productivity, retention, innovation, and other business outcomes, they receive consistent prioritization.
Mental health discussions represent both a cultural shift and a practical skill set that organizations must develop intentionally and sustain systematically. Leaders who invest in building genuine conversational capacity, psychological safety, and systemic support structures create workplaces where employees can bring their full selves and access help when needed. Workplace Mental Health Institute provides comprehensive training programs, strategic consultation, and evidence-based resources that equip managers and organizations with the tools to transform mental health discussions from aspiration to operational reality.


