Depression and anxiety at work represent two of the most prevalent yet often misunderstood mental health challenges facing modern organizations. These conditions affect not only individual employees but also team dynamics, productivity, and organizational culture. For leaders and HR professionals, understanding the distinct characteristics, overlapping symptoms, and workplace implications of depression and anxiety at work is fundamental to creating supportive environments. This comprehensive guide provides evidence-based strategies for recognizing, addressing, and preventing these conditions within professional settings.
Understanding Depression and Anxiety as Distinct Conditions
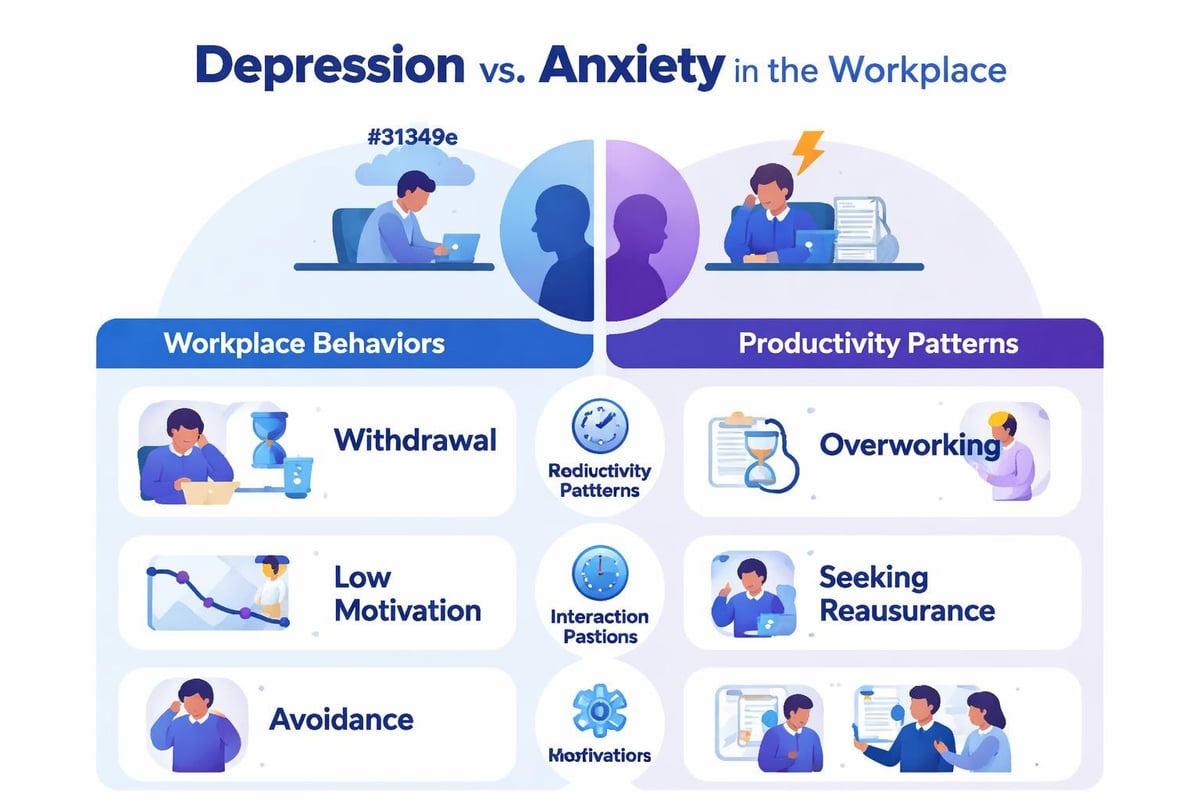
While frequently mentioned together, depression and anxiety present differently in workplace contexts. Depression typically manifests as persistent low mood, loss of interest in previously enjoyable activities, and diminished energy that affects work performance over extended periods. Employees experiencing depression may struggle with concentration, decision-making, and maintaining consistent productivity levels.
Anxiety, conversely, centers on excessive worry, heightened arousal, and anticipatory distress about future events or outcomes. At work, this might appear as perfectionism, difficulty delegating, procrastination driven by fear of failure, or physical symptoms like tension headaches and digestive issues.
Key Diagnostic Distinctions
Understanding these conditions requires moving beyond surface observations:
- Depression indicators: Persistent sadness, withdrawal from colleagues, decreased motivation, changes in work quality, increased absenteeism, expressions of hopelessness
- Anxiety indicators: Restlessness, irritability, difficulty concentrating due to racing thoughts, avoidance of challenging tasks, excessive reassurance-seeking, physical tension
- Comorbidity factors: Approximately 60% of individuals with depression also experience anxiety symptoms, creating complex presentation patterns
| Characteristic | Depression | Anxiety |
|---|---|---|
| Primary emotion | Sadness, emptiness | Fear, apprehension |
| Energy level | Low, fatigued | Agitated, tense |
| Time orientation | Past-focused rumination | Future-focused worry |
| Work impact | Reduced output, disengagement | Perfectionism, overwork |
| Physical symptoms | Fatigue, sleep changes | Muscle tension, restlessness |
The Organizational Impact of Untreated Mental Health Conditions
Research examining anxiety and depression effects on organizations demonstrates significant consequences beyond individual suffering. Depression and anxiety at work generate measurable costs through multiple pathways that leaders must recognize.
Presenteeism-when employees attend work while unwell-often exceeds absenteeism costs. Workers experiencing depression or anxiety may be physically present but cognitively impaired, producing lower-quality work, making more errors, and requiring additional supervision. Studies indicate presenteeism can reduce productivity by 35-50% for affected individuals.
Quantifiable Business Consequences
Organizations face several measurable impacts:
- Increased absenteeism rates: Employees with depression take an average of 7-10 additional sick days annually compared to peers
- Elevated turnover costs: Mental health conditions contribute to 30-40% higher voluntary turnover rates
- Reduced team performance: Team productivity decreases when members experience untreated mental health challenges
- Safety incidents: Depression and anxiety correlate with increased workplace accidents and injuries
- Healthcare expenditure: Organizations see 4-6 times higher healthcare costs for employees with untreated mental health conditions
The CDC emphasizes supporting worker mental health as essential for organizational sustainability. Beyond direct costs, untreated depression and anxiety at work erode workplace culture, diminish innovation, and create ripple effects throughout teams.
Risk Factors and Environmental Contributors
Workplace environments themselves can precipitate or exacerbate mental health conditions. Understanding these risk factors enables preventative intervention rather than reactive crisis management.
Research on low control environments identifies autonomy deficits as significant contributors to both depression and anxiety. Employees who lack decision-making authority, face unpredictable schedules, or experience micromanagement show substantially elevated risk for developing these conditions.
Organizational Risk Factors
- Job design issues: Role ambiguity, conflicting demands, excessive workload, insufficient resources
- Leadership behaviors: Inconsistent communication, lack of recognition, punitive management styles, absent support structures
- Cultural elements: Stigma around mental health, presenteeism expectations, competitive rather than collaborative norms
- Structural factors: Job insecurity, limited advancement opportunities, inadequate work-life integration policies
Certain sectors face amplified risk. Healthcare workers, for example, experience elevated rates of depression and anxiety due to emotional demands, staffing shortages, and exposure to traumatic situations. The Workplace Mental Health Institute’s specialized programs address these sector-specific challenges through targeted training interventions.

Recognition and Early Identification Strategies
Managers and HR professionals serve as frontline observers who can identify concerning changes before conditions become severe. Early recognition enables timely support and prevents deterioration that affects both individuals and teams.
Observable Workplace Changes
Leaders should note patterns rather than isolated incidents:
- Performance fluctuations: Inconsistent work quality, missed deadlines, uncharacteristic errors
- Behavioral shifts: Withdrawal from team activities, increased irritability, changes in communication patterns
- Physical indicators: Visible fatigue, frequent illness, changes in appearance or personal care
- Attendance patterns: Increased sick leave, arriving late, leaving early, extended breaks
- Interpersonal dynamics: Conflict with colleagues, reduced collaboration, isolation
Effective identification requires psychological safety. Employees must trust that disclosing struggles won’t result in career penalties. Organizations implementing healthy workplace strategies report higher disclosure rates and earlier intervention opportunities.
Manager Capability Development
Training managers to recognize depression and anxiety at work constitutes essential infrastructure. Evidence-based training programs equip leaders with:
- Conversation frameworks for expressing concern without diagnosing
- Active listening techniques that encourage disclosure
- Referral pathways to appropriate support resources
- Strategies for reasonable workplace adjustments
- Self-care approaches to prevent vicarious trauma
Managers need not become therapists, but they must develop literacy around mental health presentations and organizational response protocols.
Evidence-Based Intervention Approaches
Once depression or anxiety at work is identified, organizations must activate appropriate support mechanisms. Effective intervention balances individual support with systemic improvements.
Individual-Level Supports
| Intervention Type | Description | Evidence Strength |
|---|---|---|
| Employee Assistance Programs | Confidential counseling services, typically 6-8 sessions | Moderate to high |
| Workplace adjustments | Modified duties, flexible scheduling, workload reallocation | High |
| Return-to-work planning | Gradual reintegration with ongoing support | High |
| Peer support programs | Trained colleague support networks | Moderate |
| Mental health days | Designated time off for psychological recovery | Emerging positive evidence |
Information needs research demonstrates that employees value accurate, accessible information about their conditions. Organizations should provide psychoeducational resources explaining depression and anxiety, available supports, and recovery trajectories.
Organizational-Level Interventions
Systemic changes address root causes rather than merely treating symptoms:
- Job redesign initiatives: Increasing autonomy, clarifying roles, ensuring adequate staffing
- Leadership development: Training in supportive management practices and psychological safety creation
- Policy reform: Implementing flexible work arrangements, reasonable workload standards, anti-stigma protocols
- Culture building: Normalizing mental health conversations, celebrating help-seeking, modeling senior leadership disclosure
The Workplace Mental Health Institute’s assessment services help Australian organizations identify systemic contributors to depression and anxiety at work, enabling targeted interventions that improve conditions for all employees.
Preventative Strategies and Resilience Building
Prevention surpasses intervention in both effectiveness and cost-efficiency. Organizations investing in mental health infrastructure before crises emerge demonstrate superior outcomes across wellbeing and performance metrics.
Organizational Prevention Framework
Building resilience requires multi-level approaches:
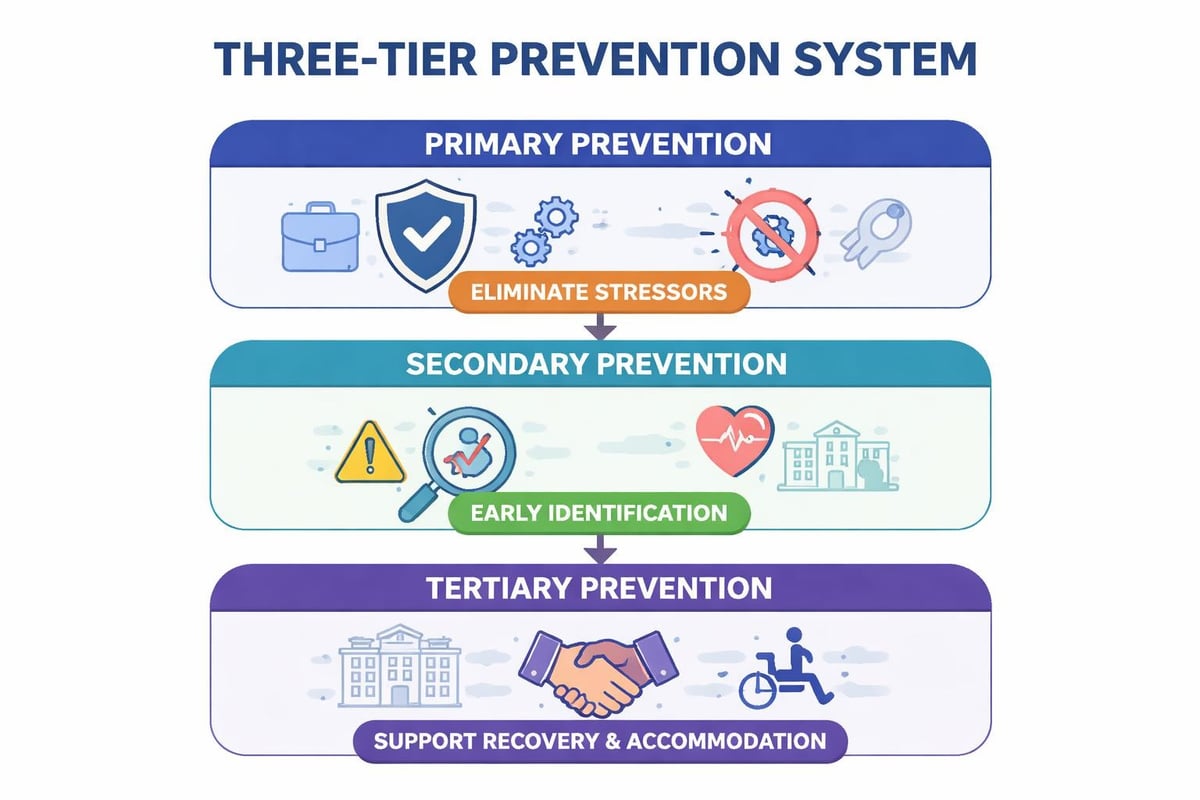
- Primary prevention: Eliminating or reducing workplace stressors through job design, reasonable workloads, and supportive leadership
- Secondary prevention: Early identification systems, regular wellbeing check-ins, accessible mental health literacy training
- Tertiary prevention: Comprehensive return-to-work programs, ongoing accommodation processes, sustained support structures
Resilience development extends beyond individual coping skills. While personal resilience matters, organizational resilience-the capacity of systems to support employee wellbeing during challenges-provides more sustainable protection against depression and anxiety at work.
Manager Training as Prevention Infrastructure
Investing in manager capability represents one of the highest-impact preventative interventions. Trained managers create psychologically safe teams, recognize early warning signs, respond supportively to disclosures, and model healthy work practices.
Effective manager training programs incorporate:
- Psychological health literacy: Understanding mental health conditions, risk factors, and protective factors
- Conversation skills: Having supportive discussions about wellbeing without overstepping professional boundaries
- Referral knowledge: Connecting team members with appropriate internal and external resources
- Boundary management: Balancing support with professional role limitations
- Self-care practices: Maintaining personal wellbeing while supporting others
The Workplace Mental Health Institute’s training portfolio demonstrates these principles through practical, skills-based approaches that managers can immediately implement.
Legal and Ethical Considerations
Organizations navigating depression and anxiety at work must balance support with legal obligations and ethical responsibilities. Understanding these frameworks prevents inadvertent harm while ensuring compliance.
Accommodation Requirements
Most jurisdictions require reasonable accommodations for employees with mental health conditions. These might include:
- Modified work schedules or remote work options
- Reduced or redistributed workload during treatment
- Quiet workspace or sensory accommodations
- Additional breaks or flexible leave arrangements
- Graduated return-to-work plans following absence
Accommodations should emerge from collaborative discussions between employees, managers, and HR professionals. The interactive process respects employee autonomy while addressing organizational needs.
Privacy and Confidentiality Obligations
Managers frequently struggle with information-sharing boundaries. Clear protocols should specify:
- What managers need to know: Sufficient information to implement accommodations and provide support
- What remains confidential: Specific diagnoses, treatment details, personal circumstances
- Who needs notification: Only those with legitimate business needs related to accommodation or safety
- Documentation requirements: Necessary paperwork for formal accommodation processes
- Employee consent processes: Obtaining explicit permission before sharing any health-related information
Ethical practice prioritizes employee dignity, autonomy, and privacy while meeting organizational compliance requirements.
Creating Sustainable Support Systems
Addressing depression and anxiety at work requires sustained commitment rather than one-time initiatives. Organizations that embed mental health support into operational practices achieve superior long-term outcomes.
Integration Strategies
Sustainable systems incorporate mental health considerations into existing processes:
- Performance management: Including wellbeing conversations in regular check-ins, separating support discussions from evaluative processes
- Onboarding programs: Introducing mental health resources, destigmatizing help-seeking from day one
- Exit interviews: Gathering data on mental health factors influencing turnover decisions
- Leadership development: Making psychological safety and team wellbeing core leadership competencies
- Strategic planning: Allocating resources for mental health infrastructure alongside other business priorities
These integration points normalize mental health as fundamental to operational excellence rather than peripheral HR concern.
Measurement and Continuous Improvement
Organizations should track relevant metrics to evaluate intervention effectiveness:
| Metric Category | Example Measures |
|---|---|
| Prevalence indicators | Self-reported wellbeing scores, psychological safety indices, stress levels |
| Impact measures | Absenteeism rates, turnover statistics, productivity metrics, engagement scores |
| Utilization data | EAP usage rates, training completion, accommodation requests, policy awareness |
| Climate indicators | Stigma assessments, help-seeking comfort levels, perceived leadership support |
Regular measurement enables data-driven refinement of strategies addressing depression and anxiety at work.
The Role of Specialized Training and Development
Comprehensive organizational response to mental health challenges requires capability development across all levels. Strategic investment in training yields returns through improved early identification, more effective support, and reduced mental health-related costs.
Training Priorities by Role
Different organizational roles require tailored mental health competencies:
- Senior leaders: Strategic mental health planning, resource allocation, anti-stigma modeling, culture setting
- Middle managers: Recognition skills, supportive conversations, accommodation implementation, team psychological safety
- HR professionals: Policy development, accommodation processes, legal compliance, program design and evaluation
- All employees: Mental health literacy, self-care strategies, peer support skills, help-seeking confidence
Organizations partnering with specialized providers access evidence-based content, experienced facilitators, and measurable capability development. Workplace Mental Health Institute’s offerings span these role-specific needs through customizable programs that address unique organizational contexts.
Effectively addressing depression and anxiety at work requires organizations to move beyond awareness toward comprehensive, evidence-based action. By understanding these conditions as distinct yet often co-occurring challenges, implementing multilevel prevention and intervention strategies, and building sustainable support infrastructure, organizations protect both employee wellbeing and business performance. Workplace Mental Health Institute provides the specialized training, assessment, and strategic consultation services that transform mental health from organizational risk to competitive advantage through practical, empowering approaches tailored to your workforce needs.
