Nurses encounter mental health challenges across every healthcare setting, from emergency departments to aged care facilities. The demand for specialized mental health training for nurses has intensified as healthcare systems recognize that psychological wellbeing intersects with physical health outcomes in nearly every patient interaction. With approximately one in five adults experiencing mental illness annually, nurses require sophisticated competencies beyond basic awareness to deliver effective, compassionate care while protecting their own psychological resilience.
Core Competencies in Nursing Mental Health Education
Mental health training for nurses must address both clinical knowledge and interpersonal skills. Effective programs build competency across multiple domains rather than treating mental health as a standalone specialty concern.
Essential Knowledge Domains
Nurses require foundational understanding in psychopathology, psychopharmacology, and evidence-based interventions. Training should cover major diagnostic categories including mood disorders, anxiety conditions, psychotic disorders, substance use disorders, and personality disorders. However, knowledge acquisition alone proves insufficient without application skills.
Critical competency areas include:
- Recognition of early warning signs and symptom presentation
- Risk assessment for self-harm and harm to others
- De-escalation techniques for agitated or distressed patients
- Trauma-informed communication approaches
- Cultural competency in mental health contexts
- Legal and ethical considerations in psychiatric care

Understanding psychopharmacology extends beyond medication names to mechanism of action, side effect profiles, and monitoring requirements. Nurses must recognize adverse effects quickly, particularly extrapyramidal symptoms, serotonin syndrome, and metabolic changes associated with psychiatric medications.
Therapeutic Communication Skills
The therapeutic relationship forms the foundation of effective mental health nursing. Training programs must provide opportunities for skill practice, not merely theoretical instruction.
Advanced communication techniques include motivational interviewing, cognitive-behavioral approaches, and solution-focused strategies. Nurses learn to balance empathy with professional boundaries, validate patient experiences while encouraging adaptive coping, and respond therapeutically to challenging behaviors.
| Communication Technique | Application | Expected Outcome |
|---|---|---|
| Motivational Interviewing | Ambivalence about treatment | Enhanced treatment engagement |
| Validation Therapy | Emotional dysregulation | Reduced distress, improved rapport |
| De-escalation Protocols | Aggressive behavior | Safety maintenance, crisis resolution |
| Reflective Listening | Emotional expression | Deeper therapeutic alliance |
Programs from Workplace Mental Health Institute emphasize practical application of communication frameworks within workplace contexts, recognizing that nurses apply these skills with colleagues and patients alike.
Certification Pathways and Specialized Training
Professional certification demonstrates advanced competency in psychiatric and mental health nursing. Multiple pathways exist depending on educational background and career objectives.
Psychiatric-Mental Health Nursing Certification
The American Nurses Credentialing Center offers certification for both registered nurses and advanced practice nurses. The Psychiatric-Mental Health Nursing certification requires current RN licensure, specific practice hours, and successful examination completion. Reference materials for certification cover comprehensive content domains from neurobiology to therapeutic modalities.
Advanced practice certification as a Psychiatric-Mental Health Nurse Practitioner requires master’s or doctoral preparation with specialized clinical training hours. These practitioners function autonomously, providing diagnostic assessment, psychotherapy, and prescriptive authority in many jurisdictions.
Certification benefits include:
- Enhanced clinical competency and confidence
- Career advancement opportunities
- Salary increases averaging 10-15%
- Professional recognition and credibility
- Improved patient outcomes through specialized expertise
Global Standards and Academic Credentials
Mental health nursing credentials vary internationally, with different educational requirements and scope of practice definitions. Global academic credentials for psychiatric-mental health nursing reflect diverse healthcare system structures and regulatory frameworks.
Australian nurses pursuing mental health specialization can access resources through WMHI Australia, which provides region-specific training aligned with local clinical guidelines and workplace requirements.
European models often integrate mental health content throughout generalist nursing education, while North American systems favor post-registration specialization. Understanding these variations proves valuable for internationally educated nurses and organizations with diverse workforces.
Evidence-Based Training Methodologies
Effective mental health training for nurses employs multiple pedagogical approaches rather than relying solely on didactic instruction.
Simulation-Based Learning
High-fidelity simulation creates safe environments for practicing crisis intervention, therapeutic communication, and clinical decision-making. Scenarios replicate acute psychiatric presentations including suicidal ideation, psychotic episodes, and violent behavior.
Debriefing following simulation exercises reinforces learning through structured reflection. Facilitators guide participants to analyze decision-making processes, identify alternative approaches, and consolidate knowledge application.
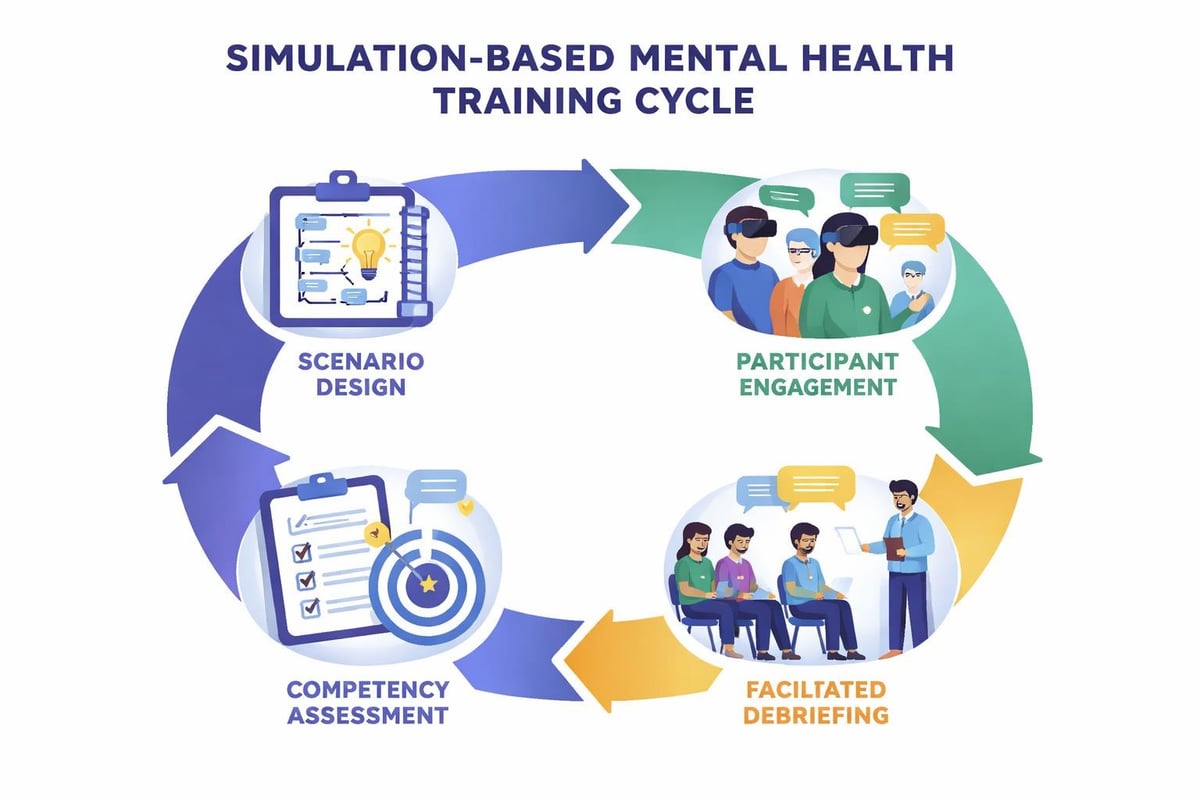
Research demonstrates that simulation-based training significantly improves confidence and competence in psychiatric nursing skills. The controlled environment allows repeated practice without patient risk, accelerating skill acquisition beyond traditional clinical placement limitations.
Mental Health First Aid Integration
Mental Health First Aid training specifically designed for nurses enhances behavioral health knowledge and intervention capabilities. This evidence-based program teaches systematic approaches to identifying mental health crises, providing initial assistance, and connecting individuals with appropriate professional resources.
Unlike general Mental Health First Aid, nurse-specific versions incorporate clinical context and professional responsibilities. Participants learn to apply first aid principles while maintaining therapeutic boundaries and professional standards.
The program typically covers five major psychiatric emergencies:
- Suicidal thoughts or behaviors
- Panic attacks and acute anxiety
- Psychotic episodes
- Substance overdose
- Acute stress reactions
Organizations implementing Mental Health First Aid report improved early intervention rates, reduced emergency department presentations, and enhanced team confidence in managing psychological crises.
Workplace Application and Organizational Integration
Mental health training for nurses achieves maximum impact when integrated into broader organizational wellness strategies rather than treated as isolated professional development.
Creating Psychologically Safe Practice Environments
Training effectiveness diminishes when workplace culture undermines learned principles. Healthcare organizations must address systemic factors including workload pressures, inadequate staffing, and moral injury risks that compromise both nurse wellbeing and patient care quality.
| Organizational Factor | Impact on Training Transfer | Mitigation Strategy |
|---|---|---|
| High patient-to-nurse ratios | Limited time for therapeutic engagement | Workload rebalancing, skill mix optimization |
| Inadequate supervision | Skill decay, reduced confidence | Regular case consultation, peer support |
| Stigmatizing attitudes | Reduced disclosure, help-seeking | Leadership modeling, policy reform |
| Insufficient resources | Incomplete care pathways | Service mapping, referral protocols |
Training programs from WMHI Online address organizational context, equipping participants to navigate system constraints while advocating for necessary resources and supports.
Trauma-Informed Care Implementation
Trauma-informed approaches recognize that many patients have experienced trauma that influences current presentation and treatment engagement. Mental health training for nurses increasingly incorporates trauma-informed principles as foundational rather than specialty knowledge.
The six key principles guiding trauma-informed care include safety, trustworthiness and transparency, peer support, collaboration and mutuality, empowerment, and cultural humility. Nurses trained in these frameworks demonstrate increased sensitivity to trauma triggers, reduced use of coercive interventions, and improved therapeutic relationships.
Implementation requires both individual skill development and systemic policy alignment. Organizations must examine practices that may inadvertently re-traumatize patients, including unnecessary restraint use, authoritarian communication styles, and inflexible protocols that ignore individual needs.
Specialized Populations and Context-Specific Training
Different clinical settings and patient populations require tailored mental health competencies beyond generalist training.
Perinatal Mental Health
Perinatal and postpartum mental health conditions affect approximately 15-20% of new mothers, yet many nurses lack confidence in screening, assessment, and support provision. Specialized training addresses mood and anxiety disorders during pregnancy and postpartum, psychosis risk factors, and bonding difficulties.
Essential perinatal mental health competencies:
- Administration and interpretation of validated screening tools
- Differentiation between “baby blues” and clinical depression
- Recognition of postpartum psychosis warning signs
- Supportive counseling techniques for new parents
- Appropriate referral pathways and collaborative care models
Aged Care and Dementia Contexts
Mental health presentations in older adults frequently differ from working-age populations, with depression often manifesting as cognitive complaints, social withdrawal, or somatic symptoms rather than expressed sadness. Training must address the intersection of mental health, cognitive decline, and physical comorbidities.
Behavioral and psychological symptoms of dementia (BPSD) require specialized approaches combining environmental modification, person-centered care, and judicious medication use. Nurses trained in dementia-specific mental health strategies demonstrate improved management of agitation, wandering, and other challenging behaviors while reducing antipsychotic medication reliance.
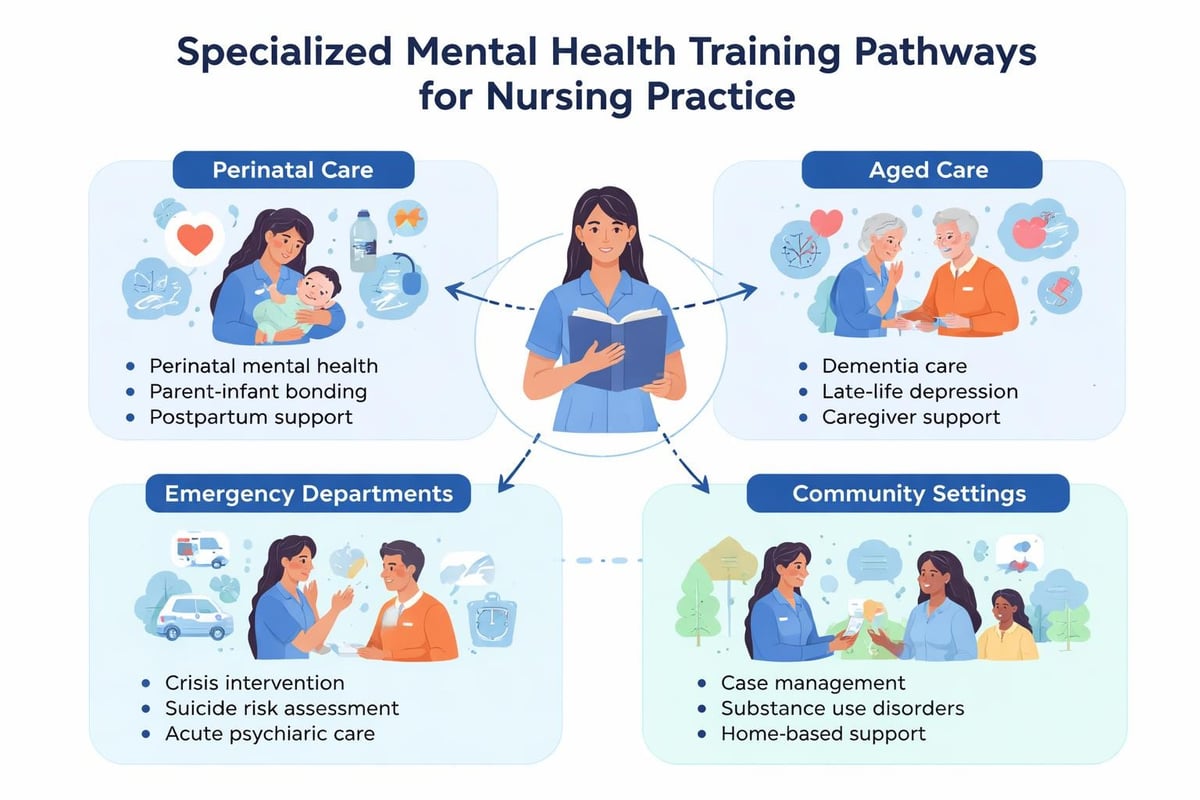
Emergency and Acute Care Settings
Emergency departments have become de facto psychiatric crisis centers in many communities. ED nurses require rapid assessment skills, safety management capabilities, and disposition decision-making frameworks.
Training for acute settings emphasizes brief interventions, violence risk assessment, medical clearance protocols for psychiatric presentations, and effective handover to mental health specialists. The high-pressure environment demands efficient yet compassionate approaches that maintain therapeutic principles despite time constraints.
Measuring Training Effectiveness and Outcomes
Robust evaluation distinguishes effective mental health training for nurses from programs that generate positive participant feedback but limited practice change.
Kirkpatrick’s Four Levels Applied
The Kirkpatrick model provides a framework for comprehensive training evaluation across reaction, learning, behavior, and results levels.
- Reaction: Participant satisfaction and perceived relevance
- Learning: Knowledge acquisition and skill demonstration
- Behavior: Practice change and skill application in clinical settings
- Results: Patient outcomes, safety metrics, and organizational performance
Most training programs assess reaction and learning levels adequately but fail to measure behavior change and clinical outcomes. Meaningful evaluation requires workplace observation, chart audits, patient feedback, and longitudinal outcome tracking.
Key Performance Indicators
Organizations implementing mental health training should monitor multiple indicators to assess impact comprehensively.
Pre- and post-training comparison metrics include:
- Mental health-related incident rates
- Restraint and seclusion frequency
- Patient satisfaction scores for psychological care
- Nurse confidence ratings in managing psychiatric presentations
- Referral appropriateness and timeliness
- Documentation quality for mental status assessments
- Staff psychological safety and wellbeing measures
Sustained improvement requires ongoing reinforcement through case discussions, refresher training, and embedded workplace supports rather than one-time educational events.
Continuous Professional Development Models
Mental health competency requires ongoing development rather than single-point training completion. Healthcare organizations should embed continuous learning opportunities into standard practice.
Communities of Practice
Establishing mental health communities of practice creates peer learning networks where nurses share challenges, discuss complex cases, and collectively develop expertise. Regular meetings might focus on specific diagnoses, intervention techniques, or ethical dilemmas encountered in practice.
These communities foster psychological safety for discussing uncertainty and mistakes, which accelerates learning beyond formal training contexts. Facilitated reflection on real cases proves more impactful than abstract educational content for many practitioners.
Integrated Learning Pathways
Progressive skill development through tiered training creates clear advancement pathways from foundational awareness to advanced specialist competency.
| Career Stage | Training Focus | Competency Level |
|---|---|---|
| Graduate Nurse | Recognition, basic communication, safety | Foundation |
| Experienced RN | Assessment, intervention planning, brief therapy | Intermediate |
| Advanced Practice | Diagnosis, psychotherapy, prescribing | Advanced |
| Clinical Leadership | Program development, consultation, supervision | Expert |
This structured approach allows organizations to match training investment with role requirements while providing career development pathways that retain skilled mental health nursing staff.
Resources available through the Workplace Mental Health Institute YouTube channel provide accessible refresher content and emerging topic coverage supporting continuous professional development.
Addressing Nurse Wellbeing Through Training
Mental health training for nurses must include content addressing practitioner wellbeing and resilience. Nurses experiencing psychological distress demonstrate reduced empathy, increased errors, and higher burnout rates.
Vicarious Trauma and Compassion Fatigue
Repeated exposure to patient trauma and suffering creates cumulative psychological impact even without direct personal threat. Training should normalize these experiences while providing concrete strategies for processing difficult cases and maintaining boundaries.
Evidence-based resilience techniques include regular supervision, peer debriefing protocols, mindfulness practices, and organizational support systems. However, individual resilience strategies prove insufficient without addressing systemic workplace stressors including understaffing, inadequate resources, and organizational injustice.
Help-Seeking and Stigma Reduction
Many nurses hesitate to access mental health support due to professional stigma, confidentiality concerns, and fears regarding licensure implications. Training programs that incorporate stigma reduction content demonstrate improved help-seeking behavior among participants.
Organizations should establish clear, confidential support pathways separate from performance management systems. Modeling help-seeking at leadership levels reduces stigma more effectively than educational content alone.
Mental health training for nurses represents a critical investment in healthcare quality, patient safety, and workforce sustainability. Comprehensive programs that combine evidence-based content, practical skill development, and organizational integration deliver measurable improvements in clinical outcomes and nurse confidence. Workplace Mental Health Institute provides specialized training and consultation services designed specifically for healthcare organizations seeking to enhance mental health competency across their nursing workforce, offering practical, evidence-informed programs that translate directly into improved workplace performance and employee wellbeing.


