Depression in the workplace represents one of the most significant yet frequently misunderstood challenges facing modern organizations. Affecting approximately one in five employees at some point during their careers, this condition extends far beyond individual suffering to impact team dynamics, organizational productivity, and workplace safety. For leaders and HR professionals, understanding the nuances of workplace depression and developing responsive strategies has become an essential competency rather than an optional consideration.
Understanding Depression as a Workplace Issue
Depression manifests differently in professional settings than in personal life. While clinical depression involves persistent low mood, loss of interest, and changes in sleep or appetite, workplace-specific indicators often appear more subtle. Employees may exhibit increased absenteeism, declining work quality, difficulty concentrating during meetings, or withdrawal from team interactions.
The economic burden of depression extends across multiple organizational dimensions. Direct costs include medical expenses and short-term disability claims, while indirect costs encompass reduced productivity, increased turnover, and workplace accidents. Research consistently demonstrates that untreated depression affects not only the individual but creates ripple effects throughout teams and departments.
The Distinction Between Clinical and Situational Depression
Leaders must recognize the difference between clinical depression and temporary low mood triggered by specific workplace stressors. Clinical depression persists regardless of circumstances and requires professional intervention. Situational depression may arise from specific challenges such as role changes, interpersonal conflicts, or excessive workload demands.
Key distinguishing factors include:
- Duration of symptoms (clinical depression persists beyond two weeks)
- Impact on multiple life domains versus work-specific concerns
- Response to environmental changes or support interventions
- Presence of physical symptoms including fatigue, pain, or sleep disturbance
Neither form should be dismissed, yet each requires different organizational responses. Comprehensive mental health training equips managers to recognize these distinctions and respond appropriately.

The Performance Impact of Untreated Depression
Depression in the workplace creates measurable performance deficits that extend beyond simple absenteeism. The concept of “presenteeism” describes employees physically present but functioning at reduced capacity due to mental health challenges. Studies indicate that presenteeism costs organizations more than direct absenteeism, as decreased cognitive function, slower decision-making, and reduced creativity persist invisibly.
Research published in scientific literature demonstrates how anxiety and depression compromise individual performance while simultaneously affecting organizational safety. Employees experiencing depression show impaired attention, delayed reaction times, and reduced problem-solving capacity, all critical factors in safety-sensitive environments.
| Performance Domain | Impact of Depression | Organizational Consequence |
|---|---|---|
| Cognitive Processing | 35-40% reduction in executive function | Delayed projects, quality errors |
| Interpersonal Relations | Withdrawal, reduced collaboration | Team dysfunction, conflict |
| Decision-Making | Risk aversion, analysis paralysis | Missed opportunities, stagnation |
| Physical Safety | Reduced attention, slower reactions | Increased incident rates |
The workplace mental health research emphasizes that addressing depression proactively reduces these performance impacts significantly. Organizations implementing early intervention programs report substantial improvements in productivity metrics and employee engagement scores.
Creating Psychologically Safe Environments
Psychological safety forms the foundation for addressing depression in the workplace effectively. Employees must trust that disclosing mental health challenges will not result in career penalties, stigmatization, or discrimination. Leaders set the tone through their responses to mental health discussions and their willingness to prioritize wellbeing alongside performance outcomes.
Leadership Behaviors That Promote Safety
Managers demonstrate psychological safety through specific, observable behaviors rather than abstract commitments. Effective leaders normalize mental health conversations, share appropriate vulnerability, and respond compassionately when employees disclose challenges.
Essential leadership practices include:
- Using inclusive language that acknowledges mental health as part of overall wellbeing
- Addressing workload concerns proactively before employees reach crisis points
- Providing flexible work arrangements when appropriate
- Maintaining confidentiality while connecting employees with resources
- Following up consistently after employees return from mental health leave
Training programs offered through workplace mental health specialists develop these competencies systematically, moving beyond awareness to practical skill development.
Structural Supports Beyond Individual Interventions
While manager training proves essential, organizational systems must support mental health comprehensively. Policies regarding workload management, leave flexibility, and reasonable accommodations require regular review and updating. Employee assistance programs should offer timely access to qualified mental health professionals rather than serving as bureaucratic obstacles.
Workplace wellbeing assessments identify systemic factors contributing to depression, including excessive demands, inadequate resources, role ambiguity, or toxic team dynamics. Addressing these structural issues prevents depression more effectively than individual interventions alone.
Recognition and Early Intervention Strategies
Early recognition of depression in the workplace enables intervention before significant performance decline or personal crisis occurs. Managers trained in mental health literacy identify concerning patterns while avoiding diagnosis or overstepping professional boundaries.
Observable indicators requiring attention include persistent changes in behavior, performance, or interpersonal interactions. A previously collaborative employee who becomes withdrawn, a high performer whose quality suddenly declines, or a team member who appears consistently exhausted despite adequate time off all warrant compassionate inquiry.
The Role of Structured Conversations
Effective early intervention relies on structured, supportive conversations rather than informal check-ins. Managers should prepare for these discussions, choosing private settings and allocating sufficient time. The conversation focuses on observable behaviors and their impact rather than personal speculation about mental health conditions.
Conversation framework:
- Open with specific observations: “I’ve noticed you’ve missed several deadlines recently, which is unusual for you.”
- Express genuine concern: “I’m concerned about how you’re doing and want to make sure you have the support you need.”
- Listen without judgment or immediate problem-solving
- Offer specific resources including EAP, flexible arrangements, or workload adjustments
- Document the conversation appropriately while maintaining confidentiality
Resources from mental health organizations provide additional guidance on conducting these sensitive conversations effectively. The Institute for Work & Health offers evidence-informed approaches that integrate research with practical application.
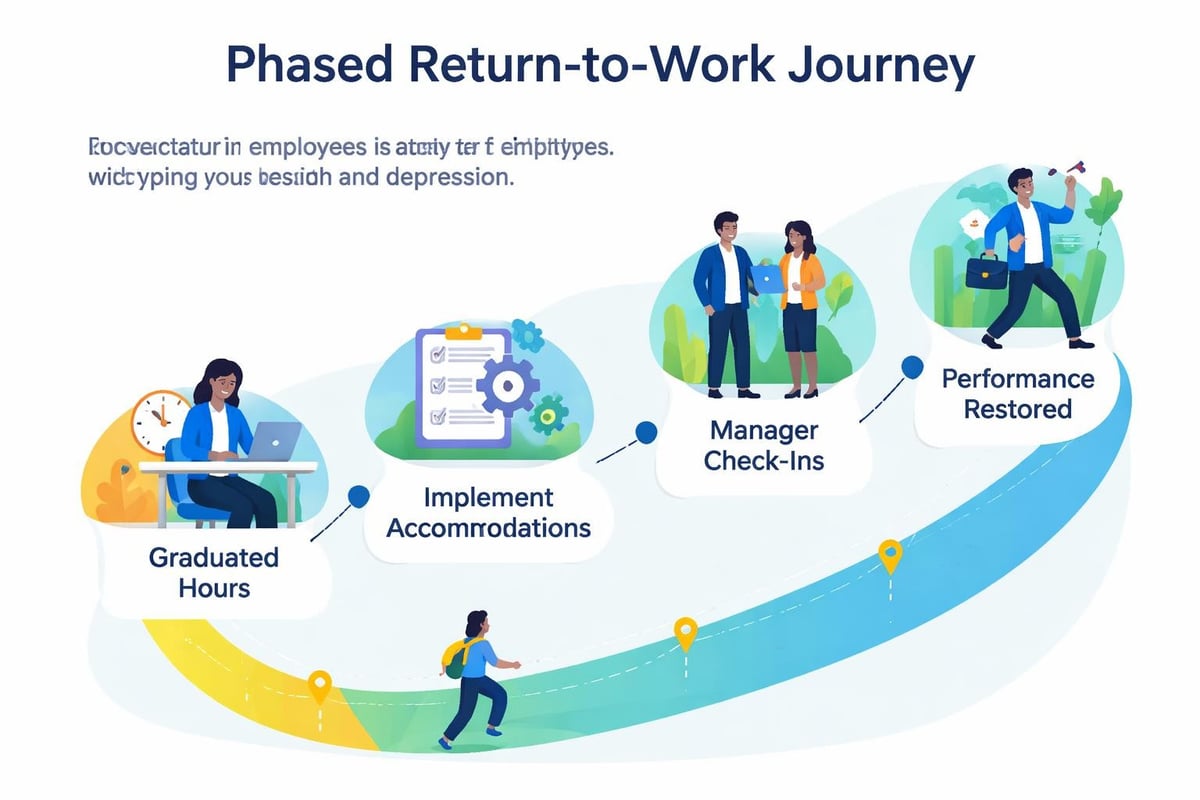
Accommodation and Return-to-Work Processes
When employees require time away for depression treatment, thoughtful return-to-work planning facilitates successful reintegration. Graduated return schedules, temporary workload reductions, or modified duties support employees while maintaining team functionality.
Legal frameworks in many jurisdictions require reasonable accommodations for mental health conditions equivalent to physical health issues. Leaders familiar with accommodation processes navigate these requirements confidently while supporting employee recovery.
| Accommodation Type | Application | Duration |
|---|---|---|
| Reduced Hours | Gradual increase from part-time to full-time | 2-6 weeks |
| Modified Duties | Temporary removal of high-stress tasks | 4-12 weeks |
| Flexible Scheduling | Self-directed start/end times | Ongoing as needed |
| Workload Adjustment | Reduction in project volume or complexity | Reassess monthly |
Communication during leave and return requires balance between maintaining connection and respecting boundaries. Regular check-ins should focus on practical matters rather than recovery progress, which remains private unless the employee chooses to share.
Building Organizational Resilience
Beyond individual case management, organizations benefit from systematic approaches to mental health promotion and depression prevention. Resilience programs develop employee capacity to navigate stress, maintain perspective during challenges, and access support networks proactively.
The American Psychiatric Association’s workplace resources emphasize prevention through organizational culture change rather than reactive intervention alone. Organizations with strong mental health cultures report lower depression rates, reduced absenteeism, and higher employee engagement.
Evidence-Based Prevention Strategies
Research-informed prevention programs address multiple organizational levels simultaneously. Individual skill-building combines with manager training, policy development, and environmental modifications to create comprehensive support systems.
Effective prevention components:
- Stress management and cognitive resilience training for all employees
- Manager development in supportive leadership practices
- Workload monitoring and redistribution protocols
- Regular workplace wellbeing assessments
- Peer support networks and mental health champion programs
Training delivered through platforms like specialized online courses ensures consistency while allowing employees to engage at their own pace. Australian organizations can access region-specific programs through localized providers that address cultural and regulatory contexts.
The Role of Occupational Health in Depression Management
Occupational health professionals play crucial roles in addressing depression in the workplace, particularly in larger organizations. These specialists coordinate between treating clinicians, managers, and employees to facilitate appropriate accommodations while protecting confidentiality.
Medical directors and occupational health nurses assess fitness for duty, recommend workplace modifications, and monitor return-to-work transitions. Their expertise ensures that medical recommendations translate into practical workplace applications without compromising employee privacy or organizational functioning.
Studies examining the role of corporate medical directors highlight the importance of occupational health interventions in reducing both individual suffering and organizational costs. These professionals bridge clinical and organizational perspectives, ensuring interventions address both health outcomes and workplace functionality.
Integrating Clinical and Workplace Support
Effective depression management requires coordination between clinical treatment and workplace support. While managers should never involve themselves in treatment decisions, they can facilitate communication between occupational health professionals and treating clinicians when employees provide consent.
This integration ensures that workplace accommodations align with treatment recommendations, return-to-work timelines reflect recovery progress, and employees receive consistent messaging about expectations and support availability. Clear protocols defining roles, responsibilities, and communication channels prevent confusion while protecting confidentiality.
Measuring Impact and Continuous Improvement
Organizations committed to addressing depression in the workplace establish metrics that track both process implementation and outcome achievement. Leading indicators include manager training completion rates, EAP utilization patterns, and accommodation request trends. Lagging indicators encompass absenteeism rates, turnover statistics, and productivity measures.
The World Federation for Mental Health emphasizes the importance of monitoring cognitive symptoms specifically, as these most directly impact workplace performance. Regular assessment enables organizations to refine programs based on effectiveness data rather than assumptions.
Key performance indicators for workplace mental health programs:
- Percentage of managers completing mental health literacy training
- Time from employee disclosure to accommodation implementation
- Successful return-to-work rates following mental health leave
- Employee perception of psychological safety (survey data)
- Changes in absenteeism and presenteeism rates
- EAP engagement and satisfaction scores
Dashboards tracking these metrics inform strategic decisions about resource allocation, program expansion, and continuous improvement priorities. Organizations demonstrating commitment through measurement signal to employees that mental health initiatives represent genuine priorities rather than superficial gestures.
Cultural Considerations and Inclusive Approaches
Depression in the workplace affects diverse populations differently based on cultural background, generational factors, and individual circumstances. Younger employees may discuss mental health more openly than older colleagues, while cultural backgrounds influence help-seeking behaviors and symptom expression.
Inclusive mental health programs acknowledge these differences through culturally responsive resources, diverse representation in mental health champions, and multiple access points for support. Some employees prefer digital resources, others value peer support, while some require professional clinical intervention.
Language accessibility, cultural competence in EAP providers, and awareness of how depression manifests across different populations enhance program effectiveness. Organizations serving diverse workforces should regularly evaluate whether mental health resources reach and resonate with all employee groups equitably.
Training programs that incorporate cultural competence alongside clinical knowledge prepare managers to support diverse teams effectively. Video resources available through workplace mental health channels often model these inclusive approaches through varied scenarios and perspectives.
Addressing depression in the workplace requires systematic approaches that combine leadership skill development, supportive policies, and organizational culture change. The evidence demonstrates that organizations investing in comprehensive mental health programs achieve measurable improvements in employee wellbeing, performance outcomes, and organizational effectiveness. Workplace Mental Health Institute provides the specialized training, assessment tools, and strategic consultation that enable organizations to develop these capabilities systematically, moving from awareness to meaningful action that supports both people and performance.


