Organizations today face mounting pressure to address psychological wellbeing systematically, yet many struggle to translate good intentions into actionable frameworks. A robust mental health policy workplace initiative serves as the foundation for creating psychologically safe environments while meeting legal obligations and business objectives. This comprehensive guide examines how leaders and HR professionals can design, implement, and sustain policies that genuinely improve workforce mental health rather than simply checking compliance boxes.
Understanding Mental Health Policy in Organizational Context
A mental health policy workplace framework differs fundamentally from generic wellness initiatives. While wellness programs often focus on individual lifestyle choices, comprehensive policies address systemic factors that influence psychological health across the organization.
Defining Policy Scope and Objectives
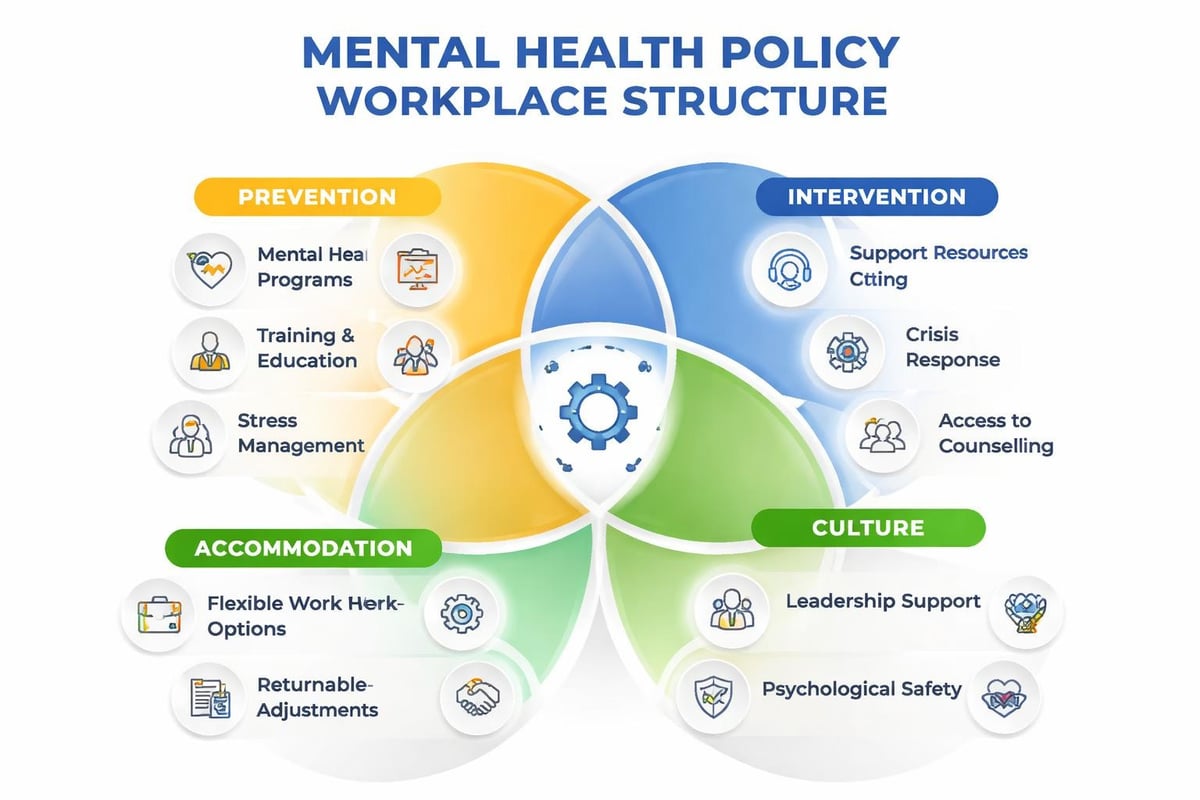
Effective policies establish clear boundaries around what the organization commits to providing and what falls outside its responsibility. Policy scope typically encompasses prevention strategies, early intervention protocols, accommodation procedures, return-to-work processes, and manager responsibilities.
The World Health Organization emphasizes that workplace mental health interventions must address both individual support and organizational conditions. Organizations should define measurable objectives that align with both employee wellbeing and performance metrics.
Core policy objectives include:
- Reducing stigma through leadership modeling and communication
- Establishing accessible pathways to professional support
- Training managers in psychologically informed supervision
- Creating accommodation processes that balance individual needs with operational requirements
- Monitoring psychological hazards and implementing controls
Legal Obligations and Compliance Frameworks
Organizations must navigate complex legal landscapes when developing mental health policy workplace strategies. In the United States, the Americans with Disabilities Act (ADA), Family and Medical Leave Act (FMLA), and Occupational Safety and Health Act (OSH Act) create specific obligations around mental health conditions.
Legal obligations for managing mental health extend beyond simply avoiding discrimination. Employers must provide reasonable accommodations, protect confidentiality, and in many jurisdictions, actively prevent psychological harm.
Australian organizations face additional requirements under Work Health and Safety legislation, which explicitly recognizes psychosocial hazards. Workplace Mental Health Institute Australia provides region-specific guidance for navigating these frameworks.
| Legal Framework | Primary Requirements | Policy Implications |
|---|---|---|
| ADA (US) | Reasonable accommodations, anti-discrimination | Clear accommodation request processes, confidentiality protocols |
| FMLA (US) | Protected leave for health conditions | Leave administration procedures, communication guidelines |
| WHS (Australia) | Psychosocial hazard identification and control | Risk assessment protocols, preventive measures |
| GDPR/Privacy Laws | Data protection for health information | Strict confidentiality standards, limited disclosure |
Building Evidence-Based Policy Components
The most effective mental health policy workplace initiatives incorporate multiple intervention levels, from organizational redesign to individual support pathways.
Prevention-Focused Organizational Strategies
Primary prevention addresses root causes of psychological distress before problems emerge. This requires examining work design, job demands, autonomy, recognition systems, and interpersonal dynamics.
Organizational-level interventions include:
- Workload management systems that prevent chronic overload
- Role clarity frameworks reducing ambiguity and conflict
- Participatory decision-making processes enhancing control
- Recognition programs acknowledging contributions meaningfully
- Conflict resolution protocols addressing interpersonal issues early
Research demonstrates that organizational interventions produce more sustainable outcomes than individual-focused programs alone. The WHO guidelines on mental health at work recommend combining both approaches for maximum impact.
Manager Training and Capability Development
Managers serve as critical implementation points for mental health policy workplace frameworks. Without adequate preparation, even well-designed policies fail during frontline application.
Effective manager training moves beyond awareness to build specific capabilities:
- Recognizing early indicators of psychological distress without diagnosing
- Conducting supportive conversations using psychologically informed approaches
- Implementing accommodations within operational constraints
- Managing confidentiality while coordinating necessary support
- Maintaining boundaries between support and clinical intervention
Workplace Mental Health Institute specializes in manager training that emphasizes practical skills over theoretical knowledge. Their programs focus on confidence-building through scenario-based learning rather than simply information transfer.
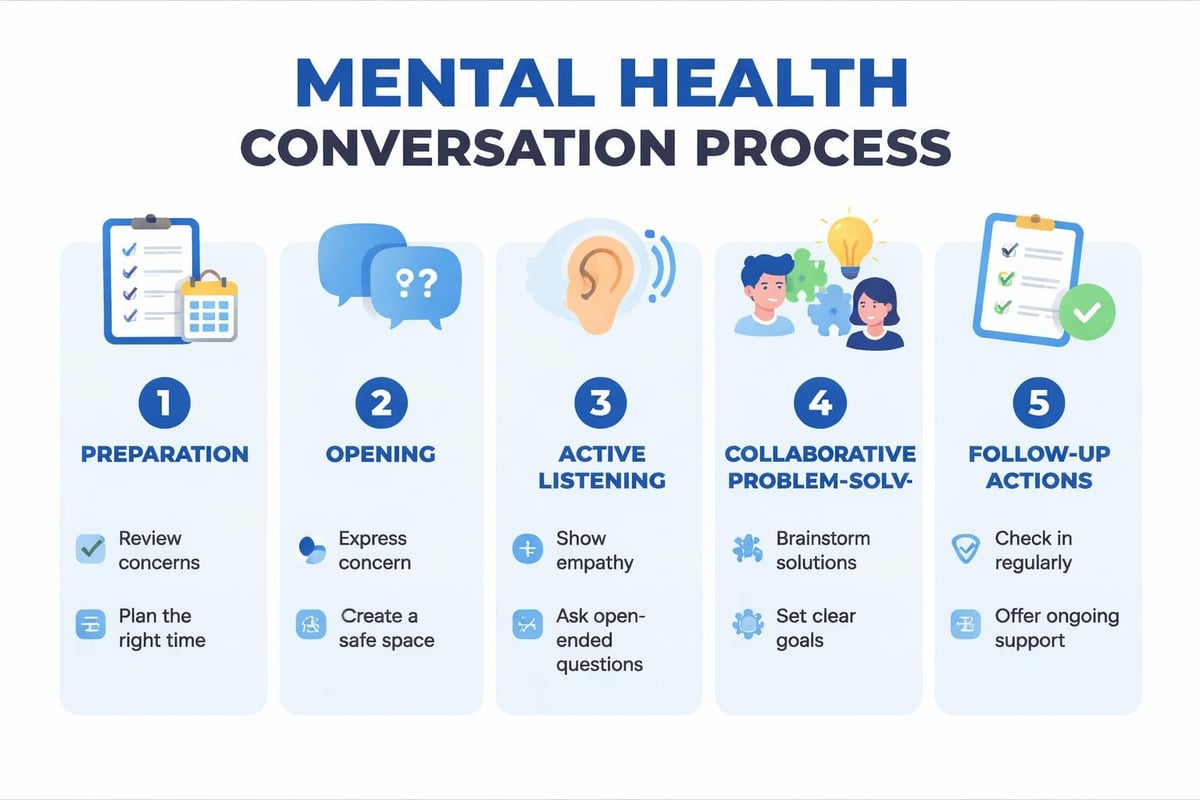
Implementation Strategies That Drive Adoption
Policy documents alone rarely change organizational culture. Implementation requires deliberate change management strategies that address both structural and cultural dimensions.
Stakeholder Engagement and Co-Design
Involving diverse stakeholders during policy development increases both quality and buy-in. Effective co-design processes include representatives from:
- Senior leadership (ensuring resource commitment)
- HR and legal teams (addressing compliance requirements)
- Frontline managers (incorporating implementation realities)
- Employee representatives (reflecting worker perspectives)
- Health and safety committees (integrating existing frameworks)
Co-design benefits:
- Identifies implementation barriers early
- Builds ownership across organizational levels
- Incorporates diverse perspectives on psychological safety
- Creates internal champions for policy adoption
Communication Cascades and Cultural Integration
Mental health policy workplace implementation succeeds when communication extends beyond initial announcements to ongoing cultural integration.
| Communication Phase | Key Messages | Delivery Methods |
|---|---|---|
| Launch | Policy rationale, leadership commitment, available resources | Town halls, video messages, written materials |
| Education | Specific procedures, manager responsibilities, employee rights | Training sessions, quick reference guides, FAQs |
| Normalization | Success stories, reduced stigma, ongoing support | Regular updates, testimonials, leader modeling |
| Sustainment | Policy updates, impact metrics, continuous improvement | Annual reviews, feedback mechanisms, refresher training |
Leadership visibility proves particularly crucial. When executives openly discuss mental health, share personal experiences, or visibly utilize policy provisions, permission structures shift dramatically.
Measurement Frameworks and Continuous Improvement
What gets measured gets managed. Comprehensive mental health policy workplace strategies include both leading indicators (policy utilization) and lagging indicators (outcomes).
Leading indicators to monitor:
- Manager training completion rates
- Accommodation request volumes and processing times
- Employee Assistance Program (EAP) utilization
- Policy awareness survey results
- Participation in wellbeing initiatives
Lagging indicators revealing impact:
- Absenteeism and presenteeism trends
- Workers' compensation claims for psychological injury
- Turnover rates, particularly among high performers
- Employee engagement and satisfaction scores
- Productivity metrics and performance indicators
The WHO guidance on workplace mental health policies recommends establishing baseline measurements before policy implementation to enable meaningful evaluation.
Addressing Common Implementation Challenges
Even well-designed mental health policy workplace frameworks encounter predictable obstacles during implementation.
Managing Confidentiality While Coordinating Support
Organizations must balance confidentiality obligations with operational needs to coordinate accommodations and support. This tension creates particular challenges when multiple parties (managers, HR, occupational health) need information to fulfill their responsibilities.
Best practices include:
- Establishing clear consent processes for information sharing
- Limiting disclosures to the minimum necessary for accommodation
- Training all parties on confidentiality obligations
- Creating secure systems for health information storage
- Separating medical information from personnel files
Managers need sufficient information to implement accommodations without requiring clinical details about diagnoses or treatment.
Preventing Policy Abuse While Maintaining Accessibility
Some organizations struggle with concerns about employees exploiting mental health policies. However, restricting access based on these fears typically causes greater harm than occasional misuse.
Creating reasonable safeguards without imposing barriers requires:
- Clear eligibility criteria based on functional impact rather than diagnosis
- Documented processes without excessive bureaucracy
- Regular review of accommodations with flexibility for changes
- Consistent application across all employees
- Focus on outcomes rather than presenteeism
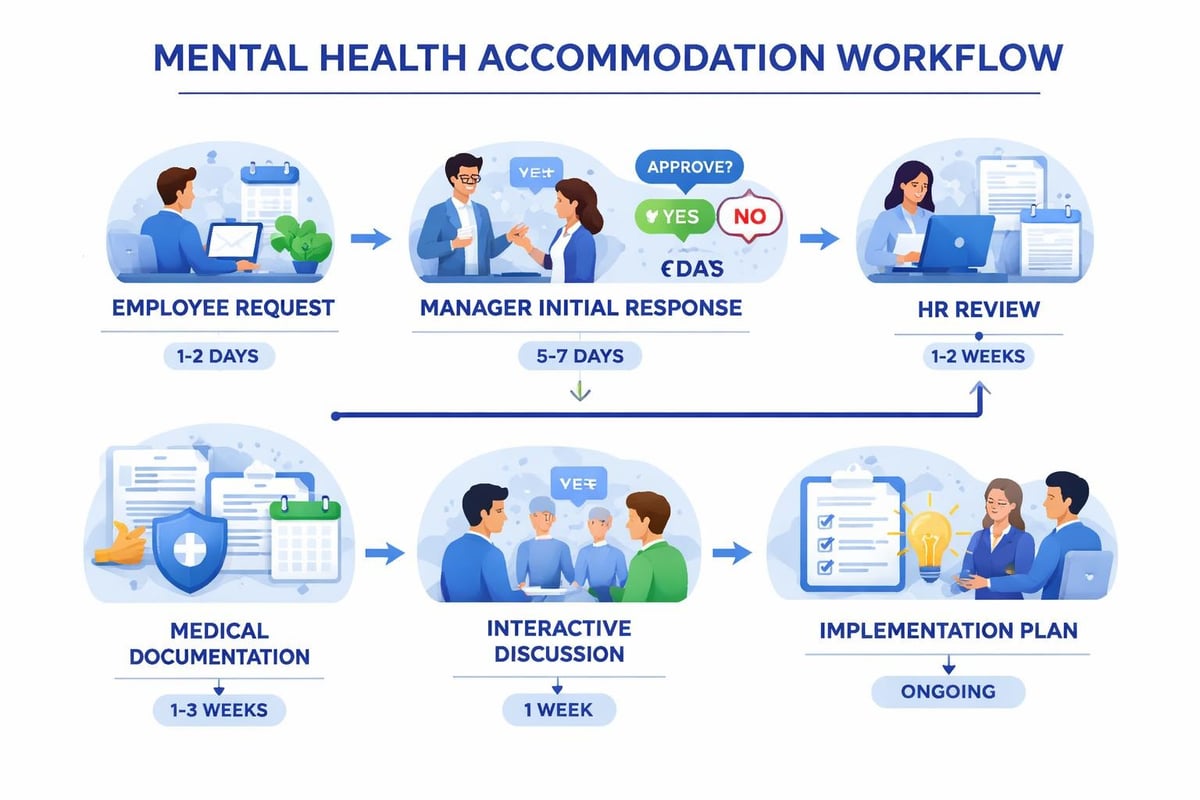
Building Psychological Safety for Disclosure
Policies fail when employees fear career consequences from disclosure. Building genuine psychological safety requires addressing power dynamics, establishing accountability, and demonstrating consistent support.
Strategies for enhancing safety:
- Anti-retaliation provisions with clear enforcement
- Anonymous reporting mechanisms for policy violations
- Leadership storytelling that normalizes mental health challenges
- Visible support for employees who disclose
- Career progression data showing no adverse impact from accommodation use
Training programs from Workplace Mental Health Institute’s online platform equip managers to respond supportively rather than defensively when employees disclose mental health concerns.
Specialized Policy Considerations for High-Risk Roles
Certain occupations face elevated psychological risks requiring tailored mental health policy workplace provisions.
Trauma-Exposed Workforces
First responders, healthcare workers, social services personnel, and others regularly exposed to traumatic material need specialized support structures.
Essential policy elements include:
- Pre-incident preparation through trauma-informed training
- Immediate post-incident support including psychological first aid
- Peer support programs leveraging shared occupational experience
- Access to specialized treatment for trauma-related conditions
- Return-to-work protocols following critical incidents
Organizations should implement routine psychological screening without pathologizing normal stress responses or creating barriers to disclosure.
High-Consequence Decision Makers
Roles involving high-stakes decisions under pressure (aviation, healthcare, finance) require balancing safety obligations with individual support.
Policy frameworks must address:
- Fitness-for-duty assessments that protect safety while respecting rights
- Graduated return-to-work for safety-critical positions
- Peer review processes that identify concerning patterns early
- Alternative duties during recovery when appropriate
- Clear criteria for when and how to restrict duties
These provisions work best when developed collaboratively with professional associations and unions rather than imposed unilaterally.
Integration With Broader Wellbeing Strategies
Mental health policy workplace initiatives achieve greater impact when integrated with comprehensive wellbeing approaches rather than operating as standalone programs.
Connecting Physical and Psychological Health
The artificial separation between physical and mental health creates gaps in support. Integrated policies recognize that:
- Chronic physical conditions significantly impact psychological wellbeing
- Mental health conditions manifest through physical symptoms
- Recovery from any health condition involves both dimensions
- Accommodation needs often cross physical-psychological boundaries
Integration strategies include:
- Single accommodation request process for all health conditions
- Cross-training between occupational health and EAP providers
- Coordinated return-to-work planning across condition types
- Holistic wellbeing assessments addressing multiple dimensions
Aligning With Diversity, Equity, and Inclusion Initiatives
Mental health experiences and help-seeking behaviors vary significantly across demographic groups. Culturally responsive policies acknowledge these differences while maintaining equitable access.
Considerations include:
- Cultural variations in mental health conceptualization and symptom expression
- Disparate impacts of workplace stressors across identity groups
- Barriers to accessing support among marginalized populations
- Representation in policy development and program design
- Tailored communication strategies for diverse audiences
The WHO European guidance on promoting mental health emphasizes the importance of addressing social determinants and reducing health inequities through workplace interventions.
Sustaining Policy Effectiveness Over Time
Initial policy implementation represents only the beginning of long-term cultural change. Sustaining effectiveness requires ongoing attention, adaptation, and renewal.
Regular Policy Review and Updates
Mental health policy workplace frameworks should undergo formal review every 2-3 years, with interim updates as needed based on:
- Changes in legal requirements or regulatory guidance
- Emerging research on effective interventions
- Internal evaluation data showing gaps or opportunities
- Workforce demographic shifts or organizational restructuring
- Stakeholder feedback on policy barriers or improvements
Review processes should examine:
| Review Element | Assessment Questions | Data Sources |
|---|---|---|
| Utilization | Who accesses policy provisions? Who doesn't? Why? | Usage data, employee surveys, focus groups |
| Effectiveness | Are outcomes improving? Where are persistent gaps? | Health metrics, performance data, incident reports |
| Accessibility | Do processes create unnecessary barriers? | Process mapping, user experience research |
| Cultural Integration | Is mental health normalized or stigmatized? | Climate surveys, manager feedback |
| Resource Adequacy | Do available supports meet demand? | Wait times, capacity analysis, needs assessment |
Building Internal Expertise and Capacity
External consultants play valuable roles in policy development, but sustainable implementation requires building internal capability.
Organizations should develop:
- Internal champions at multiple organizational levels
- Communities of practice for managers supporting employees
- Peer support networks leveraging lived experience
- HR specialization in psychological accommodation and support
- Leadership competencies in psychologically informed management
Video resources from Workplace Mental Health Institute’s YouTube channel provide accessible ongoing education to supplement formal training programs.
Celebrating Progress While Maintaining Momentum
Recognition of improvements sustains engagement while acknowledging ongoing challenges prevents complacency.
Effective celebration strategies:
- Sharing aggregated outcome data showing positive trends
- Highlighting specific examples of policy impact (with permission)
- Recognizing teams or leaders demonstrating excellent implementation
- Communicating research contributions or industry leadership
- Connecting improvements to organizational values and mission
Balanced messaging acknowledges progress without declaring premature victory, maintaining focus on continuous improvement rather than compliance achievement.
Developing comprehensive mental health policy workplace frameworks represents both a legal imperative and a strategic opportunity to build resilient, high-performing organizations. Success requires moving beyond compliance thinking to genuine cultural integration where psychological wellbeing becomes embedded in how work gets done. Workplace Mental Health Institute partners with organizations to design evidence-based policies and build the internal capabilities needed for effective implementation, offering specialized training, strategic consultation, and ongoing support that translates policy documents into meaningful workplace change.


