Mental health awareness topics have evolved from peripheral concerns to central pillars of organizational strategy. Leaders and HR professionals now recognize that understanding these topics directly impacts employee retention, productivity, and workplace culture. This comprehensive guide examines the most critical mental health awareness topics for modern workplaces, providing evidence-based frameworks that managers and decision-makers can implement immediately. These topics represent not merely concepts to acknowledge during awareness campaigns, but actionable areas requiring sustained attention and organizational commitment throughout the year.
Understanding Core Mental Health Awareness Topics in Professional Settings
Mental health awareness topics encompass a broad spectrum of conditions, experiences, and interventions that affect workplace populations. Rather than treating these as isolated issues, effective organizations recognize them as interconnected elements of a comprehensive wellbeing strategy.
Defining Mental Health in Workplace Contexts
Mental health extends beyond the absence of diagnosable conditions. According to the World Health Organization, mental health represents a state of wellbeing where individuals realize their abilities, cope with normal life stresses, work productively, and contribute to their communities. In workplace settings, this definition translates to employees who can engage meaningfully with their roles, navigate challenges constructively, and maintain psychological resilience under professional demands.
Organizations often conflate mental health awareness with mental illness education, but this represents only one dimension. Comprehensive mental health awareness topics include:
- Preventive strategies that build resilience before crises emerge
- Early intervention frameworks that identify concerns at nascent stages
- Supportive environments that reduce stigma and encourage help-seeking
- Systemic factors including workload management, autonomy, and psychological safety
- Recovery-oriented approaches that support employees returning from mental health challenges
The Business Case for Mental Health Topic Proficiency
Research demonstrates that organizations with sophisticated understanding of mental health awareness topics experience measurable advantages. Employees in psychologically healthy workplaces report higher engagement, lower absenteeism, and stronger organizational commitment. The National Institute of Mental Health emphasizes that mental health conditions affect productivity across all industries, making awareness not a discretionary investment but a fundamental business requirement.

Prevalent Conditions Requiring Organizational Awareness
Leaders must understand the mental health conditions most commonly affecting their workforce. This knowledge enables appropriate policy development, accommodation strategies, and resource allocation.
Depression and Anxiety Disorders in Professional Populations
Depression and anxiety represent the most prevalent mental health conditions in workplace settings. These conditions manifest differently across individuals but share common workplace impacts including concentration difficulties, decision-making challenges, and interpersonal strain.
Depression symptoms in professional contexts often include:
- Persistent fatigue despite adequate rest
- Reduced interest in previously engaging work
- Difficulty concentrating on complex tasks
- Withdrawal from team interactions
- Increased irritability or emotional flatness
Anxiety disorders, meanwhile, may present through excessive worry about performance, physical symptoms including tension headaches, avoidance of certain work situations, or hypervigilance to perceived threats. The National Alliance on Mental Illness provides extensive resources on recognizing these conditions and understanding their workplace manifestations.
| Condition Type | Workplace Indicators | Support Approaches |
|---|---|---|
| Major Depression | Missed deadlines, withdrawn behavior, decreased quality | Flexible scheduling, workload adjustment, EAP referral |
| Generalized Anxiety | Perfectionism, difficulty delegating, physical symptoms | Clear expectations, regular check-ins, stress management training |
| Panic Disorder | Sudden absences, avoidance of meetings, physical complaints | Accommodation planning, gradual exposure support, crisis protocols |
| Social Anxiety | Limited participation, email preference, isolation | Structured communication options, smaller team settings, skill building |
Burnout as a Distinct Mental Health Awareness Topic
While not classified as a mental illness, burnout constitutes a critical mental health awareness topic requiring organizational attention. Burnout develops through chronic workplace stress that has not been successfully managed, characterized by emotional exhaustion, cynicism toward work, and reduced professional efficacy.
Organizations addressing burnout must examine systemic factors rather than treating it as individual weakness. Contributing elements include unrealistic workload expectations, insufficient autonomy, unclear role definitions, lack of recognition, and toxic workplace dynamics. Effective interventions require leadership commitment to structural change, not merely resilience training for affected employees.
Trauma-Informed Approaches in Workplace Mental Health
Trauma-informed care has emerged as an essential mental health awareness topic, particularly as organizations recognize that many employees have experienced significant adverse events. This approach reshapes how organizations design policies, interactions, and support systems.
Principles of Trauma-Informed Workplace Practices
Trauma-informed workplaces operate from understanding that traumatic experiences are common, that they affect behavior and functioning in identifiable ways, and that organizational practices can either support recovery or inadvertently re-traumatize individuals. The Substance Abuse and Mental Health Services Administration outlines core principles including safety, trustworthiness, peer support, collaboration, empowerment, and cultural sensitivity.
Practical applications include:
- Reviewing policies through a trauma lens to identify potentially triggering practices
- Training managers to recognize trauma responses without requiring disclosure
- Creating predictable processes that reduce uncertainty and anxiety
- Offering choice and control wherever possible in work arrangements
- Building peer support networks that reduce isolation
Recognizing Trauma Responses in Professional Settings
Trauma manifests through various responses that leaders often misinterpret as performance issues or attitude problems. Hypervigilance, emotional dysregulation, difficulty with authority relationships, or sudden performance changes may reflect trauma responses rather than capability deficits.
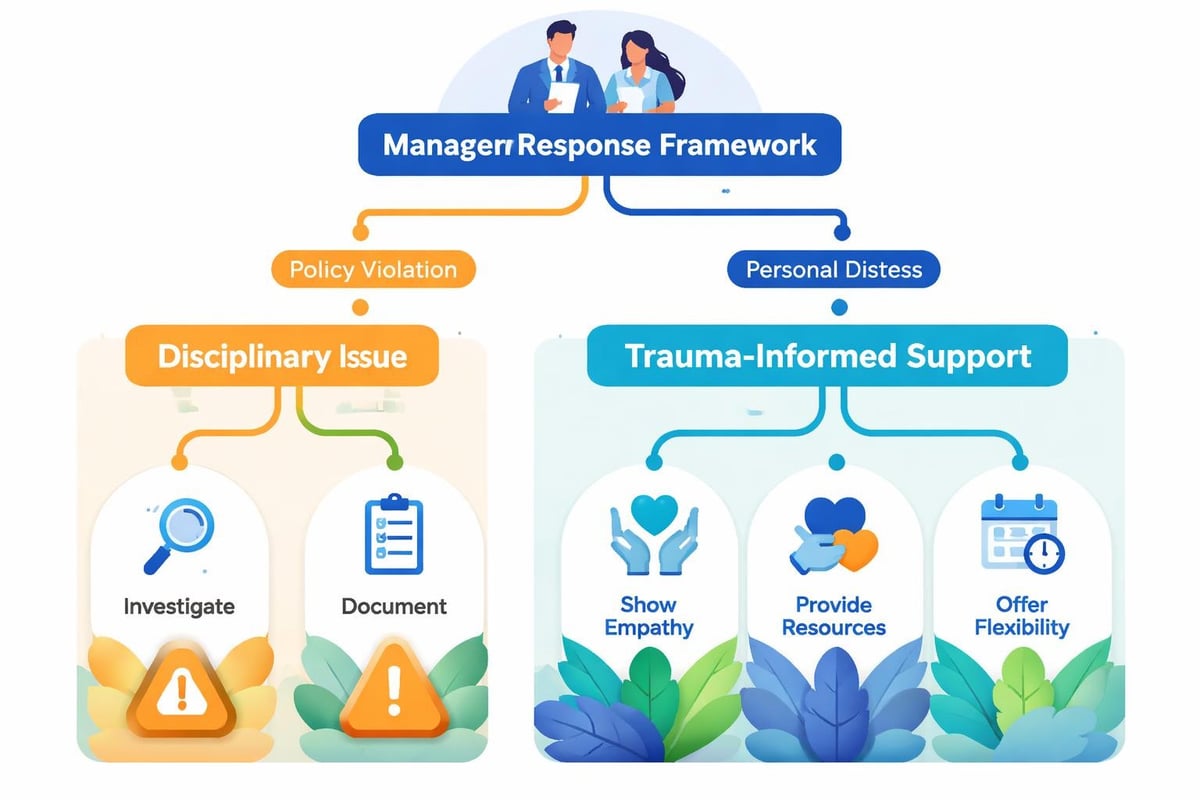
Managers equipped to recognize these patterns can respond with appropriate support referrals rather than punitive measures. This requires training that builds psychological literacy without expecting managers to become therapists. Organizations like Workplace Mental Health Institute specialize in developing this capability through evidence-based training programs.
Suicide Prevention as a Workplace Responsibility
Suicide prevention represents one of the most critical mental health awareness topics, yet many organizations avoid addressing it due to discomfort or fear of legal liability. This avoidance leaves employees vulnerable when workplace factors contribute to suicidal ideation or when warning signs emerge in professional settings.
Creating Safety Nets Through Awareness and Training
Effective suicide prevention requires multiple organizational layers. Awareness campaigns reduce stigma and normalize help-seeking. Training equips managers and peers to recognize warning signs and respond appropriately. Clear protocols establish response pathways when concerns arise. According to Mental Health America, comprehensive approaches significantly reduce risk by creating multiple intervention opportunities.
Warning signs that trained observers can identify include:
- Verbal statements about feeling hopeless or being a burden
- Sudden mood improvements after prolonged depression (suggesting decision resolution)
- Increased risk-taking or reckless behavior
- Withdrawal from relationships and activities
- Giving away possessions or finalizing affairs
- Researching methods or acquiring means
Response Protocols for Workplace Suicide Risk
Organizations need clear, practiced protocols for responding when suicide risk emerges. This includes immediate response procedures, connection to professional resources, follow-up support, and postvention strategies if a death occurs. Many organizations partner with Employee Assistance Programs or mental health providers to ensure appropriate expertise guides these responses.
Documentation requirements must balance duty of care with privacy considerations. Legal counsel should review protocols to ensure they meet regulatory obligations while respecting employee rights. Training should emphasize that responding to suicide risk differs fundamentally from managing performance issues.
Stress Management and Resilience Building
Stress management constitutes a foundational mental health awareness topic because chronic stress precedes many mental health conditions. Organizations that address stress proactively reduce both individual suffering and downstream organizational costs.
Individual Versus Organizational Stress Interventions
Historically, workplace stress interventions focused exclusively on individual skill-building: teaching employees relaxation techniques, time management, or cognitive reframing. While these skills have value, exclusive focus on individual adaptation implicitly blames employees for stress generated by organizational design.
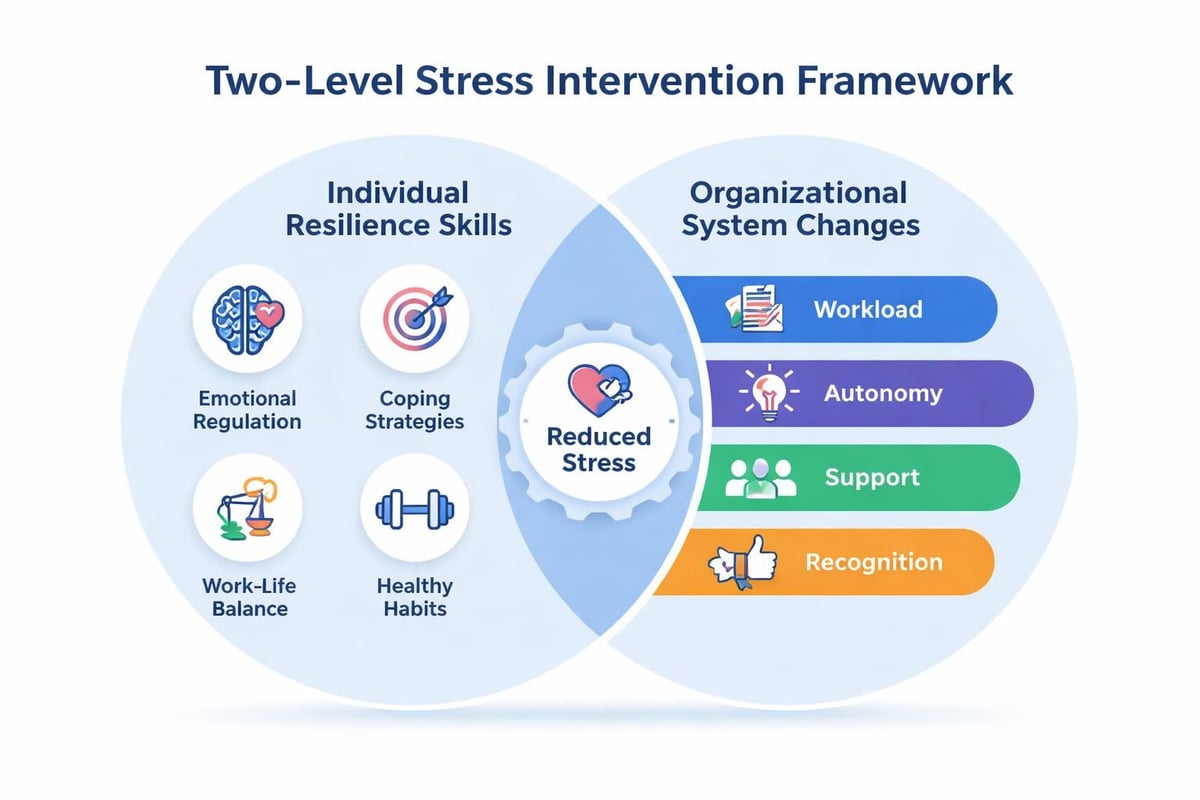
Comprehensive stress management addresses both levels:
Individual interventions include:
- Evidence-based stress reduction techniques
- Sleep hygiene and recovery strategies
- Boundary-setting skills
- Emotional regulation capabilities
Organizational interventions include:
- Workload audits and redistribution
- Role clarity improvements
- Decision authority alignment
- Recognition and appreciation systems
- Flexibility in work arrangements
Research consistently demonstrates that organizational interventions produce larger, more sustained effects than individual training alone. Effective programs combine both approaches, positioning individual skills as tools for navigating unavoidable stressors while simultaneously reducing preventable organizational stressors.
Building Psychological Resilience in Teams
Resilience training helps employees maintain wellbeing and performance during adversity. Effective programs teach specific, evidence-based capabilities rather than vague exhortations to "stay positive." Components include realistic optimism, behavioral activation, social connection, values clarification, and growth mindset development.
Team-based resilience building offers advantages over purely individual approaches. Teams develop shared language for discussing challenges, normalize help-seeking, and create mutual support systems. Leaders model resilience practices, demonstrating that these capabilities enhance rather than conflict with high performance. Organizations seeking structured programs can explore options through specialized training platforms that deliver consistent, scalable content.
Substance Use and Workplace Mental Health
Substance use disorders intersect significantly with other mental health awareness topics, yet organizations often address them through separate, punitive frameworks rather than integrating them into comprehensive mental health strategies.
Understanding Co-Occurring Conditions
Substance use frequently co-occurs with depression, anxiety, trauma, and other mental health conditions. Individuals may use substances to self-medicate distressing symptoms or may develop mental health symptoms as consequences of substance use. This interconnection requires integrated support approaches rather than sequential treatment.
Workplace policies traditionally emphasized detection and discipline, creating environments where employees hid problems until they became severe. Progressive organizations now emphasize early intervention, confidential support, and recovery-oriented accommodations. This shift requires training managers to distinguish between performance management issues and indicators suggesting support referrals.
| Approach Element | Traditional Model | Evidence-Based Model |
|---|---|---|
| Primary Focus | Detection and discipline | Prevention and early support |
| Manager Role | Enforcement and documentation | Observation and referral |
| Employee Response | Concealment and fear | Earlier help-seeking |
| Return to Work | Probationary monitoring | Graduated support and accommodation |
| Outcome Measure | Rule compliance | Sustained recovery and performance |
Creating Recovery-Supportive Workplaces
Employees in recovery from substance use disorders benefit from workplace cultures that understand recovery as an ongoing process requiring sustained support. This includes flexible scheduling for treatment appointments, peer support opportunities, and managers trained to provide appropriate encouragement without overstepping boundaries.
Organizations should review policies for unintentional barriers to recovery support. Many policies designed decades ago reflect outdated understanding of addiction and recovery. Modern approaches align with evidence from addiction science while maintaining appropriate performance expectations.
Psychological Safety and Organizational Culture
Psychological safety, the belief that one can speak up without punishment or humiliation, represents a foundational mental health awareness topic affecting all other initiatives. Without psychological safety, awareness campaigns, training programs, and support resources underperform because employees fear consequences of acknowledging struggles.
Building Cultures Where Mental Health Topics Are Discussable
Leaders create psychological safety through consistent behaviors demonstrating that vulnerability is acceptable and that raising concerns leads to support rather than judgment. This requires sustained effort across multiple organizational levels, not singular training events or awareness days.
Concrete practices include:
- Leader disclosure of their own mental health experiences or support-seeking
- Responding to concerns with curiosity rather than defensiveness
- Separating performance conversations from wellbeing discussions
- Acknowledging systemic contributors to stress rather than blaming individuals
- Celebrating help-seeking as strength and wisdom
Research by Active Minds demonstrates that stigma remains the primary barrier preventing individuals from accessing mental health support. Organizations that systematically reduce stigma through psychological safety initiatives see increased help-seeking, earlier intervention, and improved outcomes.
Measuring and Monitoring Organizational Mental Health Climate
Organizations serious about mental health awareness topics implement regular assessment of their mental health climate. This extends beyond counting EAP utilization to examining workplace factors affecting mental health, employee perceptions of support availability, and manager capability in responding to concerns.
Assessment approaches include employee surveys measuring psychological safety and mental health climate, focus groups exploring experiences with support systems, analysis of absence patterns and turnover data, and manager self-assessment of mental health response confidence. Data should inform targeted improvements rather than serving merely as report metrics.
For organizations in Australia seeking localized support and assessment tools, regional specialists provide culturally adapted frameworks aligned with Australian workplace contexts and regulatory requirements.
Early Intervention and Help-Seeking Promotion
Early intervention represents one of the highest-value mental health awareness topics because treatment effectiveness increases significantly when conditions are addressed at early stages. Yet organizational cultures often inadvertently discourage early help-seeking through stigma, workload pressures, or fear of career consequences.
Designing Systems That Enable Early Support Access
Effective early intervention systems reduce barriers to accessing help through multiple mechanisms. This includes ensuring employees know what resources exist, communicating that using resources carries no negative consequences, designing resources that fit into work schedules, and creating financial accessibility.
Many organizations assume that simply offering an Employee Assistance Program satisfies early intervention requirements. However, EAP utilization typically ranges between 3-8% annually, suggesting that either mental health needs are dramatically lower than population prevalence data indicates, or significant barriers prevent access. Investigation typically reveals the latter.
Barrier reduction strategies include:
- Multiple access pathways including self-referral, manager referral, and peer referral
- Clear communication about confidentiality protections and their limitations
- Flexible timing for appointments and follow-up
- Reduced administrative complexity in accessing services
- Manager training on making supportive referrals without overstepping
Training Managers as First Responders
Managers serve as the organizational front line for identifying emerging mental health concerns. Employees experiencing difficulties typically display observable changes in behavior, performance, or presentation before seeking formal help. Managers who recognize these changes and respond supportively can facilitate earlier intervention.
Effective training equips managers to notice changes, express appropriate concern, listen without diagnosing, refer to appropriate resources, and follow up supportively. Training should clarify role boundaries, emphasizing that managers facilitate access to professional support rather than providing therapy or diagnosing conditions. Video resources, such as those available through the Workplace Mental Health Institute YouTube channel, can supplement formal training with accessible refresher content.
Specific Population Considerations
Mental health awareness topics must account for the reality that different populations experience distinct challenges and may require tailored approaches to support.
Generational Differences in Mental Health Experience and Expression
Younger employees often demonstrate greater openness discussing mental health, having grown up with reduced stigma and increased awareness. This creates both opportunities and challenges for organizations. Opportunities include leveraging younger employees' willingness to normalize mental health conversations. Challenges include ensuring support systems meet diverse needs across age groups and preventing assumptions that older employees require less support simply because they discuss mental health less frequently.
Organizations should avoid stereotyping generations while acknowledging general patterns. Tailored communication strategies may increase effectiveness across different age cohorts without creating entirely separate systems.
Cultural Considerations in Mental Health Awareness
Cultural background significantly influences how individuals experience, express, and respond to mental health challenges. Some cultures emphasize collective over individual wellbeing, others prioritize stoicism or view mental health struggles as private family matters rather than workplace concerns.
Culturally responsive organizations recognize this diversity without essentializing or stereotyping. This includes offering varied support modalities, training managers in cultural humility, ensuring diverse representation in mental health resources and imagery, and partnering with culturally specific organizations when developing targeted initiatives.
Resources from MentalHealth.gov provide information on cultural considerations in mental health support, helping organizations develop more inclusive approaches.
Implementation Framework for Mental Health Awareness
Understanding mental health awareness topics intellectually differs fundamentally from implementing organizational change based on that understanding. Effective implementation requires strategic planning, stakeholder engagement, resource allocation, and sustained leadership commitment.
Conducting Organizational Readiness Assessments
Before launching major mental health initiatives, assess current organizational capacity, existing resources, leadership commitment, employee needs, and cultural readiness. This assessment prevents implementing programs misaligned with organizational context or attempting sophisticated interventions without necessary foundational elements.
Assessment components include:
- Policy audit identifying existing mental health-related policies and gaps
- Stakeholder interviews with leadership, HR, managers, and employees
- Resource inventory cataloging current programs, benefits, and support systems
- Culture evaluation measuring psychological safety and stigma levels
- Needs analysis identifying priority mental health awareness topics for the specific workforce
Results inform strategic planning that sequences interventions appropriately, builds on existing strengths, addresses critical gaps, and aligns with organizational capacity.
Developing Multi-Year Mental Health Strategies
Sustainable progress on mental health awareness topics requires multi-year commitment rather than one-time initiatives. Effective strategies identify 3-5 year goals, establish annual objectives supporting those goals, define success metrics, allocate necessary resources, and assign clear accountability.
Strategic plans should integrate mental health across multiple organizational systems rather than treating it as an isolated HR initiative. Integration points include:
- Recruitment and onboarding incorporating mental health culture messaging
- Performance management separating wellbeing discussions from evaluation
- Learning and development building mental health literacy systematically
- Leadership development making psychological safety and support capability core competencies
- Operations and workflow design considering mental health impacts of processes
Developing organizational expertise across these mental health awareness topics requires sustained investment in training, policy development, and cultural transformation. The interconnected nature of these topics means that addressing any single area without attending to others produces limited results, while comprehensive approaches create synergistic improvements across employee wellbeing and organizational performance. Workplace Mental Health Institute provides the specialized training, assessment tools, and strategic consultation that enables organizations to translate awareness into measurable workplace improvements, building capabilities that protect and enhance employee mental health across all career stages.


